The appendix was long considered an odd little organ in the body. It was a potentially troublesome, rather redundant appendage to the lower colon of the intestinal tract, and biologists were baffled as to its true function. Recently there were suspicions that it may be playing a role in Parkinson’s disease. This week, however, new research suggests that this may not be the case.
We have previously discussed the idea that Parkinson’s may possibly start in the gut (click here to read more on this). Some in the research community suspect that there is a particular part of the gut where it may start: the Appendix.
What is the Appendix?
The human appendix is a small (averaging 9 cm in length) tube attached to the beginning of the large intestine. Most of us only ever think of the appendix when we are affected by it in the case of Appendicitis.
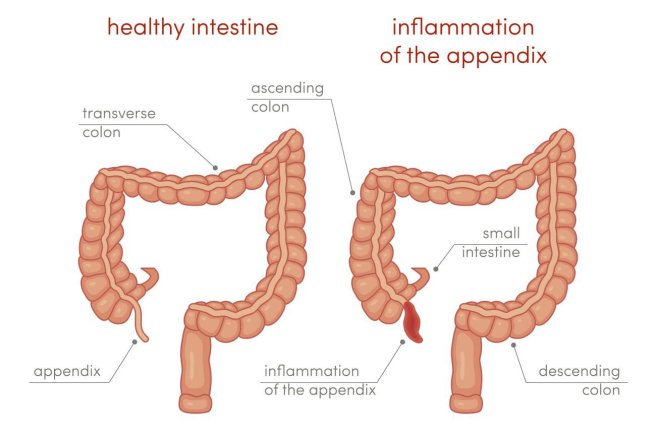
Source: Healthversed
The Appendix was long considered functionless, an oddity, and by some an mistake or accident of evolution. More recently, however, a new image has started to appear with regards to the appendix. And it has to do with the bacteria of the gut.
We have previously written about Helicobacter pylori and the possible associations with Parkinson’s disease, and in that post we discussed the wide variety of bacteria in the gut. These populations of bacteria are constantly changing, based on our interactions with the world around us (eg. what we are eating, geographically where we are, etc). The developing image of the appendix is that this small organ represents a safe house for bacteria, that is to say: ‘the appendix serves as a haven for useful bacteria when illness flushes those bacteria from the rest of the intestines’ (Wikipedia).
So what would this have to do with Parkinson’s disease?
We have previously discussed the idea that the gut may be one of the starting points for Parkinson’s disease. Many researchers believe that some unknown agent or causal factor is accessing the brain via the nerve fibers surrounding the gut. This theory is supported by reports that sectioning those nerves (to treat ulcers) can reduce your chance of Parkinson’s disease (click here for more on this).
When looking at the nerve fibres surrounding the intestinal system, one can not help but notice that the appendix is densely innervated. And this is why some researchers suspect that the appendix may be playing a role in Parkinson’s disease.
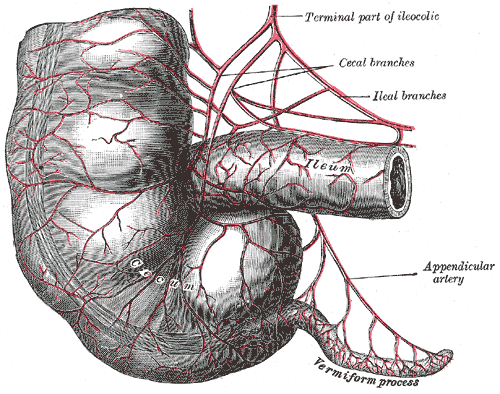
Blood vessels of the Appendix. Source: Wikipedia
What evidence exists for a connection between the Appendix and Parkinson’s disease?
In 2014, a group of research looked at tissue of the appendix from normal people and they found something interesting.

Title: Alpha-synuclein in the appendiceal mucosa of neurologically intact subjects.
Authors: Gray MT, Munoz DG, Gray DA, Schlossmacher MG, Woulfe JM.
Title: Mov Disord. 2014 Jul;29(8):991-8. doi: 10.1002/mds.25779. Epub 2013 Dec 18.
PMID: 24352892
The researchers looked at biopsies of the appendix from 20 normal people (no history of Parkinson’s disease). In all cases they found high levels of the Parkinson’s disease associated protein, Alpha synuclein (Click here to read more on this), in the nerve fibres surrounding the Appendix. When they looked at other areas of the intestinal system, they found little or no alpha synuclein.
This result got a lot of attention.
A group of researchers then took a large cohort of people with Parkinson’s disease and asked which of them had ever had an appendectomy (removal of the Appendix).

Title: Appendectomy may delay Parkinson’s disease Onset
Authors: Mendes A, Gonçalves A, Vila-Chã N, Moreira I, Fernandes J, Damásio J, Teixeira-Pinto A, Taipa R, Lima AB, Cavaco S.
Journal: Mov Disord. 2015 Sep;30(10):1404-7. doi: 10.1002/mds.26311. Epub 2015 Jul 30.
PMID: 26228745
Of the 295 people with Parkinson’s disease involved in the study, 34 were found to have had an appendectomy. There was no significant difference in age of onset across the entire group of people involved in the study, but in people with late onset Parkinson’s (after the age of 55 years) the authors found that found evidence that an appendectomy significantly delayed the onset of Parkinson’s symptoms.
This result led some researchers to conclude that the appendix may have some role in Parkinson’s disease.
What was found in the study this week?
Before you rush out and order yourself an appendectomy, please read the following – This week, any role of the Appendix in Parkinson’s disease has been called into question with the publication of this study:

Title: Appendectomy in mid and later life and risk of Parkinson’s disease: A population-based study.
Authors: Marras C, Lang AE, Austin PC, Lau C, Urbach DR.
Journal: Mov Disord. 2016 May 31. doi: 10.1002/mds.26670. [Epub ahead of print]
PMID: 27241338
The researchers involved in this study looked at the medical records of the 14 million residents of Ontario (Canada) who have health care insurance. They found 42,999 had undergone an appendectomy. When the researchers compared people with appendectomies with people without an appendectomy (the control group) and people who had a cholecystectomy (removal of the gallbladder – a surgical control group), they found no difference in the risk of Parkinson’s disease. The researchers concluded that their data did not support an association between mid to late life appendectomy and Parkinson’s disease.
These results are based on large numbers of people and it will be interesting to see how the research community reacts to them. We’ll keep you posted.
UPDATE (23/09/16): A new study came out last week from a group in Denmark that suggests Appendectomies ARE associated with a small increase in risk of developing Parkinson’s disease, but importantly this is only at 10 or more years post surgery.
Title: Appendectomy and risk of Parkinson’s disease: A nationwide cohort study with more than 10 years of follow-up.
Authors: Svensson E, Horváth-Puhó E, Stokholm MG, Sørensen HT, Henderson VW, Borghammer P.
Journal: Mov Disord. 2016 Sep 13.
PMID: 27621223
Today’s banner, illustrating the location of the Appendix was sourced from UCDenver
 Appendix. Source: journalofethics
Appendix. Source: journalofethics