|
# # # # Inflammation is the means by which tissue in our bodies communicate with the immune system to indicate when something is wrong. Tiny messenger proteins are released from stressed or damaged cells to alert neighbouring cells of their situation. Ailing cells can also release additional components – such as DNA – that can activate immune cells and cause inflamation. Recently, researchers have identified both messenger proteins and specific types of DNA that are present in the blood of individuals with a genetically-associated sub-type of Parkinson’s. The discovery could provide both novel biomarkers, but also point towards specific biological pathways that could be therapeutically targetted. In today’s post, we will review this new research. # # # # |
When cells in your body are stressed, damaged, or sick, they begin to release large amounts of tiny messenger proteins which inform the rest of your body that something is wrong.
When enough of these messenger proteins are released, cells of the immune system will become activated, and come looking for the source of the trouble.
This is inflammation.
 Source: Youtube
Source: Youtube
Inflammation is a critical part of the immune system’s response to problems. It is the body’s way of communicating with the immune system and explaining that something is wrong. This also aid in activating the immune system so that it can help deal with the situation.
By releasing the messenger proteins (called cytokines), injured/sick cells kick off a process that results in multiple types of immune cells entering the troubled area of the body and undertaking very specific tasks.
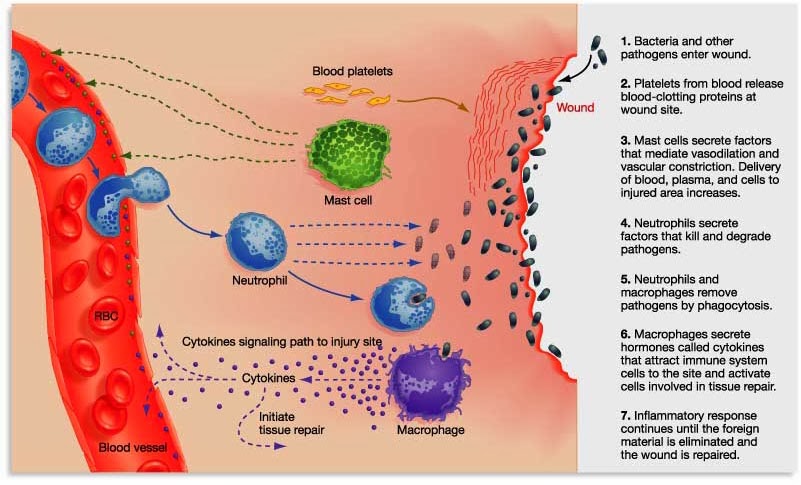 The inflammatory process. Source: Trainingcor
The inflammatory process. Source: Trainingcor
The strength of the immune response depends on the volume of the signal arising from those released messenger proteins.
For a long time, it has been hoped that some of these messenger proteins might be useful as biomarkers for conditions like Parkinson’s. And recently, researchers have published data suggesting that they might have found one cytokine that could be very useful for a specific sub-set of people with Parkinson’s.
What did they find?







