We have previously discussed the strange connection between Melanoma and Parkinson’s disease (click here to read that post).
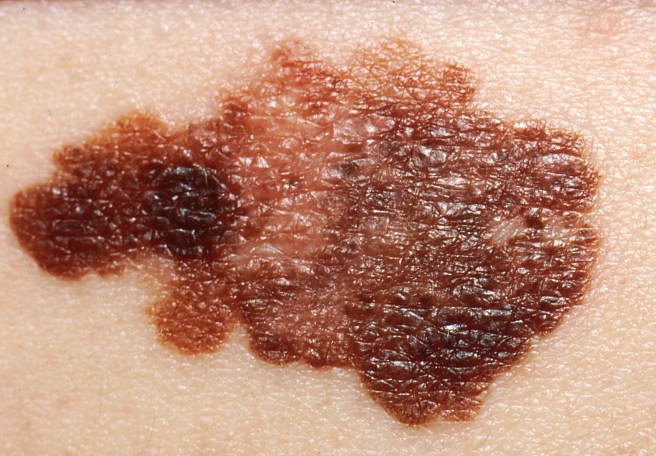
That post included the curious observations that:
- People with Parkinson’s disease are 2-8 times more likely to develop melanoma than people without Parkinson’s.
- People with melanoma are almost 3 times more likely to develop Parkinson’s disease than someone without melanoma.
And we have no idea why (there is no shared genetic predisposition for the two conditions).
Research published this week, however, may begin to explain part of the connection:

Title: Parkinson disease (PARK) genes are somatically mutated in cutaneous melanoma.
Authors: Inzelberg R, Samuels Y, Azizi E, Qutob N, Inzelberg L, Domany E, Schechtman E, Friedman E.
Journal: Neurol Genet. 2016 Apr 13;2(3):e70.
PMID: 27123489 (This research article is OPEN ACCESS if you would like to read it)
In this study, the scientists looked at somatic mutations in cells from 246 tissue samples of melanoma.
What are somatic mutations?
Somatic mutations are genetic alteration that have been acquired by a cell that can then be passed to the progeny of that mutated cell (via cell division). These somatic mutations are different from ‘germline’ mutations, which are inherited genetic alterations that are present in the sperm and egg that were used in making each of us.

Somatic vs Germline mutations. Source: AutismScienceFoundation
In the 246 samples analysed, the researchers found 315,914 somatic mutations in 18,758 genes. Yes, that is a lot, but what was very interesting was their discovery of somatic mutations in many of the PARK genes.
What are PARK genes?
There are a number (approx. 20) genes that are now recognised as conferring vulnerability to developing Parkinson’s disease. These genes are referred to as PARK genes. They include the gene that makes the protein Alpha synuclein ( SNCA ) and many others with interesting names (like PINK1 and LRRK2). Approximately 15% of cases of Parkinson’s are believed to occur because of a mutation in one (or more) of the PARK genes. As a result there is a lot of research being conducted on the PARK genes.
Were all of PARK genes mutated in the Melanoma samples?
Somatic mutation in 14 of the 15 PARK genes (that the researchers analysed) were present in the melanoma samples. This means that after the skin cells turned into melanoma cancer cells, they acquired mutations in some of the PARK genes. Overall, 48% of the analysed samples had a mutation in at least 1 PARK gene, and 25% had mutations in multiple PARK genes (2–8 mutated genes). One PARK gene in particular, PARK 8, was more significantly present in the melanoma cells than the others. PARK8 is also known as Leucine-rich repeat kinase 2 or LRRK2 (we have previously discussed Lrrk2 – click here to read that post). Three additional PARK genes (PARK2, PARK18, and PARK20) were also significantly present, but not as significant as Lrrk2.
So what does it all mean?
The researchers speculate in the discussion of their report about what the findings could mean, but it is interesting to note that many of the PARK genes are susceptible to acquiring mutations (particularly Lrrk2). And this is important to consider when thinking about our development as individual human beings – even though you may not born with a particular mutation for Parkinson’s disease (you haven’t inherited it from our parents), somewhere along the developmental pathway (from egg fusing with sperm to full grown adult) you could acquire some of these mutations which would make you vulnerable to Parkinson’s disease.And here we should note that skin and brain share the same developmental source (called the ectoderm). A mutation in a PARK gene could occur during your development and you would never know.
We thought this was a very interesting study – certainly worthy of reporting here.


