Novel therapeutic approaches for Parkinson’s disease are popping up all the time.
Recently there has been quite a bit of noise in the media regarding something called ‘focused ultrasound-based therapies‘ for Parkinson’s disease. We’re talking about reports such as this and this.
The initial results look very exciting and the Michael J Fox foundation has helped to fund a phase one clinical trial of the technology, but what exactly is focused ultrasound?
Let’s start at the beginning: Ultrasound
Ultrasound is defined as sounds at frequencies greater than 20 kHz. These are at high frequencies and short wavelengths.

Approximate frequency ranges corresponding to ultrasound. Source: Wikipedia
The human ear is not designed to register ultrasound, but it is still useful to us. Since ultrasound was first used by Paul Langevin to detect submarines in 1917, we have found many uses for it, most of them in the field of medicine (notably the imaging of unborn babies and breaking up kidney stones).
The use of ultrasound in procedures involving the brain has previously been very limited because of that natural protective helmet we call the skull. Normal ultrasound does not penetrate the skull very well. High intensity ultrasound, however, does.
So what is focused ultrasound?
High intensity focused ultrasound, also known as magnetic resonance guided focused ultrasound, is a procedure that uses very intense ultrasound generated from multiple points but focused on one specific area. The waves from those different points of emission are all in phase – that is to say their waves match. All that ultrasound concentrated in one location generates a lot of heat at that focal point. That heat allows for the destruction of diseased or damaged tissue at that particular point of focus.

A schematic demonstrating the focused ultrasound technique. Source: Ghanouni et al (2015)
The procedure is relatively quick, non-invasive (no surgery). The subject is placed on a bed and their head is covered by a cooling unit. Around the cooling unit is the ultrasound transducer array – multiple generators of the ultrasound pointing in toward the skull.

Images demonstrating the focused ultrasound technique: Source: Ghanouni et al (2015)
The subject, the cooling unit, and the transducer array are then placed inside an MRI brain scanning machine to allow for extremely accurate focusing of the ultrasound waves. Once everything is in place, the procedure will begin. According to the scientists conducting the research, the procedure – from start to finish – takes approximately 2 hours.
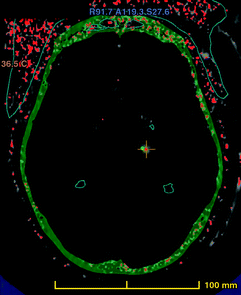 A brain scan image of the area being targeted (red cross). The skull is in green, and the cooled water unit is is red. Source: Ghanouni et al (2015)
A brain scan image of the area being targeted (red cross). The skull is in green, and the cooled water unit is is red. Source: Ghanouni et al (2015)
So what has been done research wise?
The research about using focused ultrasound in Parkinson’s disease is still very new. The first papers investigating the utility of the technology with regards to PD were only published a couple of years ago.
These papers include:

Title: First experience with MR-guided focused ultrasound in the treatment of Parkinson’s disease.
Authors: Magara A, Bühler R, Moser D, Kowalski M, Pourtehrani P, Jeanmonod D.
Journal: J Ther Ultrasound. 2014 May 31;2:11.
PMID: 25512869 (This article is OPEN SOURCE if you would like to read it)
This study was the first report of focused ultrasound being employed in humans with Parkinson’s disease. The researchers performed a pallidothalamic tractotomy (or destruction of the fibres connecting the basal ganglia to the thalamus – see our previous post about these structures). This removed the inhibitory signal being sent to the thalamus, allowing it to function more freely.
In this paper, the procedure was performed on 13 patients, demonstrating the safety and efficacy of the approach. The investigators reported a 60% improvement in Parkinson’s motor assessment (using the UPDRS) at 3 months post procedure.

Title: MRI Guided Focused Ultrasound Thalamotomy for Moderate-to-Severe Tremor in Parkinson’s Disease.
Authors: Schlesinger I, Eran A, Sinai A, Erikh I, Nassar M, Goldsher D, Zaaroor M.
Journal: Parkinsons Dis. 2015;2015:219149.
PMID: 26421209 (This article is also OPEN SOURCE if you would like to read it)
This study involved 7 subjects with Parkinson’s disease who received a thalamotomy (the destruction of part of the thalamus) using focused ultrasound. The subjects demonstrated a better than 50% improvement in their motors scores and the effects were sustained for at least 7 months post procedure.

Title: Unilateral magnetic resonance-guided focused ultrasound pallidotomy for Parkinson disease.
Authors: Na YC, Chang WS, Jung HH, Kweon EJ, Chang JW.
Journal: Neurology. 2015 Aug 11;85(6):549-51.
PMID: 26180137
In this case study report, the researchers conducted a pallidotomy (the destruction of the source of the fibres projecting to the thalamus) using focused ultrasound in a patient with Parkinson’s disease who had extremely severe dyskinesias (uncontrollable movements associated with long term use of PD medications). They reported 70-80% reductions in many of the motor assessments at 6 months post-procedure. The researchers noted many of the complications of deep brain stimulation that can be avoided with this technique (those complications include infection & hemorrhage due to surgery, and hardware-related complications with the expensive devices).
Importantly all of these study illustrated that the focused ultrasound technique was safe and had beneficial effects.
In Summary:
Focused ultrasound therapy is a new experimental treatment that is being tested in people with Parkinson’s disease. It is currently being oriented as a treatment option for people with Parkinson’s who have severe dyskinesias.
The pros of the focused ultrasound technology/approach:
- No surgery – the procedure is non-invasive
- No risk of infection
- Little collateral damage (e.g. due to instruments passing through the cortex to get to the target region)
- The effect is relatively immediate
The cons:
- It does not cure the disease, merely alleviates motor features (tremors, etc)
- It is very important to note that the focused ultrasound procedure is irreversible.
- Once performed, the effect is unadjustable – there is no ‘volume control’ on the resulting effect.
- The technique is still experimental and the researchers do not know how long the effects will last.
We here at the Science of Parkinson’s have presented this post for information purposes. We are not affiliated with any of the groups/companies currently promoting this treatment. We have tried to remain unbiased in our explanations and assessment.
We would like to see some long-term data on the focused ultrasound approach before passing judgement on this treatment approach. Importantly, we need to know how long the effect can last – this will most likely vary from person to person. Given that the disease will still be progressing in individuals who have this treatment, it would be interesting to see the longer term consequences.
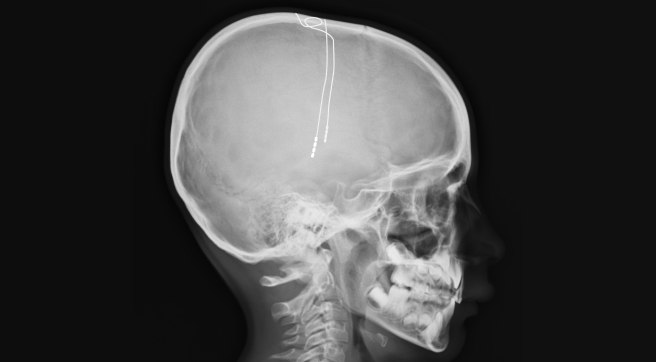
We would also like to see a comparative study between focused ultrasound and deep brain stimulation (the current best option for people with severe dyskinesias). Deep brain stimulation is an invasive, surgical procedure in which a ‘pacemaker’ like probe is inserted into the brain. Importantly deep brain stimulation is adjustable (the electrical signal being sent into the brain can be fine tuned) while focused ultrasound is not adjustable once the procedure is completed. Given this last detail, we believe that the focused ultrasound should remain a last choice option in any treatment approach to Parkinson’s disease (at least for the time being).





 A brain scan image of the area being targeted (red cross). The skull is in green, and the cooled water unit is is red. Source:
A brain scan image of the area being targeted (red cross). The skull is in green, and the cooled water unit is is red. Source: 

