I really didn’t expect to be writing about Parkinson’s research being conducted in New Zealand again so quickly, but yesterday a new study was published which has a few people excited.
It presents evidence of how the disease may be spreading… using cells collected from people with Parkinson’s disease.
In today’s post we will review the study and discuss what it means for Parkinson’s disease.

The South Island of NZ from orbit. Source: Sciencenews
We may have mentioned the protein Alpha synuclein once or twice on this blog.
For anyone familiar with the biology of Parkinson’s disease, alpha synuclein is a major player. It is either public enermy no.1 in the underlying pathology of this condition or else it is the ultimate ‘fall guy’, left standing in the crime scene holding the bloody knife.
Remind me, what is alpha synuclein?
Alpha synuclein is an extremely abundant protein in our brains – making up about 1% of all the proteins floating around in each neuron (one of the main types of cell in the brain).
In healthy brain cells, normal alpha synuclein is typically found just inside the surface of the membrane surrounding the cell body and in the tips of the branches extending from the cell (in structures called presynaptic terminals which are critical to passing messages between neurons).
And why is alpha synuclein important in Parkinson’s disease?
Genetic mutations account for 10-20% of the cases in Parkinson’s disease.
Five mutations in the alpha-synuclein gene have been identified which are associated with increased risk of Parkinson’s disease (A53T, A30P, E46K, H50Q, and G51D – these are coordinates for locations on the alpha synuclein gene). Rare duplication or triplication of the gene have also been associated with Parkinson’s disease.
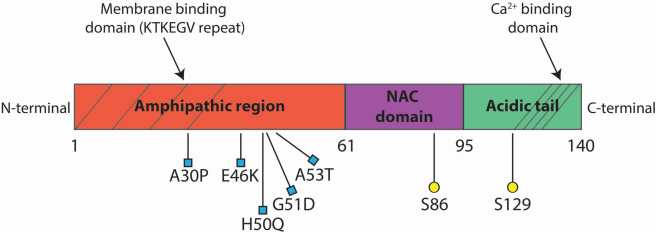
The structure of alpha synuclein protein – blue squares are mutations. Source: Mdpi
So genetically, alpha synuclein is associated with Parkinson’s disease. But it is also involved at the protein level.
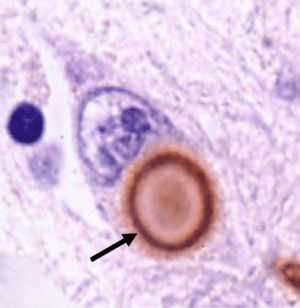
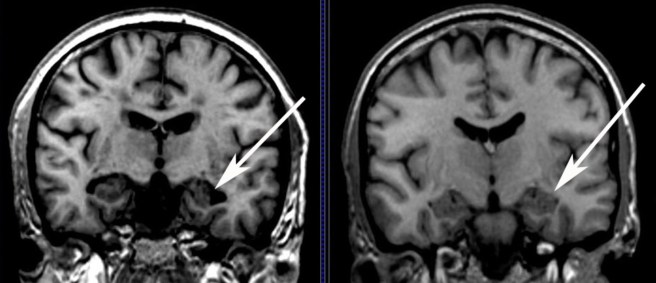
In brains of many people with Parkinson’s disease, there are circular clumps of alpha synuclein (and other proteins) that collect inside cells. These clumps are called Lewy bodies. They are particularly abundant in areas of the brain that have suffered cell loss.
A lewy body (brown with a black arrow) inside a cell. Source: Cure Dementia
No one has ever seen the process of Lewy body formation, so all we can do is speculate about how these aggregates develop. Currently there is a lot of evidence supporting the idea that alpha synuclein can be passed between cells. Once inside the new cell, the alpha synuclein helps to seed the formation of new Lewy bodies, and this is how the disease is believed to progress.
The passing of alpha synuclein between brain cells. Source: Nature
Exactly how alpha synuclein is being passed between cells is the topic of much research at the moment. There are many theories and some results implicating methods such as direct penetration, or via a particular receptor. Perhaps even by a small package called an exosome being passed between cells (see image above).
How this occurs in the Parkinson’s disease brain, however, is unknown.
And this (almost) brings us to the kiwi scientists.
Last years, a group of Swiss scientists demonstrated that alpha synuclein could be passed between cells via ‘nanotubes’ – tiny tubes connecting between cells. The outlined their observations and results in this article:

Title: Tunneling nanotubes spread fibrillar α-synuclein by intercellular trafficking of lysosomes.
Authors: Abounit S, Bousset L, Loria F, Zhu S, de Chaumont F, Pieri L, Olivo-Marin JC, Melki R, Zurzolo C.
Journal: EMBO J. 2016 Oct 4;35(19):2120-2138.
PMID: 27550960
The researchers who conducted this study were interested in tunneling nanotubes.
Yes, I know, ‘What are tunneling nanotubes?’
Tunneling nanotubes (also known as Membrane nanotubes or cytoneme are long protrusions extending from one cell membrane to another, allowing the two cells to share their contents. They can extend for long distances, sometimes over 100 μm – 0.1mm, but that’s a long way in the world of cells!

Tunneling nanotubes (arrows). Source: Wikipedia (and PLOSONE)
Previous studies had demonstrated that tunneling nanotubes can pass different infectious agents (HIV for example – click here to read more on this), supporting the idea that these structures could be a general conduit by certain diseases could be spreading.
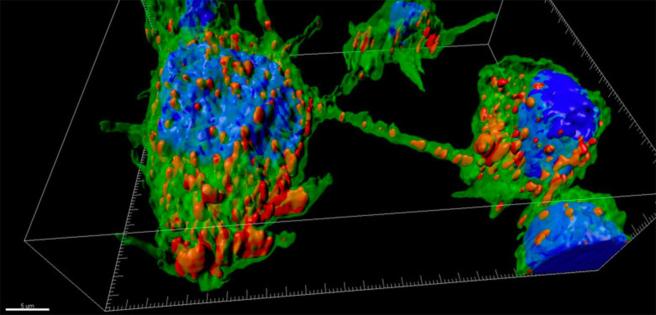
A tunneling nanotube between two cells. Source: Pasteur
In their study the Swiss researchers found that alpha synuclein could be transferred between brain cells (grown in culture) via tunneling nanotubes. In addition, following that process of transfer, the alpha synuclein was able to induce the aggregation (or clumping) of the alpha synuclein in recipient cells.
A particularly interesting finding was that alpha synuclein appeared to encourage the appearance of tunneling nanotubes (there were more tunneling nanotubes apparent when cells produced more alpha synuclein). And the alpha synuclein that was being transferred was being passed on in ‘lysosomal vesicles’ – these are the rubbish bags of the cell (lysosomal vesicles are used to take proteins away for degradation).
Paints a rather insidious picture of the ‘ultimate fall guy’ huh!
And that image was made worse by the results published by the kiwis last night:

Title: α-synuclein transfer through tunneling nanotubes occurs in SH-SY5Y cells and primary brain pericytes from Parkinson’s disease patients
Authors: Dieriks BV, Park TI, Fourie C, Faull RL, Dragunow M, Curtis MA.
Journal: Scientific Reports, 7, Article number: 42984
PMID: 28230073 (This article is OPEN ACCESS if you would like to read it)
In their study, the New Zealand scientists extended the Swiss research by looking at cells collected from people with Parkinson’s disease. The researchers took human brain pericytes, which were derived from the postmortem brains of people who died with Parkinson’s disease.
And before you ask: pericytes are cells that wrap around the cells lining small blood vessels. They are important to the development of new blood vessels and maintaining the structural integrity of microvasculature.

A pericyte (blue) hugging a blood vessel (red). Source: Xvivo
Pericytes contain alpha synuclein precipitates like those seen in neurons, and the kiwi scientists demonstrated that pericytes too can transfer alpha synuclein via tunneling nanotubes to neighbouring cells – representing a non-neuronal method of transport.
They also found that the transfer through the tunneling nanotubes can be very rapid – within 30 seconds – and the transferred alpha synuclein can hang around for more than 72 hours, suggesting that it is difficult for the receiving cell to dispose of. The researchers did note that the transfer through tunneling nanotubes occurred only in small subset of cells, but that this could explain the slow progression of Parkinson’s disease over time.
What does it all mean?
In order for us to truly tackle Parkinson’s disease and bring it under control, we need to know how this slowly progressing neurodegenerative condition is spreading. Some researchers in New Zealand have provided evidence involving cells collected from people with Parkinson’s disease that indicates one method by which the disease could be passed from one cell to another.
Tiny tunnels between cells, allowing material to be shared, could explain how the disease slowly progresses. The scientists observed the Parkinson’s associated protein alpha synuclein being passed between cells and then hanging around for more than a few days.
This method of transfer was made more interesting because the New Zealand researchers reported that non-neuronal cells (Pericytes, collected from people with Parkinson’s disease) could also form tunneling nanotubes. This observation raises questions as to what role non-neuronal cells could be playing in Parkinson’s disease.
This line of questions will obviously be followed up in future research, as will efforts to determine if tunneling nanotubes are actually present in the human brain or simply biological oddities present only in the culture dish. Demonstrating nanotubes in the brain will be difficult, but it would provide us with solid evidence that this method of disease transfer could be a bonafide cause of disease spread.
We watch with interest for further work in this area.
FULL DISCLOSURE: The author of this blog is a kiwi… and proud of it. He is familiar with the researchers who have conducted this research, but has had no communication with them regarding the publishing of this post. He simply thought that the results of their study would be of interest to the Parkinson’s community.
The banner for today’s post was sourced from Pinterest