|
# # # # Over the past two decades, pharmaceutical companies have shifted from maintaining large in-house drug development platforms to a model that involves acquiring small biotech firms with interesting agents once those companies reach a certain point in their maturation. This week a biotech firm called Inflazome was bought by the big pharma Roche. Inflazome has been developing a novel NLRP3 inhibitor, which targets inflammasome activation and the company has had Parkinson’s in it’s sights as far as indications of interest. In today’s post, we will discuss what the inflammasome is, how NLRP3 inhibitors work, and what will be happening next. # # # # |
 Source: Science
Source: Science
One of the hottest areas of Parkinson’s research world is ‘inflammation‘ (cheesy pun intended).
What is inflammation?
When cells in your body are stressed or sick, they begin to release tiny messenger proteins which inform the rest of your body that something is wrong.
When enough of these messenger proteins are released that the immune system becomes activated, it can cause inflammation.
Inflammation is a critical part of the immune system’s response to trouble. It is the body’s way of communicating to the immune system that something is wrong and activating it so that it can help deal with the situation.
By releasing the messenger proteins (called cytokines), injured/sick cells kick off a process that results in multiple types of immune cells entering the troubled area of the body and undertaking very specific tasks.
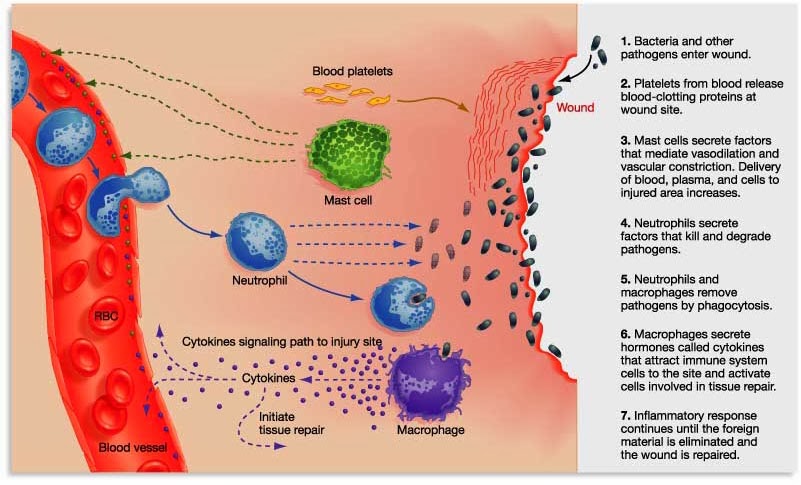 The inflammatory process. Source: Trainingcor
The inflammatory process. Source: Trainingcor
The strength of the immune response depends on the volume of the signal arising from those released messenger proteins. And there are processes that can amplify the immune response.
One of those processes is called inflammasomes.
What are inflammasomes?