|
A reader recently asked for an explanation of some recent research regarding diabetes and Parkinson’s. You see, a significant proportion of the Parkinson’s community have glucose intolerance issues and some live with the added burden of diabetes. That said, the vast majority of diabetics do not develop PD. Likewise, the vast majority of people with Parkinson’s do not have a diagnosis of diabetes. There does appear to be a curious relationship between Parkinson’s and diabetes, with some recent research suggests that this association can be detrimental to the course of the condition. In today’s post we will look at what what diabetes is, consider the associations with Parkinson’s, and we will discuss the new research findings. |
Foreman and Ali. Source: Voanews
1974 was an amazing year.
On October 30th, the much-hyped heavyweight title match – the ‘Rumble in the Jungle’ – between George Foreman and Muhammad Ali took place in Kinshasa, Zaire (Democratic Republic of the Congo).
Stephen King. Source: VanityFair
A 26-year-old author named Stephen King published his debut novel, “Carrie” (April 5, with a first print-run of just 30,000 copies).
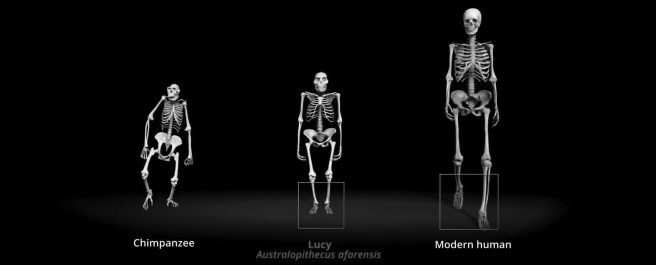
Lucy. Source: Youtube
The fossil remains of a 3.2 million years old hominid skeleton was discovered in Ethiopia (November 24th). It was named ‘Lucy’ – after the song “Lucy in the Sky with Diamonds” by The Beatles which was played repeatedly in the expedition camp the evening after the team’s first day of work on the site (Source).
And Richard Nixon becomes the first US president to resign from office (August 9th).
President Richard Nixon. Source: Fee
In addition to all of this, in December of 1974, a small study was published in the Journal of Chronic Diseases.
It dealt with Parkinson’s and it presented a rather startling set of findings: