|
# # # # Drug repurposing (repositioning, reprofiling or re-tasking) is a strategy of identifying novel uses for clinically approved (or experimental) drugs that fall outside the scope of the original medical indication. Many drug repurposing efforts have started with screening experiments, looking for drugs with certain properties. Recently, researchers conducted a drug repurposing screening experiment for molecules that enhance a Parkinson’s protein (called GCase) and they found an interesting result: the antipsychotic medication quetiapine. In today’s post, we will explain what GCase does, review what the new study found, and consider what could happen next. # # # # |
At the recent “Rallying to the Challenge” meeting (which was conducting in parallel with the Van Andel Institute‘s “Grand Challenges in Parkinson’s Disease“), I was asked by Cure Parkinson’s to present on why the biology surrounding genetic risk factors – like variation in the GBA and LRRK2 genes – are important targets for potential therapeutic intervention in Parkinson’s (my presentation starts at 2 hours & 10 minutes into the video above).
Specifically, I was asked to discuss why they are important targets not just for individuals carrying the genetic variations in these genes, but for the wider Parkinson’s community in general. And it is a good question.
How could inhibitors of LRRK2 or enhancers of GCase activity possibly be useful to individuals with idiopathic (spontaneous or not associated with a genetic risk factor) Parkinson’s?
My answer was rather simple.
What was it?
In the case of LRRK2 there is evidence that some individuals with Parkinson’s have increased levels of LRRK2 activity.
For example:
Title: LRRK2 activation in idiopathic Parkinson’s disease
Authors: Di Maio R, Hoffman EK, Rocha EM, Keeney MT, Sanders LH, De Miranda BR, Zharikov A, Van Laar A, Stepan AF, Lanz TA, Kofler JK, Burton EA, Alessi DR, Hastings TG, Greenamyre JT
Journal: Science Translational Medicine 25 Jul 2018: 10 (451), eaar5429.
PMID: 30045977 (This report is OPEN ACCESS if you would like to read it)
In this study, the researchers reported that many cases of idiopathic Parkinson’s showed about a 4-6 fold increase in markers of LRRK2 activity (compared with the control brains). This result suggested to the researchers that normal (un-mutated) LRRK2 protein may be highly activated in Parkinson’s.
In addition, data from the recent Denali Therapeutics Phase I clinical trial indicate elevated levels of the LRRK2 target protein (RAB10) in individuals with idiopathic Parkinson’s (Click here to read more about this trial and to learn more about LRRK2 in Parkinson’s).
And similar data exists for GBA/GCase.
There are reports that GCase activity in the brain reduces as all of us get older:
 Title: Progressive decline of glucocerebrosidase in aging and Parkinson’s disease.
Title: Progressive decline of glucocerebrosidase in aging and Parkinson’s disease.
Authors: Rocha EM, Smith GA, Park E, Cao H, Brown E, Hallett P, Isacson O.
Journal: Ann Clin Transl Neurol. 2015 Apr;2(4):433-8.
PMID: 25909088 (This report is OPEN ACCESS if you would like to read it)
In this study, the researchers collected frozen postmortem brain tissue from both male and female sporadic Parkinson’s patients and neurologically unaffected control cases. They then measured GCase activity in substantia nigra and putamen – two regions of the brain that are severely affected by Parkinson’s.
The investigators found that GCase activity in control (non-Parkinson’s) cases decreased in the substantia nigra and the putamen across the sixth to eighth decades of life – indicating an age-associated decline in GCase activity.
Source: PMC
But importantly, this reduction in GCase activity was lower in idiopathic Parkinson’s cases across many of these decades of life (in both the putamen and substantia nigra).
 Source: PMC
Source: PMC
And remember that these cases of Parkinson’s did not have any genetic variations in their GBA genes.
So something strange is occurring as we age that results in lower levels of GCase activity in everyone, but this effect is exacerbated for some reason in some people with Parkinson’s (without GBA variants).
Before we go on: What is GBA and GCase?
Glucocerebrosidase (also known as GCase) is an enzyme that helps with the digestion and recycling of various proteins (particularly glucocerebrosides) inside cells.
The enzyme is located and active inside small bags of degradative enzymes. These bags are the lysosomes and they can be found floating around inside of cells.
How do these lysosomes work?
On a relatively continual basis, small parts of a cell membrane are being brought inside the cell. This is a process called endocytosis.
It occurs when the cell needs to consume resources from the outside world in order to find what it requires to function and survive. As a section of cell membrane is brought into the cell, it forms what is called a vesicle (which is a term used to refer to small spherical bags of stuff inside cells). Given the process by which these outer membrane vesicles are formed, they is referred to as endosomes (sometimes it is also called a vacuole).
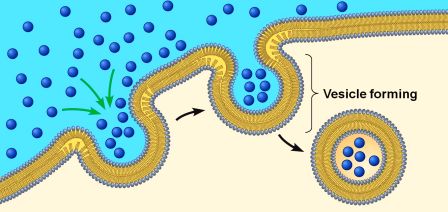 Source: Socratic
Source: Socratic
Once the endosome is inside the cell and detached from the rest of the membrane, it will bind to another vesicle which is called a lysosome. And as I mentioned above, lysosome is a small bag that is full of digestive enzymes, which help to break down the contents of the endosome.

How lysosomes work. Source: Prezi
The lysosome will fuse with the endosome/vacuole and the enzymes from the lysosome will mix with the material in the vacuole and digest it (or it break down into more manageable components).
This enzymatic process works in a very similar fashion to the commercial products that you use for washing your clothes.
 Enzymatic degradation. Source: Samvirke
Enzymatic degradation. Source: Samvirke
The reagents that you put into the washing machine with your clothes contain a multitude of enzymes, which help to break down the dirty, bacteria, flakes of skin, etc that cling to your clothes. Each enzyme breaks down a particular protein, fat or such like. And this is very similar to the collection of enzymes in the lysosome. All of them are needed to break down all of the contents of the endosome.
And if one of those enzymes – such as GCase – is faulty (due to a genetic mutation), then the enzymatic process is disrupted, which could result in the build up of un-degraded material over time.
Ok, that’s GCase, but what is GBA and how is it associated with Parkinson’s?
The enzyme GCase is produced by cells using instructions provided by the GBA gene (a gene is a section of DNA that provides the instructions for making a particular protein).
Tiny errors (called genetic variations) in the GBA gene are associated with an increased risk of developing Parkinson’s.
In fact, they are one of the most common genetic risk factors for the condition.
It is believed that approximately 5%–8% of people with Parkinson’s have a genetic mutation in their GBA gene (Click here and here to read more about this).
Researchers have been looking for drugs that can increase levels of GCase, in the hope that it will help boost the recycling system of cells of people with Parkinson’s and make the cells healthier. And if the cells are healthier, perhaps this would slow down the progression of Parkinson’s.
And given that GCase levels are lower in some people with idiopathic Parkinson’s as well as those with genetic variations in their GBA gene, drugs that boost GCase activity could be useful in treating a wide portion of the PD community.
Thus there have been many efforts to screen for and identify drugs that increase GCase activity.
|
# RECAP #1: Genetic variations in a section of DNA called the GBA1 gene, are associated with an increased risk of Parkinson’s, and results in reduced activity of an enzyme named GCase. GCase is involved in the waste disposal system of cells, helping to break down old/used proteins. It functions in small bags of waste – called lysosomes – inside of cells. Drugs that enhance GCase activity could be useful in the treatment of Parkinson’s # |
Have those screening studies identified any drugs of interest?
We have previously discussed the respiratory medication ambroxol, which Cure Parkinson’s and partners are clinically testing (click here to read a previous SoPD post on this topic).
But very recently (this past week), a new research report was published that identified another drug:
 Title: Direct targeting of wild-type glucocerebrosidase by antipsychotic quetiapine improves pathogenic phenotypes in Parkinson’s disease models.
Title: Direct targeting of wild-type glucocerebrosidase by antipsychotic quetiapine improves pathogenic phenotypes in Parkinson’s disease models.
Authors: Burbulla LF, Zheng J, Song P, Jiang W, Johnson ME, Brundin P, Krainc D.
Journal: JCI Insight. 2021 Oct 8;6(19):e148649.
PMID: 34622801 (This report is OPEN ACCESS if you would like to read more about it)
In this study, the researchers conducted a screening experiment that involved testing 1280 FDA-approved drugs to determine if any of them could increase GCase activity – in an attempt to identify any drugs that could be potentially repurposed for Parkinson’s.
And did they identify any?
Yes, they did.
The investigators found seven drugs of interest, but they focused on an anti-psychotic drug called quetiapine (pronounced: kwuh·tai·uh·peen), due to it’s high binding affinity to normal GCase protein (KD value of 5 μM).
They found that increasing concentrations of quetiapine was not only able to bind to GCase, but also increase levels of the enzyme in cells carrying a GBA-associated Parkinson’s mutation (c.84dupG frame-shift mutation):
 Source: JCI
Source: JCI
They also reported that quetiapine treatment was able to reduce levels of the Parkinson’s associated protein alpha synuclein in cells, as well as reducing the amount of oxidized dopamine (which is believed to contribute to lysosomal dysfunction):
Source: JCI
And it was not just in cell culture that quetiapine was having this effect on GCase. When the researchers treated mice with GBA1 mutations (Gba1D409V/+ mutant mice) with quetiapine (twice daily for 15 days), they observed increase GCase levels and reduced alpha synuclein in the brain:
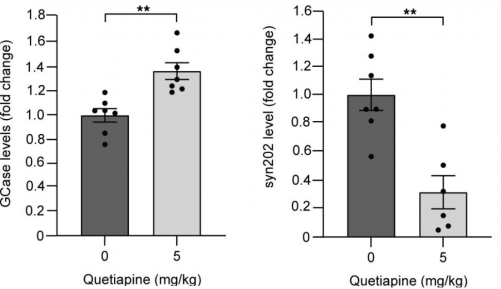 Source: JCI
Source: JCI
The researchers concluded their study by suggesting that their “findings highlight the potential value of quetiapine as a therapeutic approach for different forms of PD, including familial and sporadic PD. Future clinical studies will be required to fully evaluate quetiapine’s potential for the treatment of PD and to define appropriate doses for long-term therapy”.
|
# # RECAP #2: New research has found that the anti-psychotic drug quetiapine can bind to normal GCase protein and increase its activity. Exactly how it is increasing the activity still needs to be determined, but quetiapine was able to rescue cell culture models of Parkinson’s. Quetiapine treatment also increase levels of GCase activity in the brains of mice, and reduce levels of alpha synuclein accumulation in a Parkinson’s mouse model. # # |
Interesting. So where can I get me some quetiapine?
The results of this new study are very interesting, but the results need to be independently validated and there is still a lot of work to be done before we can get too excited.
Although it has been used clinically for a very long time and is a well characterised drug (approved way back in 1997), there are some important details that need to be considered regarding quetiapine in the context of Parkinson’s.
In addition to this binding to GCase result, quetiapine is well known to block various receptors in the brain (such as 5-HT2, alpha1 and H1 receptors). Most importantly, quetiapine also binds antagonistically to dopamine receptors (D2 in particular), preventing dopamine from binding to its receptor.
This might not be such a good thing in terms of dopamine therapy for Parkinson’s.
Likewise, quetiapine is known to lower blood pressure, and many individuals with Parkinson’s have blood pressure issues (such as orthostatic hypotension). It can also cause constipation – another favourite within the PD community (it does this via antagonism of muscarinic cholinergic receptors).
Has quetiapine ever been tested in Parkinson’s?
To be fair, quetiapine has been widely used in Parkinson’s for the management of psychoses. Recently a follow up analysis of this drug in PD has recently been conducted:
 Title: Clinical Follow-up of Parkinson’s Disease With Newly Prescribed Quetiapine.
Title: Clinical Follow-up of Parkinson’s Disease With Newly Prescribed Quetiapine.
Authors: Weintraub D, Chiang C, Kim HM, Wilkinson J, Marras C, Stanislawski B, Mamikonyan E, Kales HC.
Journal: Mov Disord. 2020 Sep;35(9):1690-1692.
PMID: 32725640 (This report is OPEN ACCESS if you would like to read more about it)
In this study, the researchers analysed the clinical records of 261 individuals with idiopathic Parkinson’s who had been prescribed quetiapine and they found that those who had negative responses to the drug were typically more advanced in their PD symptoms (as measured by the Hoehn & Yahr scale).
A similar analysis of outcomes study conducted in Sweden concluded that “quetiapine should be used with caution in elderly patients with Parkinson’s” (Click here to read more about this).
So while quetiapine has been prescribed to individuals with Parkinson’s, there may be some caution required in terms of the precise cohort that this drug could be tested on in a clinical trial exploring the implications of this new GCase finding (if independent replication can replicate the result).
So what does it all mean?
Drug repurposing represents a great way of bringing new therapies to patients. It speeds up the clinical development process as the agents being repurposed are typically well characterised from years of clinical use. This enables certain chunks of the clinical trial process to be skipped or sped up, greatly accelerating the testing and delivery of the repurposed treatments.
This process has led to large drug screening experiments focused on very specific aspects of disease biology – looking for clinically approved molecules that have an unrecognized function that could be useful in a new disease indication.
Recently researchers have identified the anti-psychotic drug called quetiapine as an activator of the Parkinson’s-associated protein GCase. Reduced levels of this enzyme have been reported in individuals with genetic risk factors as well as those without these variants. Further work is required to better understand the mechanism by which quetiapine is having its effect, as well as the dose range. Given some of the other features of this drug it may not be the best molecule for repurposing, but this research could provide insights into designing better drugs for activating GCase.
 All of the material on this website is licensed under a
All of the material on this website is licensed under a
Creative Commons Attribution 4.0 International License
You can do whatever you like with it!
EDITOR’S NOTE: The information provided by the SoPD website is for information and educational purposes only. Under no circumstances should it ever be considered medical or actionable advice. It is provided by research scientists, not medical practitioners. Any actions taken – based on what has been read on the website – are the sole responsibility of the reader. Any actions being contemplated by readers should firstly be discussed with a qualified healthcare professional who is aware of your medical history. While some of the information discussed in this post may cause concern, please speak with your medical physician before attempting any change in an existing treatment regime.
Further, the author of this post is an employee of the charitable research trust Cure Parkinson’s. The Trust has not asked for this post to be written, and there has been no effort to highlight the work of the Trust over others (perceptions of any bias should be directed to the author). This post has been written by the author solely for the purpose of sharing what the author considers interesting information.
The banner for today’s post was sourced from Youtube





I would be interested in where this research goes….my mom has lewy body dementia and it seemed to send her even more over the edge when she was taking seroquel
LikeLike
Hi Robert,
Thanks for your comment. I have heard of different responses from different people. It may be that quetiapine has responders and non-responders. We will have to wait and see.
Kind regards,
Simon
LikeLike
I just read yesterday but I cannot find the citation…there was a recent study showing no connection betwreen G case and Parkinsons
LikeLike
https://parkinsonsnewstoday.com/2021/10/11/parkinsons-risk-severity-not-linked-gcase-enzyme-activity/…what did you think about this study
LikeLike
Hi Robert,
Thanks for the really interesting comment. It is an intriguing study, but it points towards one of the great challenges in PD research at the moment: How do we measure GCase levels and enzymatic activity accurately?
GCase is an enzyme that functions inside lysosomes, but we can’t measure its ability to do its job because the lysosomes are inside of cells. So our current methods have a degree of error involved due to our inability to accurately measure. In addition (and more importantly), in this study the GCase activity was assessed in blood cells rather than brain cells. A better title for the report would have been “Glucocerebrosidase activity in peripheral blood cells is not associated with Parkinson’s Disease Risk or Severity”. It may be that GCase levels and activity may differ across different tissue types within the same individual (I wrote a post about this a while back: https://scienceofparkinsons.com/2020/06/24/gba/
Assessing GCase levels and activity is really complicated, which is making the clinical testing of drugs targeting GCase problematic. But a lot of smart minds are working on this issue.
I hope this all makes sense.
Kind regards,
Simon
LikeLike