|
New data from researchers in Taiwan has intriguing implications for our understanding of the development of Parkinson’s. An analysis of the enormous national medical database pointed towards towards hepatitis C viral infections as a risk factor for developing Parkinson’s. But here is the twist in the tale: Interferon-based antiviral therapy reduces that risk back to normal. In today’s post, we will review the new research, discuss what interferons are, explore what other research has been conducted on interferons in the context of Parkinson’s, and consider the implications of this new research for Parkinson’s.
|
 Source: Phys
Source: Phys
We have learnt a great deal about Parkinson’s over the last few years via the use of “big data”.
Whether it be the analysis of vast pools of genetic information collected from tens of thousands of individuals with the condition, to analysing massive datasets of longitudinal medical information, these investigations has open new avenues of research and investigation.
For example, “big data” studies have demonstrated that those who smoke cigarettes and drink coffee have a reduced chance of developing Parkinson’s (click here to read a previous SoPD post on this topic). ‘Big data studies have also pointed towards novel therapeutic approaches (click here for a previous SoPD post highighting an example).
Recently, an analysis of medical records from Taiwan have shed new light on another potential influencer of Parkinson’s risk: Hepatitis C
What is Hepatitis C?
The name ‘Hepatitis’ comes from the Greek: Hepat – liver; and itis – inflammation, burning sensation. Thus – as the label suggests – Hepatitis is inflammation of liver tissue.
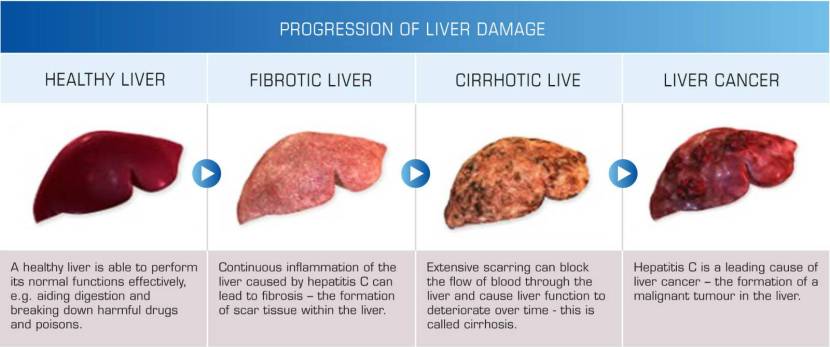
Hepatitis and the liver. Source: HealthandLovepage
It can be caused by infectious agents (such as viruses, bacteria, and parasites), metabolic changes (induced by drugs and alcohol), or autoimmune/genetic causes (involving a genetic predisposition).
The most common cause of hepatitis, however, is viral.
There are five main types of viral hepatitis (labelled A, B, C, D, and E). Hepatitis A and E are mainly spread by contaminated food and water. Both hepatitis B and hepatitis C are commonly spread through infected blood (though Hepatitis B is mainly sexually transmitted). Curiously, Hepatitis D can only infect people already infected with hepatitis B.
Hepatitis A, B, and D are preventable via the use of immunisation. A vaccine for hepatitis E has been developed and is licensed in China (Hecolin®), but is not yet available elsewhere.
Hepatitis C, however, is different.
Different how?
There is currently no vaccine for it, mainly because the virus is highly variable between strains and it mutates very quickly, which makes the development of an effective vaccine very difficult. A number of vaccines under development (Click here for more on this).
Hepatitis C is also the number 1 cause of liver cancer.
What is known about Hepatitis C and the brain?
Quite a bit.
Similar to HIV (which we discussed in a previous post), the hepatitis C virus (HCV) enters the brain via infected blood-derived macrophage cells. In the brain, it is hosted by microglial cells, which results in altered functioning of those microglial cells. This causes problems for neuronal cells – including dopamine neurons. For example, people infected with HCV have reduced dopamine transmission, based on brain imaging studies (Click here and here for more on this result).
Have there been connections between hepatitis C virus and Parkinson’s disease before?
Yes. For example:

Title: Hepatitis C virus infection: a risk factor for Parkinson’s disease.
Authors: Wu WY, Kang KH, Chen SL, Chiu SY, Yen AM, Fann JC, Su CW, Liu HC, Lee CZ, Fu WM, Chen HH, Liou HH.
Journal: J Viral Hepat. 2015 Oct;22(10):784-91.
PMID: 25608223
The researchers in this study used data collected from a community-based screening program in north Taiwan which involved 62,276 people. The World Health Organisation (WHO) estimates that the prevalence of hepatitis C viral infection worldwide is approximately 2.2–3%, representing 130–170 million people. Taiwan is a high risk area for hepatitis, with antibodies for hepatitis viruses in Taiwan present in 4.4% in the general population (Source).
The researchers found that the significant association between hepatitis C viral infections and Parkinson’s – that is to say, a previous infection of hepatitis C increased the risk of developing Parkinson’s (by 40%). The researchers then looked at what the hepatitis C and B viral infections do to dopamine neurons growing in cell culture. They found that hepatitis C virus induced 60% dopaminergic cell death, while hepatitis B had no effect.
This study was followed up a few months later, by a second study suggesting an association between Hepatitis C virus and Parkinson’s:

Title: Hepatitis C virus infection as a risk factor for Parkinson disease: A nationwide cohort study.
Authors: Tsai HH, Liou HH, Muo CH, Lee CZ, Yen RF, Kao CH.
Journal: Neurology. 2016 Mar 1;86(9):840-6.
PMID: 26701382
The researchers in this study wanted to investigate whether hepatitis C could be a risk factor for Parkinson’s. They did this by analyzing data from 2000-2010 drawn again from the Taiwan National Health Insurance Research Database.
The database included 49,967 people with either hepatitis B, hepatitis C or both, in addition to 199,868 people without hepatitis. During the 12 year period, 270 participants who had a history of hepatitis developed Parkinson’s (120 still had hepatitis C). This compared with 1,060 participants who were free of hepatitis, but went on to develop Parkinson’s.
When the researchers controlled for potentially confounding factors (such as age, sex, etc), the researchers found participants with hepatitis C had a 30% greater risk of developing Parkinson’s than the controls.
Very interesting, so what does it all mean?
No, wait. We are not summing up yet. We’re not even close to finishing.
We haven’t got to the really interesting part.
Which is?
So in June of this year, this study was published:
 Title: Association of Antiviral Therapy With Risk of Parkinson Disease in Patients With Chronic Hepatitis C Virus Infection.
Title: Association of Antiviral Therapy With Risk of Parkinson Disease in Patients With Chronic Hepatitis C Virus Infection.
Authors: Lin WY, Lin MS, Weng YH, Yeh TH, Lin YS, Fong PY, Wu YR, Lu CS, Chen RS, Huang YZ.
Journal: JAMA Neurol. 2019 Jun 5.
PMID: 31168563
In this study, the researchers were interested in exploring the risk of developing Parkinson’s in patients with Hepatitis C virus infections. They obtained medical claims data from the Taiwan National Health Insurance Research Database for 188 152 patients with recorded Hepatitis C virus infections.
The researchers then made two equally matched groups of 39 936 cases from this dataset, so that they could compare the characteristics of individuals in the treated group (which included 17 970 female [45.0%] and an average age of 52.8 years) with individuals in the untreated group (which included 17 725 female [44.4%] and an average age of 52.5 years).
What did they mean by treated?
The current standard-of-care treatment in Taiwan for Hepatitis C is administration of alpha-2b interferons and anti-viral therapies (such as protease inhibitors or nucleotide analog polymerase inhibitors).
And this is where this new study gets really interesting:
In their analysis, the researchers found that individuals with chronic Hepatitis C virus infection had a reduced risk of developing Parkinson’s IF they were treated long-term with interferon-based anti-viral therapies.
Hang on a second, go back. What exactly are alpha-2b interferons?
Interferons are a group of proteins that get their name because of what they do: they interfere with the replication of viruses. They also help to protect cells from bacterial infections and may inhibit cancer growth.
They are a family of signaling proteins, which are made and released by cells in your body in response to a viral infection. Interferons causes nearby cells to be on the alert, and to heighten their anti-viral defenses.
 Source: EBC
Source: EBC
Alpha-2b interferons are a particular type of interferon that is used in the treatment of Hepatitis C.
Has there ever been any other associations between interferons and Parkinson’s?
Actually, yes.
In the context of preclinical experiments.
For example:
 Title: Lack of Neuronal IFN-β-IFNAR Causes Lewy Body- and Parkinson’s Disease-like Dementia.
Title: Lack of Neuronal IFN-β-IFNAR Causes Lewy Body- and Parkinson’s Disease-like Dementia.
Authors: Ejlerskov P, Hultberg JG, Wang J, Carlsson R, Ambjørn M, Kuss M, Liu Y, Porcu G, Kolkova K, Friis Rundsten C, Ruscher K, Pakkenberg B, Goldmann T, Loreth D, Prinz M, Rubinsztein DC, Issazadeh-Navikas S.
Journal: Cell. 2015 Oct 8;163(2):324-39.
PMID: 26451483 (This report is OPEN ACCESS if you would like to read it)
In this study, the researchers reported that mice which had been genetically engineered to lack interferon-β develop motor and cognitive learning problems, which are accompanying by the appearance of alpha synuclein-containing Lewy bodies in their brains. Lewy bodies are one of the characteristic hall marks of the Parkinsonian brain (Click here to read a previous SoPD post about Lewy bodies).
The researchers found that absense of interferon-β causes a blockade of the waste disposal process in the cell (called autophagy) which results in a build up of alpha synuclein protein. By re-introducing interferon-β into the cells, the scientists could promote autophagy and help clear the accumulating alpha synuclein protein.
 Source: PMC
Source: PMC
The researchers concluded that their results indicate a protective role for interferon-β in neuronal homeostasis.
Where can I get me some of that interferon stuff?
Before you get too excited, understand a couple of things about interferons:
1. While they may reduce the risk of developing Parkinson’s, we have no data to suggest that they help after a diagnosis has been made.
2. Interferon treatment for hepatitis C typically lasts 24–48 weeks (6–12 months), and it is associated with some unappealing side-effects, including flu-like symptoms (headache, tiredness, and weakness), chills/fever, trouble sleeping, nausea/vomiting and (everybody’s favourite) diarrhea. Interferon treatment is not fun.
3. Our understanding of interferon biology still needs a lot of work. In fact, some of the data is rather confusing.
What do you mean?
We have a lot to learn about interferons.
For example, some patients with chronic Hepatitis C infections who are treated with interferons have been reported to develop Parkinson’s-like features (Click here to read more about this).
In addition, while the administration of interferons may reduce the risk of developing Parkinson’s in Taiwan, most of the preclinical research in the field of Parkinson’s suggests that inhibiting certain aspects of this pathway may actually be beneficial. For example:
 Title: Type-1 interferons contribute to the neuroinflammatory response and disease progression of the MPTP mouse model of Parkinson’s disease.
Title: Type-1 interferons contribute to the neuroinflammatory response and disease progression of the MPTP mouse model of Parkinson’s disease.
Authors: Main BS, Zhang M, Brody KM, Ayton S, Frugier T, Steer D, Finkelstein D, Crack PJ, Taylor JM.
Journal: Glia. 2016 Sep;64(9):1590-604.
PMID: 27404846
In this study, the researchers reported increased levels of type-1 interferon in both post mortem brains from people who passed away with Parkinson’s and neurotoxin-based (MPTP) mouse models of Parkinson’s.
They also found that mice lacking the receptor of type-1 interferon had less inflammatory response and reduced loss of dopamine neurons (compared to normal mice, when both were treated with the neurotoxin MPTP). And the researchers replicated this study using an anti-type-1 interferon treatment – it also reduced neuroinflammation and dopamine cell death in mice treated with the neurotoxin.
This same research group published a second report one year later further exploring this data:
 Title: Type-I interferons mediate the neuroinflammatory response and neurotoxicity induced by rotenone.
Title: Type-I interferons mediate the neuroinflammatory response and neurotoxicity induced by rotenone.
Authors: Main BS, Zhang M, Brody KM, Kirby FJ, Crack PJ, Taylor JM.
Journal: J Neurochem. 2017 Apr;141(1):75-85.
PMID: 28029694
In this study, the researchers used a different neurotoxin (rotenone) on cultured rodent neurons and glial (helper) cells, and found that is also caused interferon‐dependent pro‐inflammatory responses in the cells which ultimately helped cause the neurons to die. The interferons were causing the glial cells to become inflammatory. A similar treatment of glia that had the interferon gene removed resulted in substantially reduced pro‐inflammatory responses and a lot less cell death.
Are there any clinical trials investigating interferons in neurodegeneration?
Not for Parkinson’s – that I am aware of (happy to be corrected on this).
But there has been a clinical trial exploring the use of interferon beta-1a (Rebif®, Merck Serono) in early Alzheimer’s subjects (please note that this is a different type of interferon to the one discussed in the Taiwan report above).
The researchers recruited 42 early Alzheimer’s patients and randomised into two groups. One group of 23 individuals received a subcutaneous injection of interferon beta-1a, while the other group of 19 participants were treated with a placebo three times per week for 28 weeks. The groups were then followed up for a further 24 weeks of observation (with out interferon beta-1a treatment).
The results suggested the short-term use of interferon beta-1a in treatment of older patients at risk for Alzheimer’s-related cognitive decline was well tolerated and although it the results were not statistically significant, there were some interesting trends in the data hinting at possible effects, which the researchers said required further investigation in a larger Phase III study (Click here to read more about the results and click here to read more about this trial design).
I am not aware of a larger study being conducted (happy to be corrected on this).
There is also a human monoclonal antibody that binds to and blocks the type I interferon receptor being developed by the pharmaceutical compant Astrazenica.
It is called Anifrolumab.
It is currently being tested in various autoimmune/inflammatory conditions, and recently demonstrated positive results in a critical Phase III trial of lupus (Click here to read more about this).
But as I said above, we need to understand a lot more about interferons and their biology before we start considering any clinical trials in Parkinson’s. There are many different interferons (20+ different proteins across three distinct families of interferons – according to Wikipedia), and they have different functions.
 Some different types of interferon. Source: Heighpubs
Some different types of interferon. Source: Heighpubs
We would also need to be very careful regarding which people with Parkinson’s would be appropriate for testing an interferon-based approach. We currently do not have the insight or technology required for selecting people in this regarding.
Thus, while the new data from Taiwan is interesting, further research is needed in this area (andrest assured that this is being investigated).
So what does it all mean?
New research from Taiwan – based on big data analysis – suggests that Hepatitis C infection may increase one’s risk of developing Parkinson’s. The data also suggests that the use of antiviral-interferon-based therapy reduces that risk. The results is interesting, but it needs to be independently replicated before we get too excited, and it must be taken with the caveat that the study is based on medical records rather than clinical research.
In addition, while we have explored the biology of interferons in this post, there is one glaring elephant in the room that has not been discussed: The possiblity that a viral agent could be associated with an increased risk of developing Parkinson’s.
We have previously explored this idea here on the SoPD website (Click here to read an example), and I am hoping to re-examine this idea in a future post based on some interesting new research. I have long harboured a viral/bacterial (multi-hit/infection) theory of Parkinson’s. I try to balance out my bias by reading up on all the other interesting research in this field.
Interfering with interferons has re-ignited that bias though.
The banner for today’s post was sourced from NIH


Love what you do thank you so much. What are your thoughts on Neuralink Elan Musk 2019. Dale Vance
On Wed, Sep 4, 2019 at 3:54 PM The Science of Parkinson’s wrote:
> Simon posted: ” New data from researchers in Taiwan has intriguing > implications for our understanding of the development of Parkinson’s. An > analysis of the enormous national medical database pointed towards towards > hepatitis C viral infections as a ris” >
LikeLike