A community in New Brunswick (Canada) was recently shocked to discover that a 2 year old boy in their midst had been diagnosed with Parkinson’s disease (Click here to read more).
Yes, you read that correctly, it’s not a typo: a 2 year old boy.
Juvenile-onset Parkinson’s disease is an extremely rare version of the condition we discuss here at the Science of Parkinson’s. It is loosely defined as being ‘diagnosed with Parkinson’s disease under the age of 20’. The prevalence is unknown, but there is a strong genetic component to form of the condition. In today’s post we will review what is known about Juvenile-onset and look at new research about a gene that has recently been discovered to cause a type of Juvenile-onset Parkinson’s disease.

Dr Henri Huchard. Source: Wikipedia
In 1875, Dr Henri Huchard (1844-1910; a French neurologist and cardiologist) described the first case of a child who, at just 3 years of age, presented all the clinical features of Parkinson’s disease. Since that report, there have been many studies detailing the condition that has become known as ‘juvenile-onset Parkinson’s disease’.
What is juvenile-onset Parkinson’s disease?
Basically, it is a form of Parkinson’s disease that affects children and young people under the age of 20. The defining feature is the age of onset. The average age of onset is approximately 12 years of age (with the majority of cases falling between 7 and 16 years) and males are affected by this condition more than females (at a rate of approximately 5:1).
The actual frequency of juvenile-onset parkinson’s is unknown given how rare it is. When researcher look at people with early onset Parkinson’s disease (that is diagnosis before the age of 40; approximately 5% of the Parkinson’s community), they have found that between 0.5 – 5% of that group of people were diagnosed before 20 years of age. This suggests that within just the Parkinson’s community, the frequency of juvenile-onset parkinson’s is at the most 0.25% (or 2.5 people per 1000 people with Parkinson’s). Thus it is obviously a very rare condition.
It is interesting to note that Lewy bodies (the clusters of aggregated protein that classically characterise the brains of people with Parkinson’s disease) are very rare in cases of juvenile-onset parkinson’s disease. To our knowledge there has been only one case of Lewy bodies in juvenile-onset parkinson’s disease (Click here to read more on this). This suggests that the juvenile-onset form of Parkinson’s disease may differ from other forms of the condition in its underlying biology.
Do we know what causes juvenile-onset parkinson’s disease?
There is a very strong genetic component to juvenile-onset parkinson’s disease. In fact, the incidence of Parkinsonism in relatives of people with juvenile-onset parkinson’s disease is higher than in the general public AND in the relatives of people with other forms of Parkinson’s disease.
Genetic mutations in three genes are recognised as causing juvenile-onset Parkinson’s disease. The three genes are known to the Parkinson’s world as they are all PARK genes (genetic variations that are associated with Parkinson’s). Those three genes are:
- Parkin (PARK2)
- PTEN-induced putative kinase 1 (PINK1 or PARK6)
- DJ1 (PARK7)
In juvenile-onset Parkinson’s disease, all of these mutations are associated with autosomal recessive – meaning that two copies of the genetic variation must be present in order for the disease to develop.
Parkin mutations account for the majority of juvenile-onset Parkinson’s disease cases. Affected individuals have a slowly progressing condition that is L-dopa responsive. Dystonia (abnormal muscle tone resulting in muscular spasm and abnormal posture) is very common at the onset of the condition, particularly in the lower limbs.
Can the condition be treated with L-dopa?
The answer is: ‘Yes, but…’
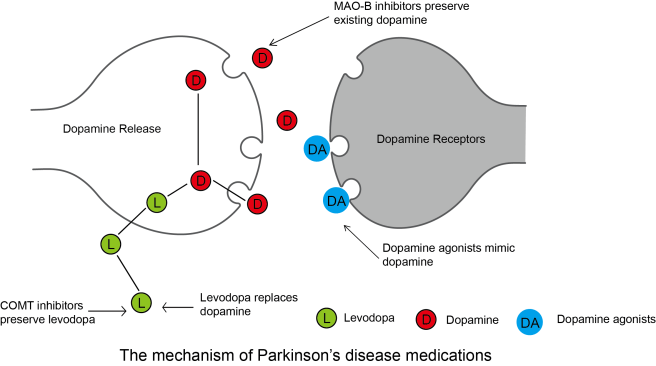
L-dopa (or dopamine replacement) treatment is the standard therapy for alleviating the motor features of Parkinson’s disease.
The majority of people with juvenile-onset parkinson’s respond well to L-dopa, but in the Parkin mutation version individuals will typically begin to experience L-dopa-induced motor fluctuations (dyskinesias) early in that treatment regime.
What research is currently being done on this condition?
Given that cases are so very rare and so few, it is difficult to conduct research on this population of individuals. Most of the research that is being conducted is focused on the genetics underlying the condition.
And recent that research lead to the discovery of a new genetic variation that causes juvenile-onset Parkinson’s disease:

Title: Discovery of a frameshift mutation in podocalyxin-like (PODXL) gene, coding for a neural adhesion molecule, as causal for autosomal-recessive juvenile Parkinsonism.
Authors: Sudhaman S, Prasad K, Behari M, Muthane UB, Juyal RC, Thelma BK.
Journal: Journal Med Genet. 2016 Jul;53(7):450-6.
PMID: 26864383 (This article is OPEN ACCESS if you would like to read it)
The researchers who wrote this article were presented with a 10 member Indian family from Aligarh, Uttar Pradesh. Of the 8 children in the family, 3 were affected by Parkinsonian features (tremor, slowness, rigidity and gait problems) that began between 13 and 17 years of age. The researchers conducted DNA sequencing and found that none of the three affected siblings had any of the known Juvenile-onset Parkinson’s disease genetic mutations (specifically, mutations in the genes PARK2, PINK1and DJ1).
They then compared the DNA from the three siblings with the rest of the family and found a genetic variant in a gene called podocalyxin-like (or PODXL). It must be noted that PODXL is a completely novel gene in the world of Parkinson’s disease research, which makes it very interesting. PODXL has never previously been associated with any kind of Parkinson’s disease, though it has been connected with two types of cancer (embryonal carcinoma and periampullary adenocarcinoma).
The researchers then turned to their genetic database of 280 people with Parkinson’s disease have had their genomes sequenced. The researchers wanted to determine if any genetic variants in the PODXL gene were present in other suffers of Parkinson’s disease, but had not been picked up as a major contributing factor. They found three unrelated people with PODXL mutations. All three had classical Parkinson’s features, and were negative for mutations in the Parkin, PINK1 and DJ1 genes.
The researchers concluded that the PODXL gene may be considered as a fourth causal gene for Juvenile-onset Parkinson’s disease, but they indicated that further investigations in other ethnic groups are required.
The banner for today’s post was sourced from ClipArtBest