|
“In current models of neurodegeneration, individual diseases are defined by the presence of one or two pathogenic protein species. Yet, it is the rule rather than the exception that a patient meets criteria for more than one disease” These are the first lines of a manuscript on the preprint sharing webiste BioRxiv, which analysed the co-occurance of biological markers of Alzheimer’s or Parkinson’s or other neurodegenerative conditions across 18 brain regions in 1389 postmortem brain from people who passed away with a neurodegenerative condition. The results are interesting. In today’s post, we will discuss what this study did, what is meant by “transdiagnostic disease clusters”, and consider what could they mean for our understanding of Parkinson’s… and heck, neurodegenerative conditions in general.
|
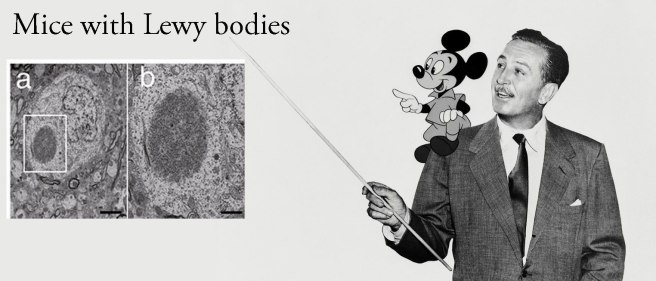
 Malcolm Gladwell. Source: Masterclass
Malcolm Gladwell. Source: Masterclass
I am a fan of Malcolm Gadwell (not an endorsement, this is just me sharing).
He has a great way of looking at a situation from a completely different angle, finding things that no one else sees, and then writing about it in a clever, easy to read manner. Having read most of his books, I was rather pleased to learn that he has a podcast – Revisionist History.
And it’s good.
Oh boy, it’s good.
The first episodes of the most recent series of the podcast have helped to raise my fragile self esteem, because I am definitely a tortoise (just listen to the first two episodes of season 4 and you’ll understand).
Oh, and Mr Gladwell, if you ever read this – in the next series of the podcast, please have a look at the dysfunctional way we clinically test new therapies in medicine – click here to read a previous SoPD rant on this topic. Thanks!
What does Malcolm Gladwell have to do with Parkinson’s?
It all comes back to that idea of looking at a situation from a completely different angle.
What do you mean?