|
On Tuesday 21st December, 1824, James Parkinson passed away in his home – two days after suffering a stroke. It was the end of an amazing and extremely productive life. In this post about James Parkinson – the final in the series of four observing the 200th anniversary of his first observation of Parkinson’s disease – we look at what happened following his death, and reflect on his overall legacy. |
St Leonard’s church in Hoxton, London – James’ church
At the end of the third post on the life of James Parkinson (Click here to read that post), the Battle of Waterloo had just occurred and James was publishing the last of his writings.
One of the last major events in the life of James Parkinson occurred in 1823, when James was awarded the Royal College of Surgeons’ first Gold Medal.
Understand that this was a big deal.
The college had established the award way back in 1802 for “distinguished labours, researches and discoveries”. But it took them a full 21 years to find anyone that they thought worthy enough to be the first recipient.
And that first recipient: one James Parkinson
This event, however, represents very nicely how the legacy of James has changed over time. While the world currently associates James Parkinson with a neurological condition that he first described in 1817, the Royal College of Surgeons awarded him their first gold medal not for any of his medical publications, but rather for his “splendid Work on Organic Remains”.

Source: Lindahall
As I have written before, James was a bit of a rockstar to the geological/palaeontology community. His writings on what he called his “favourite science”, had earned him an international reputation and one has to wonder how he would feel now if he knew that his reputation lies elsewhere.
As JP aficionado Dr Cherry Lewis once wrote: history is fickle.
His final days
In that same year as receiving the Royal College of Surgeons’ gold medal (1823), James and Mary Parkinson moved to no.3 Pleasant Row, Kingsland Road (Hoxton) with their unmarried daughter, Mary. It appears to have been a ‘house-swap’ as James’s son John WK Parkinson had been living at no.3 Pleasant Row and subsequently moved into no.1 Hoxton Square. James is believed to have largely retired from his medicinal practice with this move.
No.3 Pleasant Row, Kingsland Road (Hoxton). Source: Searching4James
On Sunday 19th December, 1824 – just 4 months shy of his 70th birthday – James suffered a major stroke (possibly associated with his years of gout) which left him unable to speak and confined to his bed. Two days later, on Tuesday 21st December, 1824, James Parkinson died at 10am at his home.
Given that James was the parish surgeon, his son, John WK Parkinson wrote to the Board of Trustees of the Parish to inform them of his passing. His letter was entered into the minutes of the Board meeting, on the 23rd December, 1824:
Gentleman,
With feelings of deep regret I have to announce to you the death of much beloved and respected father.
He was suddenly attacked on Sunday afternoon with a severe paralytic affection which deprived him of his speech and of the use of his right side. Every means were employed for his recovery, but they proved to no avail – and he expired on Tuesday morning at half past ten o’clock.
I have the honour to be, Gentlemen,
Your most obediant servant
J.W.K. Parkinson
(Source: Morris, 1989)
James was buried on the 29th December by Rev. Robert Crosby, curate of at his local church, St Leonard’s – the place where he had been both baptised and married. His burial is noted in the register:
Image from Stern (2014)
If you go looking for the grave of James at St Leonards today, you will not find it.
With the expansion of London, there were significant re-developments of the land around the church and many of the coffins were dug up and transferred to a space beneath the nave of St Leonards. James is most likely there – and he would be easy to find as most of the coffins in that age had metal name plates attached.
Enough of this morbid talk.
In the absence of a grave in the gardens of St Leonard’s, on the 17th November, 1955 there was a ceremony at the church at which a memorial marble plaque was unveiled in honour of James Parkinson to commemorate the bicentennial of his passing. You can find it inside the church on the north-east wall. It reads:
‘In Piam Memoriam – James Parkinson of Hoxton, Surgeon and Apothecary, Diplomate of the Company of Surgeons, Member and the First Honorary Medallist of the Royal College of Surgeons. In his ‘Essay on the Shaking Palsy’ he first described the disease since known by his name. Founder member of the Geological Society of London and author of ‘Organis Remains of a Former World’. Honorary Medallist of the Royal Humane Society. Political and Social Reformer. Born at 1 Hoxton Square 11 April 1755, where he practised for forty years. Died at 3 Pleasant Row, Hoxton, 21 December 1824. Baptized and married in this Church, and buried in the Churchyard. A life long worshipper at the Parish Church. Erected by the nursing staff of St Leonard’s Hospital.’
The memorial plaque at St Leonard’s Church (Shoreditch)
The Essay – after James
It is often said that An Essay on the Shaking Palsy – the work by which James is remembered the most – was largely ignored by the medical profession during the first few years following its publication. This is not entirely true. In the year of its publication, the essay was reviewed in the Swedish medical press (Ars-Berättelse om Svenska Läkare-Sällskapets Arbeten 91; Stockholm, 1817), and within the next few years it was mentioned numerous times.
John Cooke. Source: Wikipedia
Physician John Cooke wrote of “a disease … lately described by Mr Parkinson under the title paralysis agitans or shaking palsy as highly deserving of attention” (Cooke, J. in A Treatise on Nervous Diseases. History and Method of Cure of the Various Species of Palsy. Vol. 2 207 – from Longman, 1821).
Marshall Hall. Source: Wikipedia
And Marshall Hall considered paralysis agitans as “well described by Mr Parkinson” (Hall, M. in On the Diseases and Derangements of the Nervous System, in their Primary Forms and in their Modifications by Age, Sex, Constitution, Hereditary Predisposition, Excesses, General Disorder, and Organic Disease 320 – from Baillière, 1841).
Thus, it does appear that the Essay was well read the medical establishment during the years after its publication.
The naming of Parkinson’s disease?
A common source of debate in the story of James Parkinson is who actually used the label ‘Parkinson’s disease’ first. It certainly wasn’t James, who preferred the title ‘paralysis agitans’.
‘Parkinson’s disease’ was first coined by a Scottish physician and pathologist named William Rutherford Sanders (1828–1881) who wrote a case study in the Edinburgh Medical Journal in 1865.
William Rutherford Sanders (1828–1881). Source: Nationalgalleries
In his article, Sanders wrote a case report about a 35 years old individual who had a marked tendency to shake and a propensity to bend the trunk forwards. Sanders referred to this condition as “Parkinson’s disease”. He emphasised that the tremor was the main feature, along with gait issues. He disagreed with James in that he thought that the label ‘paralysis’ was wrong. The condition was not a matter of weakness but rather slowness of movement.
This was a full 10 years before Charcot introduced ‘maladie de Parkinson‘ – for which he generally gets the credit of naming ‘Parkinson’s disease’.
For those who work in the field of neurology, Jean-Martin Charcot requires absolutely no introduction.
Jean-Martin Charcot (Source: Wikipedia)
Widely considered the ‘Father of neurology’, the importance of Charcot’s contribution to modern medicine is rarely in doubt. One only needs to read the names of the students that he taught at the famous Salpêtrière Hospital (in Paris) to appreciate that everyone who became someone in the field of Neurology passed through his classes.
Those names include Sigmund Freud (the founder of psychoanalysis), Joseph Babinski, Pierre Janet, Pierre Marie, Albert Londe, Charles-Joseph Bouchard, Georges Gilles de la Tourette, Alfred Binet (inventor of the first intelligence test), and Albert Pitres. Even the great William James – one of the founding fathers of Psychology – travelled all the way from America just to sit in Charcot’s classes.
Charcot was one of the most revered instructors in all of Europe, immortalised in a painting by André Brouillet:
A Clinical Lesson at the Salpêtrière (“Une leçon clinique à la Salpêtrière“)
by André Brouillet (Source: Wikipedia)
Between 1868 and 1881, Charcot focused much of his attention on the condition that would become Parkinson’s disease. Like Sanders, Charcot rejected the label ‘Paralysis Agitans’, suggesting that the former was misleading in that patients were not markedly weak and do not necessarily have tremor (Charcot, 1872). Rather than Paralysis Agitans, Charcot suggested that Maladie de Parkinson (or Parkinson’s disease) would be a more appropriate name, bestowing credit to the man who first described the condition.
Charcot made quite a habit of naming conditions after other people, as in the case of Tourette’s syndrome which he named after one of his own students (Georges Gilles de la Tourette). George had been using the name ‘maladie des tics‘ to describe the nine patients he had been studying. Charcot obviously had an eye for political correctness well before its time.
One of Charcot’s major contributions to the study of Parkinson’s was to differentiate this condition from other disorders, such as multiple sclerosis. He and his students then identified different variants of the condition, which were termed ‘Parkinson’s disease without tremor’, ‘Parkinson’s disease with extended posture’, and ‘Parkinson’s disease with hemiplegia’ (a condition that affects one side of the body).
Charcot was also one of the first doctors to propose a therapy for Parkinson’s… though it is not clear exactly how effective it was. It was called vibratory therapy, and it basically involved shaking the individual.
Vibratory therapy. Source: NCBI
Charcot had noticed that people with Parkinson’s experienced a reduction in their resting levels of tremor during and after taking a carriage ride. He speculated that the vibrations of the experience may have been the beneficial factor. A vibratory helmet which shook the head and brain was later developed, but again it is not clear how successful these first steps at a remedy were.
The development of Parkinson’s
After Charcot, there is a long list of researchers who picked up the Parkinson’s batten and ran with it. Principle among the first of them was William Gowers.
William Gowers. Source: Wikipedia
Working in James’ home town of London, Gowers was one of the first to contribute a study of demographics to Parkinson’s disease in his “Manual of Diseases of the Nervous System”. The data was collected from his personal experience with over 80 people with Parkinson’s in the 1880s. He was also one of the first to identify the slight male predominance in the condition, and he offered one of the most memorable comments regarding Parkinson’s associated tremor:
‘The movement of the fingers at the metacarpal-phalangeal joints is similar to that by which Orientals beat their small drums’
Gowers is also remembered for his famous postural drawings of people with the condition:
Drawing by Gowers from 1886. Source: Wikipedia
Research on Parkinson’s soon shifted from the clinic to the laboratory. In 1912, just two years out of medical school, neuropathologist Friedrich Lewy published his findings from analysing postmortem sections of brain from people who passed away with Parkinson’s.
Friedrich Lewy. Source: Lewy Body Society
Based on the examination of 25 patients with Parkinson’s, Lewy had observed disease-specific features in a region of the brain called the dorsal nucleus of the vagus nerve (he didn’t look at the substantia nigra). The dorsal nucleus of the vagus nerve is a collection of cells that resides in the brain stem (at the base of the brain) and it receives signals from the heart, lungs and stomach.
Source: oerpub.github
Lewy reported that a ‘large number‘ of the samples from patients with Parkinson’s who showed ‘tremor and tension of their vocal cords‘, displayed small, dense circular objects inside the cells of the dorsal nucleus of the vagus nerve. He had not found any of these same features in six cases of ‘severely senile or arteriosclerotic‘ patients.
These objects were later called “Lewy bodies” – named by Russian neuropathologist Konstantin Tretiakoff in 1919 (Source).
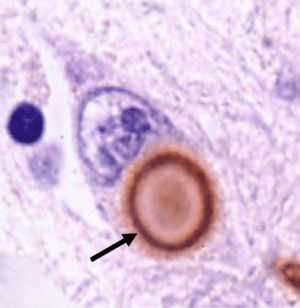
A lewy body (stained brown, indicated with a black arrow) inside a cell. Source: Cure Dementia
Tretiakoff also the first to notice one of the cardinal features of the Parkinsonian brain. In his thesis, he described the loss of pigmented cell in the substantia nigra (the regions of the brain where the ‘pigmented’ dopamine producing neurons reside) based on observations from postmortem brains of people who passed away with Parkinson’s.
During the first half of the 20th century, little occurred with regards to Parkinson’s research. There was the discovery of a chemical called dopamine, but no one really knew anything about it until a young Swedish research named Arvid Carlsson started to play with it.

Prof Arvid Carlsson. Source: Alchetron
In 1957, Carlsson discovered that when he injected a neurotoxin (reserpine) into the brains of rabbits, it killed the dopamine neurons and the animals exhibited limited movement. He also discovered that by injecting the dopamine precursor –L-dopa – into those same animals, he was able to rescue their motor ability. Importantly, he found that the precursor (called 5-hydroxytryptophan) to another chemical called serotonin, it was not capable of reversing the reduction in motor ability, indicating that the effect was specific to L-dopa.
He published this amazing discovery in a 1957 research report:

Title: 3,4-Dihydroxyphenylalanine and 5-hydroxytryptophan as reserpine antagonists.
Authors: Carlsson A, Lindqvist M, Magnusson T.
Journal: Nature. 1957 Nov 30;180(4596):1200. No abstract available.
PMID: 13483658 (the article on the Nature website – access required)
This was a fantastic discovery.
A Nobel prize winning discovery in fact.
But what to do with it? At the time, the depletion of dopamine in Parkinsonian brain was unknown. It was not until 1960 that that critical discovery of Parkinson’s disease was made by another young European scientist. Carlsson’s research (and that of others) inspired the Austrian researcher, Oleh Hornykiewicz, to look at dopamine levels in people with Parkinson’s disease.
And what he found changed everything.

Prof Oleh Hornykiewicz. Source: Kurienwissenschaftundkunst
In his study, Hornykiewicz found very high levels of dopamine in the basal ganglia of normal postmortem adult brains, but a marked and consistent reduction (approx. 10-fold) in six postmortem cases of Parkinsonisms. The basal ganglia is one of the main regions of the brain in which dopamine neurons release the bulk of their dopamine.
He published this result in this report:

Title: Distribution of noradrenaline and dopamine (3-hydroxytyramine) in the human brain and their behavior in diseases of the extrapyramidal system
Authors: Ehringer H, Hornykiewicz O.
Journal: Parkinsonism Relat Disord. 1998 Aug;4(2):53-7. No abstract available.
PMID: 18591088
Importantly, Hornykiewicz did not stop there.
In November 1960, Hornykiewicz approached Walther Birkmayer, a doctor at a home for the aged in Vienna, and together they began some clinical trials of L-dopa in July 1961. Birkmayer injected 50 to 150 mg in saline intravenously into 20 volunteers with Parkinson’s.
In their report, Birkmayer and Hornykiewicz wrote this regarding the results:
“The effect of a single intravenous injection of l-dopa was, in short, a complete abolition or substantial relief of akinesia. Bedridden patients who were unable to sit up, patients who could not stand up when seated, and patients who when standing could not start walking performed after l-dopa all of these activities with ease. They walked around with normal associated movements, and they could even run and jump. The voiceless, aphonic speech, blurred by palilalia and unclear articulation, became forceful and clear as in a normal person. For short periods of time the people were able to perform motor activities, which could not be prompted to any comparable degree by any other known drug”
Despite their initial excitement, Birkmayer and Hornykiewicz found that the response to L-dopa was very limited in its duration. In addition, subsequent trials by others were not able to achieve similar results, with many failing to see any benefit at all.
And that was when George stepped into the picture.

Dr George Cotzias…and uh, yes he is holding a brain. Source: New Scientist
Dr George Cotzias was a physician working in New York who became very interested in the use of L-dopa for Parkinson’s. And he discovered that by starting with very small doses of L-dopa, given orally every two hours and gradually increasing the dose gradually he was able to stabilise patients on large enough doses to cause a dramatic changes in their symptoms. His studies led ultimately to the US Food and Drug Administration (FDA) approving the use of L-dopa for use in PD in 1970. Cotzias and his colleagues were also the first to describe L-dopa–induced dyskinesias.
And these were just some of the consequences caused by the writings of a busy surgeon living at no.1 Hoxton Square 200 years ago. For an excellent and more thorough review of the history of Parkinson’s disease, I can recommend this review.
The legacy of James
It is interesting to read the Bulletin of John Hopkins Hospital article written by Prof Leonard George Rowntree about James Parkinson. Rowntree knew more about JP than most, and he travelled to London in search of details about the man. In the the final two paragraphs, he gives a very sober assessment of our man James:
What then did Parkinson accomplish during his life? He cannot be considered a brilliant investigator and certainly he made no startling contributions to science. He was a man of the Old Master type described by Holmes rather than the highly specialized scarabaeist. Master of medicine, chemistry, geology, paleontology and oryctology, he was a writer of many textbooks, great as a compilator, keen in observation and desirous of seeing everything named and placed in its proper class. His most important contribution to medicine was the offsprint of the last two qualities.
NOTE: The Holmes that Rowntree is referring to is not of the ‘Sherlock’ variety, but the ‘Oliver Wendell’ kind. In the third of his “Breakfast-table” series, Holmes introduces a man who is spending his entire life studying beetles. But that man rejects the title “entomologist” (a person who studies insects) and prefers to be called a “Scarabaeist” (a person who studies the beetle family Scarabaeidae).
Back to Rowntree:
He was a member of the Geological Society of London, the Wernerine Society of Edinburgh, and of the Caesarian Society of Moscow, a Fellow of the Royal College of Surgeons. ‘Tis true his chief contributions to medicine consisted simply in describing a disease and giving it a name, thereby establishing it as a clinical entity. It may be argued that he neither discovered its etiology nor found a cure; but the disease has stood an open challenge to investigators for a full century. “Let him that is without sin cast the first stone”
Coming from someone who spent a considerable amount of time reading James’s works and researching his past, this conclusion is rather remarkable. But then, so was Prof Rowntree.
To finish – and in keeping with the theme of using the writings of others to fill space – I will give the last words to JP. On the last page of An Essay on the Shaking Palsy, James wrote this:
Before concluding these pages, it may be proper to observe once more, that an important object proposed to be obtained by them is, the leading of the attention of those who humanely employ anatomical examination in detecting the causes and nature of diseases, particularly to this malady. By their benevolent labours its real nature may be ascertained, and appropriate modes of relief, or even of cure, pointed out.
James Parkinson (1817)
The banner for today’s post was sourced from Parkinsonfonds
















Interesting – a good read as they say.
LikeLike