|
A reader recently asked for an explanation of some recent research regarding diabetes and Parkinson’s. You see, a significant proportion of the Parkinson’s community have glucose intolerance issues and some live with the added burden of diabetes. That said, the vast majority of diabetics do not develop PD. Likewise, the vast majority of people with Parkinson’s do not have a diagnosis of diabetes. There does appear to be a curious relationship between Parkinson’s and diabetes, with some recent research suggests that this association can be detrimental to the course of the condition. In today’s post we will look at what what diabetes is, consider the associations with Parkinson’s, and we will discuss the new research findings. |
Foreman and Ali. Source: Voanews
1974 was an amazing year.
On October 30th, the much-hyped heavyweight title match – the ‘Rumble in the Jungle’ – between George Foreman and Muhammad Ali took place in Kinshasa, Zaire (Democratic Republic of the Congo).
Stephen King. Source: VanityFair
A 26-year-old author named Stephen King published his debut novel, “Carrie” (April 5, with a first print-run of just 30,000 copies).
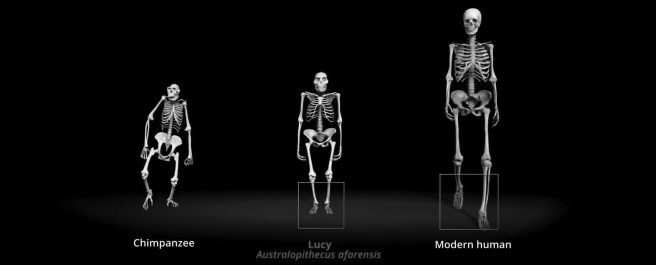
Lucy. Source: Youtube
The fossil remains of a 3.2 million years old hominid skeleton was discovered in Ethiopia (November 24th). It was named ‘Lucy’ – after the song “Lucy in the Sky with Diamonds” by The Beatles which was played repeatedly in the expedition camp the evening after the team’s first day of work on the site (Source).
And Richard Nixon becomes the first US president to resign from office (August 9th).
President Richard Nixon. Source: Fee
In addition to all of this, in December of 1974, a small study was published in the Journal of Chronic Diseases.
It dealt with Parkinson’s and it presented a rather startling set of findings:
Title: Glucose intolerance in Parkinson’s disease.
Authors: Lipman IJ, Boykin ME, Flora RE.
Journal: J Chronic Dis. 1974 Dec;27(11-12):573-9.
PMID: 4436423
In the study, Lipman and colleagues conducted some routine glucose tolerance tests on a group of 56 people with Parkinson’s (7 additional subjects with Parkinson’s were excluded because they had been previously diagnosed with diabetes).
After being asked to fast overnight, the subjects were then given 100g of glucose and blood samples were collected from them every hour for 3 hours. When the glucose levels in the blood were measured and compared with the results of 5 previous studies conducted on normal healthy adults of the same age (one of those studies involved 7000 participants), it was found that the people with Parkinson’s in the Lipman study had a much higher average level of glucose in their blood than all of the other 5 studies looking at healthy individuals.
Shockingly, almost half (46.4%) of the participants in the Lipman study actually fulfilled the criteria for a diagnosis of diabetes.
More recent survey data has revealed that diabetes is established in between 8–30% of people with Parkinson’s (click here for more on this) – obviously this is well in excess of the approximately 6% prevalence rate in the general public (Source: DiabetesUK).
What is diabetes?
Source: Vailranchpharmacy
Diabetes (or ‘Diabetes mellitus’) is basically a group of metabolic diseases that share a common feature: high blood sugar (glucose) levels for a prolonged period.
There are three types of diabetes:
Source: Cdc
In all three cases of diabetes, a protein called insulin plays an important role.
What is insulin?
Insulin is a protein (actually a hormone) that our body makes, which allows us to use sugar (‘glucose’) from the food that you eat.
Insulin. Source: Wikipedia
Glucose is a great source of energy for the cells in our bodies. After eating food, our body releases insulin which then attaches to cells and signals to those cells to absorb the glucose from our bloodstream. Without insulin, our cells have a hard time absorbing glucose. Think of insulin as a “key” which unlocks cells to allow glucose to enter the cell.
How does insulin relate to diabetes?
Let me introduce you to your pancreas.
It lies beside your stomach, under your liver – close to your gallbladder (which we recently discussed in a previous post):
The location of your pancreas. Source: WebMD
In your pancreas, you have beta cells.
The primary function of a beta cell is to store and release insulin. When there is a spike in levels of glucose in the blood (for example, after a piece of candy), beta cells respond quickly by secreting some of their stored insulin and simultaneously producing more.
In a healthy situation, the pancreas will happily produce and secrete insulin – no questions asked. In type 1 diabetes, however, the pancreas cannot or does not produce any insulin. This results in the need for insulin treatment for survival. Type 1 diabetes is considered an autoimmune condition, which means your immune system attacks healthy body tissue by mistake. In type 1 diabetes, the immune system specifically attacks the insulin-producing beta cells in the pancreas.
Source: Ghr
In type 2 diabetes, your body still breaks down your food and absorbs the glucose, which the pancreas responds to by releasing insulin. But in type 2 diabetes, the cells in your body do not respond adequately to normal levels of insulin. This situation is referred to as insulin resistance.
What is insulin resistance?
Insulin resistance occurs when the cells of your body stop recognising and responding to insulin. This situation prevents glucose from entering the cells where it can be used as energy. Blocked from entering cells, glucose levels in the blood start to rise. When the pancreas detects these rising levels of glucose in the blood, it keeps on producing insulin in an attempt to reduce those levels of glucose.
Insulin resistance. Source: Cystersoftheheart
Over time, however, the beta cells in the pancreas become less able to respond to blood sugar levels. This will lead to an insulin shortage, which will result in a build up of blood glucose levels, which can lead to hyperglycemia. When the glucose levels start building in the blood, this is referred to as glucose intolerance.
But understand that not all people with insulin resistance develop diabetes. In fact, most of the population will have some level of insulin resistance as they naturally age – adequate exercise and healthy living can help to keep this under control.
High levels of insulin and glucose in the blood, however, can cause the liver to go into overdrive, which results in a decrease in other liver functions, such as lipid (fat) digestion resulting in “fatty liver” and sometimes cirrhosis (or scarring) of the liver.
If nothing I have written regarding type 2 diabetes make any sense, this video will hopefully help:
Ok, so what does diabetes have to do with Parkinson’s?
As mentioned above, between 10–30% of the Parkinson’s community are glucose intolerant.
Why?
Source: Wellbeing365
There have, however, been numerous studies now that have suggested an association between diabetes and Parkinson’s.
The first of these studies was:

Title: Prospective cohort study of type 2 diabetes and the risk of Parkinson’s disease.
Authors: Driver JA, Smith A, Buring JE, Gaziano JM, Kurth T, Logroscino G.
Journal: Diabetes Care. 2008 Oct;31(10):2003-5.
PMID: 18599528
In this study, 21,841 male doctors (participants in the Physicians’ Health Study) were followed over 23 years. The researchers found that people with diabetes had an increased risk of developing Parkinson’s risk. Interestingly, they reported that the highest Parkinson’s risk was seen in individuals with short-duration, older-onset diabetes.
In another study:

Title: Diabetes and risk of Parkinson’s disease.
Authors: Xu Q, Park Y, Huang X, Hollenbeck A, Blair A, Schatzkin A, Chen H.
Journal: Diabetes Care. 2011 Apr;34(4):910-5. doi: 10.2337/dc10-1922. Epub 2011 Mar 4.
PMID: 21378214
This study came from another long term study, which was following 288,662 participants of the National Institutes of Health-AARP Diet and Health Study. The researchers found that the risk of Parkinson’s was approximately 40% higher among diabetic patients than among participants without diabetes. In this study, however, the analysis showed that the risk was largely limited to individuals who had diabetes for more than 10 years.
A third study:
Title: Diabetes and the risk of developing Parkinson’s disease in Denmark.
Authors: Schernhammer E, Hansen J, Rugbjerg K, Wermuth L, Ritz B.
Title: Diabetes Care. 2011 May;34(5):1102-8.
PMID: 21411503
Using data from the nationwide Danish Hospital Register hospital records, the researchers found that having diabetes was associated with a 36% increased risk of developing Parkinson’s. Interestingly, they reported that the risk was stronger in women and people with early-onset Parkinson’s (eg. diagnosed before the age of 60 years).
All of this research suggests that diabetes increases the risk of Parkinson’s, right?
No it doesn’t. Association does not equal causation.
And please understand that there is a lot of debate about this relationship between diabetes and Parkinson’s.
In fact, if you only look at the ‘case-controlled’ studies that have investigated this relationship…. there is no increase in risk. In fact there may be a decreased risk!
Que?
A few years ago, some researchers in China published this research report:

Title: Diabetes and risk of Parkinson’s disease: an updated meta-analysis of case-control studies.
Authors: Lu L, Fu DL, Li HQ, Liu AJ, Li JH, Zheng GQ.
Journal: PLoS One. 2014 Jan 21;9(1):e85781.
PMID: 24465703 (This article is OPEN ACCESS if you would like to read it)
In this meta-analysis, the researchers collected all of the data from 14 case-controlled studies looking at whether diabetes increased the risk of Parkinson’s.
What does ‘case-controlled’ mean?
Case-controlled studies are retrospective. They involve two clearly defined groups: one with the outcome/condition and one without the outcome/condition. They then look back into the (medical) past to assess whether there is a statistically significant difference in the rates of an event occurring between the groups. Case-controlled studies should involve two groups that are identical EXCEPT for their outcome.
Case controlled study. Source: Students4bestevidence
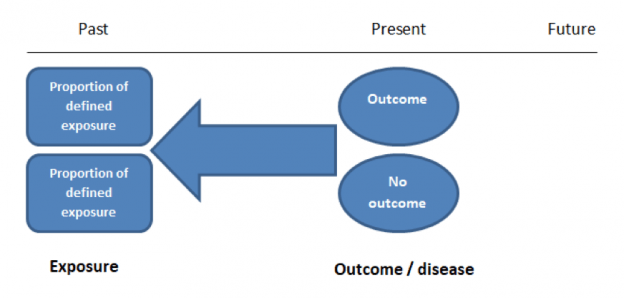
This is different to a ‘cohort study’ which can be retrospective or prospective, but usually involves following a large group of individuals and comparing outcomes based on exposures (think of the Honulu Heart study – Click here to read more about that). A cohort studies should include two groups that are identical EXCEPT for their exposure status.
Source: Students4bestevidence
Importantly, case-controlled studies are better for very rare events, such as determining whether a condition like diabetes increases the risk of developing Parkinson’s.
When the researchers looked at the results of the 14 case-controlled studies (which involved 21395 cases of Parkinson’s and 84579 control subjects), they found that people with diabetes actually have a 25% reduction in their risk of developing Parkinson’s.
Here are all of the studies used in this analysis:
Source: PLOS
This does not mean that diabetes could still be a risk factor for future Parkinson’s, but this result has also been supported by a similar analysis (Click here to read that research report).
All of that said, a different recent meta-analysis of 7 population-based cohort studies (involving 1,761,632 individuals) suggested that diabetes is associated with a 38% increased risk of developing Parkinson’s (Click here to read more about this research).
Like I said, a lot of debate about this issue.
Ok, but if you are diabetic, what happens with your Parkinson’s?
Last week a research report was published that looked at this very topic:
Title: Diabetes mellitus and Parkinson disease
Authors: Pagano G, Polychronis S, Wilson H, Giordano B, Ferrara N, Niccolini F, Politis M.
Journal: Neurology. 2018 Apr 6. pii: 10.1212
PMID: 29626177
In this study, the researchers identified 25 individuals with early, drug-naive Parkinson’s with diabetes and compared them to 25 individuals with early, drug-naive Parkinson’s without diabetes, as well as 14 control subjects who had diabetes but no Parkinson’s and 14 healthy controls. They then followed up these groups for 36 months to determine if diabetes in the Parkinson’s-affected groups was associated with faster motor progression or cognitive decline.
They found that the combination of Parkinson’s and diabetes was associated with higher motor scores, lower dopamine transporter binding (on brain imaging) and faster cognitive decline. This result caused the investigators to conclude that diabetes “can induce a more aggressive phenotype” (or form) of Parkinson’s.
Interestingly, in people with diabetes but without Parkinson’s, there was a lower level of dopamine transporter binding (brain imaging) compared to healthy controls. This led the researchers to conclude that diabetes “may predispose” individuals “toward a PD-like pathology”.
The investigators were quick to point out, however, that “the causation between diabetes and PD, the link between insulin resistance and PD, and the potential beneficial effect of novel anti-diabetic drugs need further investigation”.
But these findings are supported by previous research suggesting that diabetes is associated with gait difficulty, cognitive decline, and faster motor progression in Parkinson’s (Click here, here and here to read more about this).
How could this poorer outcome be occurring?
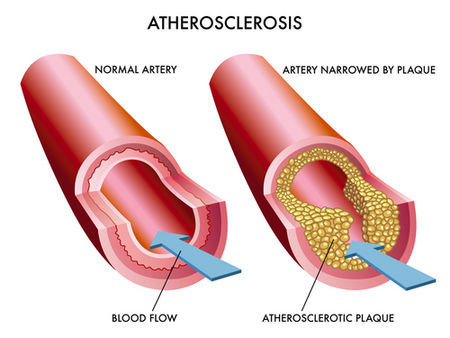
Diabetes is associated with small and large vessel ‘atherosclerosis’ – a condition where plaque builds up inside the arteries.
Atherosclerosis. Source: Drterrywillard
This outcome could lead to what is referred to as ‘vascular parkinsonism‘ rather than a classical form of Parkinson’s (Click here to read a previous SoPD post on vascular Parkinsonism). Or this vascular effect could be a influential in the progression of normal PD – this is yet to be determined though.
But there is one aspect of all this research that I do not understand.
Which is?
In 2016, an interesting research report was published in the journal Movement disorders:

Title: Reduced incidence of Parkinson’s disease after dipeptidyl peptidase-4 inhibitors-A nationwide case-control study.
Authors: Svenningsson P, Wirdefeldt K, Yin L, Fang F, Markaki I, Efendic S, Ludvigsson JF.
Journal: Movement Disorders 2016 Jul 19.
PMID: 27431803
In this study, the investigators used the Swedish Patient Register, to find the medical records of 980 people who were diagnosed with Parkinson’s but also had type 2 diabetes. Importantly, all of the subjects had been treated with type 2 diabetes medication for at least 6 months prior to the date of Parkinson’s being diagnosed.
For comparative sake, they selected 5 controls (non-Parkinsonian) with Type 2 diabetes (n = 4,900) for each of their Parkinsonian+diabetes subjects. They next looked at whether GLP-1R agonists (such as Exenatide), Dipeptidyl peptidase-4 (or DPP-4) inhibitors, or any other oral Type 2 diabetic medication can influence the incidence of Parkinson’s.
Now, if all things are considered equal, then when looking at each diabetes medication there should be 1 person in the Parkinson’s + type 2 diabetes for every 5 people in the Type 2 diabetes control group taking each medication right? That is because there are almost 1000 people in the first group and 5000 in the second group.
But this is not what the researchers found.
Early use of GLP-1R agonists was seen in just 1 person with Parkinson’s + type 2 diabetes and 7 type 2 diabetes controls. Given the low number of people using this class of drug, the investigators were reluctant to conclude very much from this result. BUT the really interesting discovery was that early use of DPP-4 inhibitors was seen in 3 people with Parkinson’s disease + Type 2 diabetes and 64 Type 2 diabetes controls.

Sitagliptin (DPP-4 inhibitor). Source: Diabetesmedicine
I think you’ll agree that a 3:64 (or 1:21) ratio is slightly larger than a 1:5 ratio. If all things were equal, then there should have been at least 12 people with Parkinson’s + Type 2 diabetes taking the DPP-4 inhibitors to match the 64 controls who were taking DPP-4 inhibitors. This result suggested to the researchers that DPP-4 inhibitors were in some way reducing the incidence of Parkinson’s.
While the researcher were again caution about concluding too much from this result, they finished by suggesting that future studies with a larger sample sizes and longer follow-up period should be conducted to confirm this observation.
Now this result by itself is pretty weak due to the low numbers. But it is supported by other research that has been conducted on DPP-4, which agrees that there could be something interesting going on here (Click here to read a previous SoPD post about DPP-4 inhibitors).
Thus, I am left wondering why – if people with diabetes have been taking medication that could potentially reduce the risk of Parkinson’s – would diabetes have a negative outcome on this neurodegenerative condition.
Bydureon pen containing Exenatide. Source: Businesswire
And this is equally bizarre when you consider the positive results of the Exenatide/Bydureon clinical trials on Parkinson’s (Click here and here to learn more about this). Those clinical trials involved a diabetes drug that is being repurposed for Parkinson’s. The results suggest that the drugs is having a positive impact on the motor features of Parkinson’s…. so why would diabetes be associated with poorer outcome in motor scores in this new study looking at the effect of diabetes on Parkinson’s (reviewed above).
It begs that the controversial question: Have the cohorts of diabetics with Parkinson’s been cases of poorly medicated diabetes?
As you can probably guess, the situation here is as clear as mud.
A great deal of more research is required.
What does it all mean?
Previous research has suggested that some people with Parkinson’s have glucose intolerance issues, but it is unclear if this is a cause or a consequence of Parkinson’s itself. The incidence of this glucose intolerance, however, has led researchers to ask if there is any association between Parkinson’s and the metabolic condition of diabetes.
Large epidemiological studies can not seem to agree on whether there is or is not an association between Parkinson’s and diabetes, but previous clinical studies suggest that having diabetes can negatively affect the course of Parkinson’s. While this information may be upsetting for some readers, it must be appreciated that not all diabetics go on to develop Parkinson’s (only a small fraction), and not all diabetics with Parkinson’s have worse outcomes than non-diabetic people with Parkinson’s. At present it is not possible to determine the progression of Parkinson’s for anyone (diabetic or not).
Future clinical trials focused on the repurposing of diabetes-based drugs for Parkinson’s (such as the Exenatide studies) should attempt to determine if the glucose intolerant participants have more or less of a response to the drug being tested. In addition, the identification of the glucose intolerant/diabetic individuals within a future clinical trial cohort should be made before assessing the efficacy of any drugs in future clinical trials to determine whether having this issues with glucose could affect the efficacy of the drug being tested. Such information could be critical for future clinical usage.
The banner for todays post was sourced from Healthline.

















One sentence stood out for me:
“At present it is not possible to determine the progression of Parkinson’s for anyone (diabetic or not).”
I wish someone had told me this when I was first diagnosed. I kept feeling like doctors knew things they didn’t want to tell me because they didn’t want to be discouraging. They seemed so reluctant to say anything about prognosis or progression and I was incredulous that after all these years they couldn’t or wouldn’t say more. Sorry about the rant but I do appreciate your helpful post and am amazed at your depth of knowledge. Thanks!
LikeLike
Hi Diana,
When folks are diagnosed with a medical condition, they immediately have lots of questions and they simply assume that the physician has all the answers. The problem (particularly with Parkinson’s) is that everyone is different – especially when it comes to prognosis or progression – and we simply have no way of predicting outcome. Your suspicion about your doctors is not a unique situation – I have heard a lot of people say similar things and voice frustration at the circumstance.
With each new finding, we are getting closer to being able to provide that kind of information, but such knowledge may not be welcomed by the receiver whose life has just been changed by the diagnosis a particular medical condition. I can foresee some difficult ethical dilemmas coming with all this new technology. But hopefully by the time we get to that point, we will also have semi-curative treatments that can slow/halt the progression of Parkinson’s.
I hope this helps.
Kind regards,
Simon
LikeLike
Lots of the same with my health I need to get some more info on this but I think I have a good feeling about the things I have been finding
LikeLike
P.s. no need to respond – it made me feel better writing but i know it’s off topic
LikeLike
Happy to respond (sorry for the delay) – not off topic at all
LikeLike
I read somewhere that the placebo response in Diabetics is poor by comparison to the response of someone with Parkinson’s.
Is there scope to measure the placebo response because of the expected response differential in these groups
.There are three potential that might provide insight into placebo response or mechanism
Groups
1Parkinson’s 2 Parkinson’s and Diabetic and? 3. Diabetic.Also are there any stats on diabetes acquired before Parkinson’s and diabetic diagnosis after Parkinson’s and associated progression outcomes
I have Parkinson’s was young onset 14 yrs ago at 44yrs now and very well,I was in the clinical trial GDNF Bristol My father got type 2 diabetes before Parkinson’s
LikeLike