|
Recently researchers have proposed an interesting idea for why Parkinson’s is a distinctly human condition: There are parts of our brains that have not kept up with evolution, and as we live longer those areas become strained which ultimately results in the features of Parkinson’s. It’s a really interesting idea – one which could have major implications. In today’s post, we will review the new proposal and consider how we could use it in our approach to therapeutic interventions.
|
 2020 Tesla Roadster. Source: Motortrend
2020 Tesla Roadster. Source: Motortrend
By nature and design, I am not a car person.
If I can actually fit in the car (I am rather tall) and it gets me from A to B, it’s a great car. I don’t really care what it looks like, because I usually look ridiculous in the more sporty versions (my knees up around my ears…). As long as it gets from A to B, I’m happy.
Having said that, I do appreciate the technological advancements that are being made by companies like Tesla (I mean seriously, their Roadster – pictured above – is an electric car that does 0-60 mph in 1.9-seconds, quarter-mile in less than 9-second, a 250-plus-mph top speed, and an all-electric range of 620-mile! All of those statistics are incredible!).
It is amazing the evolutionary process that automobiles have gone through.
 The first petrol engine-propelled car invented by Karl Benz. Source: Oxfordsurfaces
The first petrol engine-propelled car invented by Karl Benz. Source: Oxfordsurfaces
Every aspect of these vehicles has changed over time. From the wheels to the engine and from petrol to electric based cars, each component has been adapted across the decades to keep up with the needs of its environment.
Researchers are now wondering if the same can be said for our brains. And just recently some scientists have questioned whether some evolutionary design faults could explain why humans develop Parkinson’s.
What?!? What do you mean?
Recently this paper was published in the journal Movement Disorders:
 Title: Parkinson’s disease: Is it a consequence of human brain evolution?
Title: Parkinson’s disease: Is it a consequence of human brain evolution?
Authors: Diederich NJ, James Surmeier D, Uchihara T, Grillner S, Goetz CG.
Journal: Mov Disord. 2019 Feb 13. [Epub ahead of print]
PMID: 30759321 (This report is OPEN ACCESS if you would like to read it)
In this report, the researchers began by asking “why should Parkinson’s be an exclusively human disease“?
The researchers approached this question from an evolutionary stand point, firstly noted that humans have a larger brain in relation to the mass of their bodies compared to all of our fellow primates. As you can see in the graph below, when it come to brain mass vs body mass, we humans are an outlier on the brain side of things:
 Each circle represents a type of primate. Source: Wiley
Each circle represents a type of primate. Source: Wiley
And it’s not just primates. Human brain-to-body mass ratio is high across all species in the animal kingdom:
 I like the addition of the Tyrannosaurus. Source: Twitter
I like the addition of the Tyrannosaurus. Source: Twitter
But the investigators pointed out that this increase in brain mass has not been equally distributed across all of the various regions of the human brain. Some regions (such as the cerebral cortex) have grown significantly as humans have evolved, while other regions such as the midbrain (which houses the dopamine neurons – which are so severely affected in Parkinson’s) has not experienced the same levels of tremendous expansion.
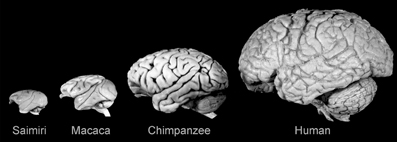 Note the change in brain size across primates. Source: Frontiers
Note the change in brain size across primates. Source: Frontiers
What is the cerebral cortex?
The cerebral cortex is the outer layer of the brain. Sometimes called the neocortex, it is the wrinkled, walnut-looking overlying surface of the brain. In the image below, the cerebral cortex is everything in pink:
Source: Slideplayer
And in the image above, you can also see the much smaller midbrain – highlighted in blue. This is where the dopamine neurons live.
Remind me again, what are dopamine neurons and why are they important to Parkinson’s?
The loss of the dopamine producing neurons in a region of the midbrain called the substantia nigra, is one of the cardinal features of the Parkinsonian brain. The substantia nigra (or ‘substance dark’) region is visible (with the human eye) on postmortem sections of brain due to the production of a molecule called neuromelanin in the dopamine neurons. And as you can see in the image below, the Parkinsonian brain has less dark pigmented cells in the substantia nigra region of the midbrain.
 The dark pigmented dopamine neurons in the substantia nigra are reduced in the Parkinsonian brain (right). Source:Memorangapp
The dark pigmented dopamine neurons in the substantia nigra are reduced in the Parkinsonian brain (right). Source:Memorangapp
In evolutionary terms, the neocortex is the most recent part of our brains to develop, and it is where we do most of our planning and thinking.
 Source: Gottalightmyfire
Source: Gottalightmyfire
At the top of the spinal cord, there is a region that is sometimes referred to as the ‘reptilian brain’ as the portions making up this part of the brain have not expanded much across evolution. This part of our brains controls some of the most basic functions of our bodies, such as respiration, sleep, balance, and heart rate. The midbrain – where the dopamine neurons reside – is within this ‘reptilian’ domain.
In between the neocortex and the ‘reptilian brain’ is the limbic brain, which is a structure that developed between these two parts of the brain.
Ok so the researchers think that the cortex has expanded over evolution faster than the older parts of the brain, like the midbrain?
Exactly.
And you can see this when you look at the number of dopamine neurons (or TH-ir neurons – in the graph below) and the volume of cortex. Again humans are an outlier here in that we have more cortical volume than might be expected on the evolutionary trend (when compared to the number of dopamine neurons). Dopamine neurons have literally been left behind.
 Source: Wiley
Source: Wiley
But why is this a big deal? And what does it have to do with Parkinson’s?
Because larger brains require more energy. And if some parts of the brain (such as the cortex) are expanding faster than other areas (such as the midbrain), this may put a lot of extra pressure on cells in the midbrain that are communicating with these larger cortical areas – think: dopamine neurons.
Can you explain how dopamine neurons are connected to these areas?
Sure. The dopamine neurons in the substantia nigra produce the chemical dopamine, but they release most of it in a region called the striatum, which is some distance from the midbrain. The dopamine neurons project long branches (called axons) to the striatum where the form of connections with other cells and provide them with dopamine.
 A diagram illustrating the location of the substantia nigra dopamine neurons
A diagram illustrating the location of the substantia nigra dopamine neurons
in the human brain, and their fibre projections to the striatum . Source: NIH
But humans differ from other animals here because the dopamine neurons form more connections in the human brain and they do in other animals (such as mice).
A lot more!
“In humans, it is estimated that a single substantia nigra dopamine axon may form 1 to 2 million synapses in the striatum—an order of magnitude greater than the number in a rodent” – Source: Wiley
This increase in the number of connections puts a lot more pressure on dopamine neurons in humans.
In addition, while rodents only live for 2-3 years, humans have traditionally lived for 40-60 years – which has required dopamine neurons to work even harder. And more recently in our evolution, we have decided that living longer is a really good idea… (can you see where all of this is heading?) …which has put yet more pressure on a population of over worked neurons, like the dopamine neurons.
In humans, hyperbranched neurons (like dopamine neurons) may be more vulnerable to stress or wear & tear. And the researchers have proposed that as we live longer, any kind of vulnerablity may show itself in the form of Parkinson’s-like symptoms (loss of dopamine neurons, slowness of movement, rigidity, and a resting tremor).
 Source: Wiley
Source: Wiley
And it’s not just the dopamine neurons.
The researchers note that the total number of neurons in a region of the ‘reptilian brain’ called the locus coeruleus (which lies just below the midbrain) is substantially lower than expected in humans, and this region is also affected by Parkinson’s. This is where the serotonergic neurons reside, and these cells also have long branching axons that project up into the neocortex.
Do the researchers speculate on how the cells may be vulnerable?
Yes, they do. And this is important because it would point towards where we could be targetting therapies if the hypothesis is correct.
For example, these ‘over-worked’ cells have very high energy needs, and for this they derive internal power from mitochondria.
What are mitochondria?
Mitochondria are the power house of each cell. They provide the cell with energy, which helps to keep the lights on. Without them, the lights go out and the cell dies.

Mitochondria and their location in the cell. Source: NCBI
But here is the interesting thing to note regarding this aspect of the ‘evolution idea of Parkinson’s’: many of the early onset forms of Parkinson’s are associated with genetic variations in genes that are involved with normal mitochondrial functioning (such as PINK1 & PARKIN – Click here and here to read previous SoPD posts about this).
The researchers also point towards large changes in calcium concentrations in cells that are affected by Parkinson’s. And ‘over-worked’ cells could be very sensitive to any changes in the handling of calcium levels.
What does calcium have to do with Parkinson’s?
Everyone has grown up hearing that calcium is important for your bones, but above and beyond that calcium is critical for the normal functioning of your entire nervous system.
Few if any neural signals would get transmitted in the absense of calcium.
And nine years ago, researchers noticed something interesting – in the context of Parkinson’s – regarding calcium channel blockers that specifically target a specific type of calcium channel (called L-type calcium channels):
 Title: L-type calcium channel blockers and Parkinson disease in Denmark.
Title: L-type calcium channel blockers and Parkinson disease in Denmark.
Authors: Ritz B, Rhodes SL, Qian L, Schernhammer E, Olsen JH, Friis S.
Journal: Ann Neurol. 2010 May;67(5):600-6.
PMID: 20437557 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers collected the medical records of 1,931 people in Denmark who were diagnosed with Parkinson’s between 2001 and 2006. These records were age and sex matched to 9,651 records of healthy controls from the same register. After analysing all of the records, the investigators found that people prescribed with a type of medication called a L-type calcium channel blocker (dihydropyridines) were 27% less likely to develop Parkinson’s.
This finding supported a previous study that found a similar result (Click here to read more about that) and the same result was independently replicated a couple of years later (Click here to read that report).
And this finding was also supported by postmortem analysis of the Parkinsonian brain:

Title: Parkinson’s disease is associated with altered expression of CaV1 channels and calcium-binding proteins.
Authors: Hurley MJ, Brandon B, Gentleman SM, Dexter DT.
Journal: Brain. 2013 Jul;136(Pt 7):2077-97.
PMID: 23771339 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers looked at where in the human brain the L-type calcium channels were present and in what concentration. They used sections of postmortem brain to carry out this analysis, looking at both healthy specimens as well as those from people who passed away with Parkinson’s.
In the normal brains, the distribution of the L-type calcium channels and certain calcium-binding proteins was not associated with regions of the brain that are prone to the selective neurodegeneration that is seen in Parkinson’s. But the investigators observed a very different picture in the Parkinsonian brains.
Increased levels of L-type calcium channels and the calcium-binding proteins were found throughout the brains of people who passed away with Parkinson’s. Even in cases of early Parkinson’s (in people who passed away shortly after being diagnosed), increased levels of L-type calcium channels were even found in the cerebral cortex – a part of the brain largely unaffected in Parkinson’s.
These findings lead the researchers to conclude that “disturbed calcium homeostasis” may be “an early feature of Parkinson’s disease and not just a compensatory consequence to the neurodegenerative process”.
The folks proposing the ‘evolutionary theory’ of Parkinson’s (what they call the “telencephalization hypothesis”) suggest that calcium dysfunction and mitochondrial issues could impose a burden on populations of cells in subcortical regions of the human brain that have been “left behind” by evolution. And these ‘burdens’ could make them vulnerable. Any kind of stress (environmental, etc) could be enough to cause these overworked cells to die and hey presto: Parkinson’s.
Interesting, but how could this new ‘telen…cepha…lization hypothesis’ of Parkinson’s influence our approach to treating the condition (as you suggested in the intro)?
Good question.
The researchers proposing the ‘telencephalization hypothesis’ of Parkinson’s suggest that a better understanding of “axonal biology, synaptic function in neuromodulatory networks, and neuronal bioenergetics” would enable better therapies for the condition.
The good news here is that we are already clinically testing therapies targetting calcium and mitochondrial pathways.
What do you mean?
One of the big clinical trials a lot of people in the Parkinson’s research community are watching this year is the STEADY-PD III study.
 Source: STEADY-PD III
Source: STEADY-PD III
STEADY-PD III is a clinical trial that is investigating the utility of the calcium channel blocker ‘Isradipine’ (tradenames DynaCirc, Prescal) for Parkinson’s.
 Isradipine. Source: Dailymed
Isradipine. Source: Dailymed
There are 3 classes of calcium channel blocker according to their chemical structure:
- Benzothiazepines
- Phenylalkylamines
- Dihydropyridines
Isradipine is a calcium channel blocker of the dihydropyridine class. It is prescribed for the treatment of high blood pressure in order to reduce the risk of stroke and heart attack. Prof Frank Church over at the ‘Journey with Parkinson’s’ blog has a great page on isradipine (Click here to read that post).
The double blind, Phase III STEADY-PD clinical trial has been conducted at 56 research centres across the US & Canada, enrolling over 300 people with newly diagnosed Parkinson’s to take either isradipine or a placebo treatment for 36 months (participants are randomly assigned to one of the two groups – click here to read more about the clinical study).
The results of the trial are going to be announced in mid 2019 – and yes, you can expect a full report from the SoPD!
In addition to the STEADY-PD/Isradipine study, there is also the recently initiated UP study (UDCA in Parkinson’s), which is a gallstone treatment that has been found to improve mitochondrial function (Click here to read a very recent SoPD post discussing that study).
So what does it all mean?
Here on the SoPD website, we have previously discussed research suggesting an evolutionary advantage to Parkinson’s.
That is, there have been several studies published that suggest some of the young-onset forms of Parkinson’s may have resulted from genetic variations which initially inferred advantages at a young age, but went on to become disadvantages to their carriers at a later age of life (Click here to read that post). In today’s post we have discussed a slightly broader evolutionary concept.
Researchers have recently proposed a nice theory of Parkinson’s – based on the evolutionary expansion of the human brain – in which they propose some regions of the brain have been left behind by evolution, which has put an added burden on certain populations of neurons in those regions. And some of those populations of cells are involved with Parkinson’s.
This is an interesting idea which could have major implications for our current theories regarding Parkinson’s. For example, where does this hypothesis leave alpha synuclein – the protein that clusters together in Parkinson’s. Rather than being a potential causative agent being passed from cell to cell, could it be that the aggregation of this protein is simply a sign of an ‘over-worked’ neuron that has become dysfunctional and having trouble disposing of waste?
I really like this new theory, particularly as up coming clinical trial results may provide further insights. Needless to say, I will be looking for the STEADY-PD results with great interest.
The banner for today’s post was sourced from Imperial


Simon, as usual, nice job describing the PD story, and a very intriguing hypothesis proposed here! Your explanation was clear with superb visuals supporting the story. And I totally agree that many of us are looking forward to the STEADY-PD results. Best wishes my friend, Frank
LikeLike
Hi Frank,
Glad you liked the post – I rather like this idea. One of those ‘kind of obvious’ ideas when someone else points it out. Fingers crossed for STEADY-PD!
Kind regards,
Simon
LikeLiked by 1 person
Shortly after I became aware of isradipine I was able to get my doctor to prescribe it for high blood pressure. One of the few advantages of having Parkinson’s and high blood pressure. It has been three years now. Hope the study is good news.
LikeLike
Hi Len,
Thanks for your comment. Fingers crossed indeed. We should know the results of the study soon.
Kind regards,
Simon
LikeLike
thank you for translating the science into a form that is (almost!) intelligible to the educated layman. Also i am very impressed with the presentation as a presentation, clear, accessible.
Mac Greene
LikeLike
Hi Mac,
Thanks for your message and kind words – glad you like the website. Please let me know if there are any particular topics you would like discussed.
Kind regards,
Simon
PS I like that attitude: “Birds still sing while I live with Parkinson’s”!
LikeLike
Hi Simon
Its really good to be looking at the problem from different angles. This model really chimed for me. it seems to match up with the lived experience more closely than other approaches.
thanks
Eirwen
LikeLike
Hi Eirwen,
I’m glad you like this idea – I really like it. It’s one of the few theories I am comfortable with (I’m not really a ‘prion hypothesis’ supporter when thinking of Parkinson’s. MSA maybe, but I’m not sure about PD). This evolution idea has some logic to it though. We’ll see where it takes us.
Kind regards,
Simon
LikeLike