|
An important aspect of developing new potentially ‘curative’ treatments for Parkinson’s is our ability to accurately test and evaluate them. Our current methods of assessing Parkinson’s are basic at best (UPDRS and brain imaging), and if we do not improve our ability to measure Parkinson’s, many of those novel treatments will fail the clinical trial process and forever remain just “potentially” curative. The ideal method of monitoring Parkinson’s would be a device that requires little effort from the individual being monitored, is completely non-intrusive in their daily living, and is continually collecting information. In today’s post, we will explore the potential of the Ōura ring.
|
 Harry’s first appearance on the SoPD. Source: Bild
Harry’s first appearance on the SoPD. Source: Bild
Prince Harry has one and I want it.
A Megan?
No.
A smart, ginger beard?
No.
What then?
An Ōura ring.
What is an Ōura ring?
Only the best interesting thing to come out of Finland since… um… hang on… give me a second… to google search… for… something… Finnish. Oh yeah: Nokia mobile phones, the Linux operating system, and person-to-person text messaging (Radiolinja, 1993).
Very techinically minded those Finnish folk!
And the Ōura ring is an EXTREMELY clever piece of technology that simply sits on your finger.
 Source: Soukie
Source: Soukie
But what does the Ōura ring do?
The Ōura ring can measure various signals from your body using three types of sensors:
- Infrared LEDs
- 3D accelerometer and gyroscpe
- NTC body temperature sensor
The ring automatically connects (via Bluetooth) and transfers data to a mobile device (via the dedicated Ōura App):
 Source: Gadfit
Source: Gadfit
The three sensors allow the Ōura ring to measure:
- Interbeat interval of the heart
- Pulse amplitude variation (related to blood pressure variation)
- ECG level resting heart rate
- Heart rate variability
- Respiratory rate
- Movements, intensity of physical activity
- Body temperature deviation
But even better than that (as the image above indicates), this ring allows you to measure your sleep patterns – the assessment of which I have recently become rather obsessed with.
Why have you become obsessed with sleep?
Because a.) I don’t get enough of it, and b.) I want us to better assess and monitor some of the clinical features of neurological conditions, and at first glance sleep seemed like an easy thing to measure.
How is sleep affected in Parkinson’s?
Problems with sleep are some of the most common non-motor features of Parkinson’s, and many studies have demonstrated this.
A good example is the PRIAMO (PaRkinson And non Motor symptOms) study. It was an epidemiology study which aimed to assess the prevalence and incidence of non-motor features of Parkinson’s. It was a longitudinal 24 month observational study conducted by 59 Neurology Centres across Italy to establish the incidence of non-motor features in Parkinson’s. The study involved 1307 people with Parkinson’s.

Title: The PRIAMO study: A multicenter assessment of nonmotor symptoms and their impact on quality of life in Parkinson’s disease.
Authors: Barone P, Antonini A, Colosimo C, Marconi R, Morgante L, Avarello TP, Bottacchi E, Cannas A, Ceravolo G, Ceravolo R, Cicarelli G, Gaglio RM, Giglia RM, Iemolo F, Manfredi M, Meco G, Nicoletti A, Pederzoli M, Petrone A, Pisani A, Pontieri FE, Quatrale R, Ramat S, Scala R, Volpe G, Zappulla S, Bentivoglio AR, Stocchi F, Trianni G, Dotto PD; PRIAMO study group.
Journal: Mov Disord. 2009 Aug 15;24(11):1641-9.
PMID: 19514014
The PRIAMO study found that 98.6% of the participants reported the presence of non-motor features, and one of the most common was sleep problems – occurring in 64.1% of cases.
And these sleep related issues could be further broken down into:
- REM sleep behaviour disorder (29.6% of cases)
- Insomnia (36.8%)
- Excessive day time sleepiness (21.2%)
- Restless legs (15.2%)
These results have been replicated numerous times. In fact, the incidence of sleep problems in Parkinson’s is generally stated as occurring in 40% to 90% of cases (Click here for a good review on the topic).
What happens in the brain in Parkinson’s that causes sleep problems?
As you will be aware, sleep is an unconscious state that the body goes into when we lie down during the night. It is characterised by immobility and reduced responsiveness. There are two broad phases of sleep:
- Rapid eye movement (REM) sleep
- Non-rapid eye movement (NREM) sleep.
We pass through these phases in a wave-like cycles as we sleep:
 Stages of sleep. Source: Wikipedia
Stages of sleep. Source: Wikipedia
In addition, there are different stages that make up these cycles (stage 1-4, on the left hand side of the image above), which we pass through on our way down to stage 4 (or NREM sleep) and back.
These stages exhibit different patterns of brain activity:
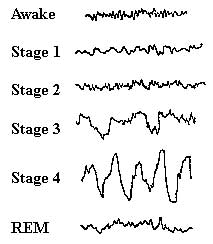 Brain activity during each stage of sleep. Source: Homesteadschools
Brain activity during each stage of sleep. Source: Homesteadschools
The brain is very active during REM sleep (this is the period during which we dream), whereas during NREM sleep the brain goes through periods of synchronised neuronal activity (resulting in the ‘high peak’ activity you can see in stage 4 of the image above).
In many cases of Parkinson’s, the pattern of sleep can be slightly different.
Parkinson’s is associated with increased sleep latency (that is, the length of time that it takes to fall sleep – more specifically, to move from full wakefulness to stage 1 in the image above). It is also associated with increased amounts of stage I sleep and reduced levels of REM sleep:
 The % of sleep time spent in stages 1-3 of non-REM sleep & REM. Source: Scialert
The % of sleep time spent in stages 1-3 of non-REM sleep & REM. Source: Scialert
This abnormal pattern of sleep is multifactorial in origin. It can of course relate to the motor issues of Parkinson’s, such as stiffness. Nocturia (needing to urinate) and medication effects (for example, dopamine agonists) can also disrupt sleep.
The sleep issues can also stem from the cell loss associated with Parkinson’s.
It was once believed that the brain had a specific “sleep region” (in a central region called the hypothalamus). And working in opposition to this was a separate “wakefulness region” (in the brainstem). But recent research has demonstrated that this proposal is too simplistic. Now it appears that wakefulness is not centralised but regulated by a whole network of structures in the brainstem, hypothalamus and basal forebrain.
 The circuitry of sleep. Source: Howsleepworks
The circuitry of sleep. Source: Howsleepworks
Unfortunately, some of the areas of the brain stem associated with sleep are affected in Parkinson’s. This is particularly evident in the REM stage of sleep.
Normally during REM sleep, reduced levels of serotonin activity in the brain leads to immobility of the body, through a network of brainstem neurons including the locus subcoeruleus and magnocellularis nucleus. But in Parkinson’s, some of these regions suffer cell loss which results in the body losing its immobility during REM. And this is why some people with very early Parkinson’s will act out their dreams.
Acting out of dreams is a feature of REM sleep behaviour disorder – a common precursor to Parkinson’s.
Click here for a very good review on the structures of the brain involved in sleep and how they are affected by Parkinson’s.
How is sleep currently assessed in Parkinson’s?
The most commonly used method of assessing sleep in Parkinson’s is the Movement Disorder Society-sponsored Unified Parkinson’s Disease Rating Scale (MDS-UPDRS).
It has two separate items for sleep:
- Nighttime sleep-related problems (item 1.7) – ranging from 0 (not present) to 4 (severe) scores.
- Daytime sleepiness (item 1.8) – ranging from 0 (not present) to 4 (severe) scores.
And that’s it.
An exhaustive assessment of sleep?
I think not.
Other rating scales can and are being used. For example, the Epworth Sleepiness Scale (ESS) has been widely used but it is not specific to Parkinson’s. It is also a self-administered rating scale and measures only daytime somnolence (or sleepiness). Other rating scales include the Pittsburgh Sleep Quality Index, Stanford Sleepiness Scale, and Karolinska Sleepiness Scale. There is also the Parkinson’s Disease Sleep Scale – a 15-item measure of commonly reported symptoms associated with sleep disturbance in Parkinson’s.
So we are measuring sleep using just rating scales?
Basically: yes.
But that’s crazy.
Indeed.
Ask someone if they are sleeping well, and they will say “yeah, I guess” or “no“. They will not say “I generally spend 30% of my night in REM stage sleep and only 18% in stage 1“.
It would be nice in a clinical trial assessing a novel treatment for Parkinson’s to have a much richer set of data to determine if the treatment is having any impact of sleep quality (which might not necessarily be the focus of the clinical trial, but it could still teach us something new).
So why don’t we assess sleep better?
The gold standard for physiological measurements of sleep is polysomnography.
Polysomnography involves recording of your brain waves, the oxygen level in your blood, heart rate and breathing, as well as eye and leg movements during a period of sleep.
 Polysomnography. Source: Sleep-apnea-guide
Polysomnography. Source: Sleep-apnea-guide
As you may appreciate from the image above, polysomnography require very specialised equipment that is needs to be calibrated and maintained in dedicated sleep laboratories, which is all rather expensive. It gives the participant and the investigators are very rich data set of information that can be used for analysis, but it is an episodic method, conducted in an artitifical environment (not in the individuals home). What we require are methods that provide continual measures, without the intrusive nature of patches and wires, and all within in the natural home environment.
And here we come back to the Ōura ring.
But how good is the ring at measuring sleep?
Well, let’s have a look.
In 2017, a group of independent sleep researchers evaluated the Ōura ring and compared it directly to polysomnography:
 Title: The Sleep of the Ring: Comparison of the ŌURA Sleep Tracker Against Polysomnography.
Title: The Sleep of the Ring: Comparison of the ŌURA Sleep Tracker Against Polysomnography.
Authors: de Zambotti M, Rosas L, Colrain IM, Baker FC.
Journal: Behav Sleep Med. 2017 Mar 21:1-15.
PMID: 28323455 (This report is OPEN ACCESS if you would like to read it)
In this study, the researchers purchased the two of the first version of the Ōura ring (two different sizes: US 7 and 11) and recruited 41 healthy teenagers and young adults (13 females; average age was 17.2 ± 2.4 years). The participants were asked to sleep overnight in a polysomnography lab, wired up to the recording machine and wearing one of the Ōura rings.
The participants were allowed to select which finger they wore the ring on (21 had the ring on their index, 2 on their middle finger, 2 on their little finger, 11 on their ring finger, and 5 on their thumb). They wore the ring from the moment they entered the lab, until the left the next morning.
The analysis of sleep was broken down into smaller periods of 30 second epochs, and a participant state (wake, N1, N2, N3 and REM) was attributed to each epoch based on the polysomnography reading.
When the researchers looked at the results, they found that the Ōura ring had a 96% sensitivity to detect ‘sleep’ – meaning that 96% of the time the ring correctly suggested the participant was asleep, matching the polysomnography result. When the researchers looked deeper at the results, they found that the Ōura ring matched the polysomnography results “light sleep” (N1), “deep sleep” (N2 + N3), and REM sleep 65%, 51%, and 61% of the time, respectively.
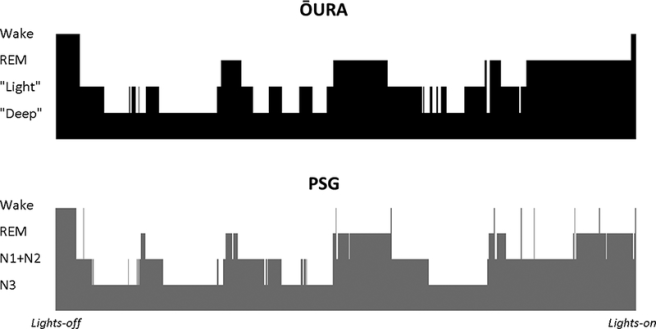 Similarities across sleep epochs. Source: PMC
Similarities across sleep epochs. Source: PMC
These numbers might not look very convincing, but more recently, these same researchers evaluated the Fitbit Charge 2™ under the same circumstances and found 96% accuracy for detecting sleep, 81% accuracy in detecting N1+N2 sleep (“light sleep”), 49% accuracy in detecting N3 sleep (“deep sleep”), and 74% accuracy in detecting REM sleep (Click here to read more about this).
Obviously these devices are not perfect, but I do like the non-intrusiveness of a ring.
It should be added that this first assessment of the Ōura ring was conducted on the first generation of the device, which was a proof of concept device.
Ist generation Ōura ring (left), shiny 2nd generation (right). Source: Engadget
The first generation only had 2-3 days of battery life, which has been significantly improved in the second generation ring (7-8 days battery life). And the battery only takes an hour or so to charge.
Charging the battery. Source: Strive
The main issue with the ring at present is the price (US$300+ at the time of writing), but hopefully that will come down over time.
And this is by no means an endorsement of the Ōura ring or company (I have had absolutely no communitcation with the company at the time of publishing this post). And Ōura is not the only tech firm in this area. Another company called MOTIV also has a tracking/smart ring.
The MOTIV ring is cheaper (approx. US$200 at the time of writing), but the battery does not appear to last as long and I can not find any peer-reviewed published research on the device (I would be happy to be corrected on this).
So what does it all mean?
As I have just said above (and below), this post is not a product endorsement.
The point of today’s post was simply to hightlight another non-intrusive means of monitoring oneself over time. But before you rush out and buy one of these clever bits of tech, I think it would be very interesting (for everyone involved) for one of these ring companies to make some of their rings available for use in a clinical evaluation of Parkinson’s.
One concern about this ring approach to monitoring Parkinson’s is what impact tremor (or dyskinesias) would have on the gyroscopic measures during day time periods. How accurate would the devices be in such cases? Even if worn on the non-tremor dominant hand. In addition, the research on the Ōura ring indicated differences in accuracy of the device between participants depending on which finger they wore the ring on – another cloud over the tech.
Perhaps, Ōura should supply us with some rings and we can have them clinically evaluated on some folks with Parkinson’s, and if they work well for a condition like PD one can assume they would be very useful for other less ‘shakey’ conditions like Alzheimer’s and multiple sclerosis.
I really like the non-intrusive nature of this ring method of monitoring Parkinson’s, particularly as while wearables like smart glasses (Click here to read a previous SoPD post about that topic) are removed before going to bed, one wears a ring continually. And in most cases (my wife will forgive me for saying so), we often forget that the ring is even there – an ideal characteristic of a wearable method of assessment (not such a good characteristic in a loving husband!).
Ōura, if you are interested – we would love to talk with you.
EDITOR’S NOTE – This is not a sponsored endorsement of the Oura ring product. The author of this post has not been asked by Oura or associated parties to produce this material. This post has been provided by the author solely for the purpose of sharing what he considers a really interesting idea. The author of this post has had no contact with the Oura company,…but if they would like to talk about doing some research on Parkinson’s, the author would be all ears.
The banner for today’s post was sourced from the5krunner




Is anyone pursuing evaluation of Parkinson’s disease progress by voice change (did your blog report 98% accuracy in diagnosis?) and retinal thinning (also emminantly measureable)? I think they must be measuring vocal changes in the PASADENA trial, judging by the daily tests.
LikeLike
Hi Susan,
Thanks for your interesting question. Yes, both of these areas are being followed up by multiple research groups. Very active areas of research.
Kind regards,
Simon
LikeLike
Hi Simon
If you get any offers for a research project, I’m up for trying it out. I bought myself a wrist base sensor but I think they need calibrating differently for PD. The analysis I got for sleep and exercise didn’t chime with my actual experience. Also the wristband disturbed my sleep (not helpful) catching on the bedclothes when I turn over, a ring would be brill!
I know from previous posts that you suggest the data collected might be more useful to clinicians than patients. In terms of managing ones lifestyle to maximise quality of life I think the feedback would be really valuable to patients.
Eirwen
LikeLike
Hi Eirwen,
Thanks for your comment. I would be interested in what you mean by “the analysis I got for sleep and exercise didn’t chime with my actual experience”. I use a Huawei wrist band and I use it mostly just for hours of sleep, heart rate, and steps. Most of the other measures I have found are inaccurate. I am talking with someone about the rings, but I suspect that they might not be great for PD due to the dyskinesias & tremor issues. We shall see what happens.
Kind regards,
Simon
LikeLike
This is good. Passive monitoring is key. I’m presently participating in a study which requires daily active monitoring. It’s downright demoralizing to see your performance change on thes tasks over time. I get anxiety from a neurologist exam wondering when the 1’s will turn to 2’s. Imagine doing that daily… bad for some of us. Others don’t mind so much.
LikeLike
Hi Double,
The psychological impact of self monitoring is a real worry. I think it will ultimately take a toll on anyone with a progressive condition. I am inclined to suggest blinding people completely and having them be monitored remotely. But I’m not sure that will actually solve the situation. It is a real tricky issue, and I’m not sure what to propose.
Kind regards,
Simon
LikeLike
I find that my fitbit heartrate is often confused and register very high rates which i put down to tremor (I check my pulse manually just to make sure …). That’s annoying but also suggests that these devices could be used to measure tremor itself.
LikeLiked by 1 person
Hi Kevin,
Thanks for your comment. Tremor is one of the hardest things to measure. You would think it would be very straightforward, but it varies from person to person and software has a very hard time discriminating tremor from other movements (outside of the clinical setting that is). If anyone has a good approach to real world measuring of it, I’d love to hear it.
Kind regards,
Simon
LikeLike
When my husband’s right hand is cold, it tremors. When he puts on good quality woollen gloves, the tremor stops. He has been diagnosed with vascular Parkinsonism. Why is this happening and so does he really have PD?
LikeLike