|
# # # # New technologies that can help us to better understand and track Parkinson’s over time has been a theme here on the SoPD. Such tools could create fantastic opportunities, particularly in the context of clinical trials evaluating new therapies, by providing comparable quantitative measures. Many of these efforts have focused on wearable technologies that require user input – mostly in the form of actually remembering to put the device on or to manually input data on a regular basis. More recently, however, some researchers have been investigating ‘invisibles’ rather than ‘wearables’, and the results have been rather remarkable. In today’s post, we will discuss how WI-FI technology is helping to better assess and measure Parkinson’s, and other medical conditions. # # # # |
 Source: Pandasecurity
Source: Pandasecurity
During the COVID19 pandemic, working from home has largely depended on availability of this strange thing called WI-FI. And as a result this strange thing called WI-FI has become a critical aspect of our daily lives.
The necessity of this strange thing called WI-FI becomes apparent when Zoom or Teams sessions are interrupted by a weak signal from this strange thing called WI-FI.
 Source: Highspeedinternet
Source: Highspeedinternet
But what exactly is this strange thing called WI-FI?
It is often said to be short for “Wireless Fidelity“, but it is not.
The generic term “WI-FI” was actually created by the marketing firm Interbrand (Source) because the wireless industry was looking for a more user-friendly name to refer to the not so user-friendly technology known as “IEEE 802.11b Direct Sequence” (Source).
WLAN (or Wireless Local Area Network) was an option, but it didn’t really have a catchy ring to it. In the end, WI-FI – a pun upon the word HI-FI – was selected and the rest is history.
WI-FI refers to the communication standard for the wireless network that has been around since the 1990s. It works as a Local Area Network for electronic devices to operate without using any types of cable or wiring.
 Source: Waveswifi
Source: Waveswifi
Most people use it for important tasks, like binge streaming ‘Squid Games’. But recently researchers have found other uses for this strange thing called WI-FI.
Like what?
This research review was published in 2020:
 Title: Deep Phenotyping of Parkinson’s Disease.
Title: Deep Phenotyping of Parkinson’s Disease.
Authors: Dorsey ER, Omberg L, Waddell E, Adams JL, Adams R, Ali MR, Amodeo K, Arky A, Augustine EF, Dinesh K, Hoque ME, Glidden AM, Jensen-Roberts S, Kabelac Z, Katabi D, Kieburtz K, Kinel DR, Little MA, Lizarraga KJ, Myers T, Riggare S, Rosero SZ, Saria S, Schifitto G, Schneider RB, Sharma G, Shoulson I, Stevenson EA, Tarolli CG, Luo J, McDermott MP.
Journal: J Parkinsons Dis. 2020;10(3):855-873.
PMID: 32444562 (This report is OPEN ACCESS if you would like to read it)
The report provides a good OPEN ACCESS overview for anyone interested in the current state of research of new techniques for the measuring and assessment of Parkinson’s. It provides a comprehensive picture of both the positive features and the limitations of some of the approaches being explored. It is recommended reading for those interested in the topic.
There are a lot of world-leading scientists in the list of authors of the review, but there is one name in the middle (bold and underlined) that I would particularly like to introduce you to.
This is Prof Dina Katabi – director of the MIT Wireless Center.
 Prof Dina Katabi. Source: Businessinsider
Prof Dina Katabi. Source: Businessinsider
Prof Katabi has taken a very different approach to measuring conditions like Parkinson’s. It involves no wearable devices… and it utilises that strange thing called WI-FI.
How can she measure Parkinson’s with WI-FI and no device???
WI-FI works on the simple principle of radio frequencies to send signals between devices.
 Source: Soundgirls
Source: Soundgirls
There are several frequency bands within the radio spectrum that are used for the WI-FI, allowing for information to be transferred very quickly.
Typically, a computer’s wireless adapter will translate data into a radio signal and transmit it via an internal antenna. Somewhere in the local environment a wireless router will receive that signal, decode it and share it with the internet using a wired Ethernet connection. That same router can take information from the internet and transmit it back to the computer by converting it into a radio signal.
But how is Prof Katabi using WI-FI to measure Parkinson’s?
When WI-FI transmitter sends radio signals out into the environment, they disperse in all directions. Solid objects like walls, deflect signals back in the direction of the transmitter and it can be picked up. The time between the signal being emitted and detected can give a measure of distance and position from the transmitter.
 Source: Csail.mit
Source: Csail.mit
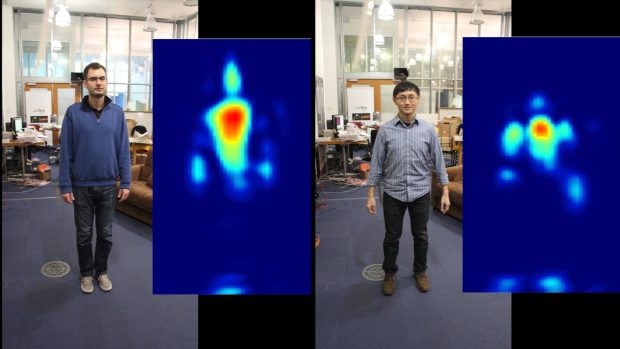
Solid objects in this case also includes us water-filled humans, and radio signals will bounce back off us and some will be received by the original transmitter.
 Source: PopularMechanics
Source: PopularMechanics
This approach allows Prof Katabi and her research team to simply place a WI-FI transmitter into a room, where it will emit radio signals. Some of these signals bounce back to the transmitter and can be received. That data is then fed into computers and rather impressive amounts of data can be analysed.
No wearable device required.
This video shows some of the data that can be collected and analysed:
And the details that can be measured are not limited to simply position of an object. This technology can also detect breathing and heart rate, which allows for some very “real world” applications:
And again, no wearable device or user input required.
Here is Prof Katabi explaining it herself:
If you are looking for a more in-depth presentation and explanation, watch this more recent video:
Fascinating. Has this ever been tested on Parkinson’s?
Yes.
In 2019, Prof Katabi and colleagues published this report:
 Title: Passive Monitoring at Home: A Pilot Study in Parkinson Disease.
Title: Passive Monitoring at Home: A Pilot Study in Parkinson Disease.
Authors: Kabelac Z, Tarolli CG, Snyder C, Feldman B, Glidden A, Hsu CY, Hristov R, Dorsey ER, Katabi D.
Journal: Digit Biomark. 2019 Apr 30;3(1):22-30.
PMID: 32095766 (This report is OPEN ACCESS if you would like to read it)
In this study, the researchers recruited 7 individuals with Parkinson’s and installed a WI-FI device in the bedroom of their homes for 8 weeks . In the image below, you can see the WI-FI device outlined in the yellow square in a bedroom setting:
 Source: PMC
Source: PMC
They wanted to determine if the technology could objectively measure both gait and time in bed, with the overall goal of generating “visualizations of home activity”. In total, they captured 353 days of monitoring over the 8 week experiment.
In the bird’s eye image below, the recorded data allowed for the visualisation of activity over a 3 hour period, with the path of movement superimposed on a schematic of the home (the WI-FI emitter is the green “Emerald device” located on the wall):
 Source: PMC
Source: PMC
The rare data is presented in the panel on the left, while the right panel provides a heat map of where time was spent.
This information can then be presented in terms of how much time was spent in different areas of the home. The researchers chose to visualise this in a circular display, which allowed for the 24 hour period to be laid out with different colours representing various activities. And each circle of colours – from the inner most to the outer most – represents a day (24 hours) of recording:
 Source: PMC
Source: PMC
A pretty picture, but it gets more interesting when one compares a particular activity between individuals, for example: time spent in bed. In the image below, you can see the daily bed activity of 6 individuals with Parkinson’s:
 Source: PMC
Source: PMC
In addition to these visualisations of the data, the researchers found that the gait speed determined by their WI-FI/Emerald device approach correlated very well with the clinical rating scores (using MDS-UPDRS total and Part III) that were collected at the start of the study. The 10-meter walk test – a clinic-based assessment of gait speed in Parkinson’s – has a reported minimal detectable change of approximately 0.22m/sec (Source), and this compared very well to the 0.07 m/sec that was recorded with the researcher’s Emerald device.
All of this data was collected from a WI-FI emitting box in the bedroom.
No wearable device required.
No user input.
And the researchers concluded their report by noting that their WI-FI/Emerald device could be very useful in observing the “natural history of diseases and detect real changes in function in clinical trials“.
Interesting, but why is this important?
A lot of what we use at the moment in the diagnosis and assessment of Parkinson’s is subjective qualitative data – describing qualities or characteristics often in a non-numeric fashion. And the subjective nature of this occurs with both the patient and clinician.
For example, how tired do you feel today? Your answer will be qualitative (very, not too bad, etc). Even if I ask you to give me a numerical measure of how tired you feel (on a scale of 1 – 10, ten being absolutely exhausted), your response is subjective (based solely on your view of things at this moment in time). Such subjective assessments can be prone to bias and change over time.
This is me when I am really tired (maybe, 8 on a scale of 1 to 10). Source: Theodysseyonline
A better way of assessing individuals with Parkinson’s over time would be continuous measurements, coming from technology that requires little or no effort from the person being monitored, and that provide numerical measures that can be compared across time and between individuals.
This may sound like a de-humanising approach, but it would hopefully provide objective, unbiased results.
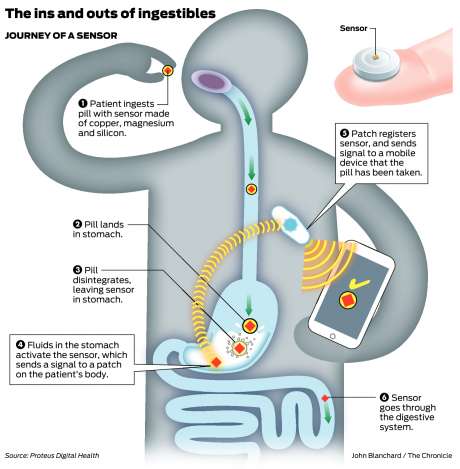
We have previously discussed new technology for assessing Parkinson’s on the SoPD – a good example being the use of smart pills to monitor what is happening in the gastrointestinal tract (Click here to read that post):
Smart pills. Source: sfchronicle
Smart pills require little effort from the individual taking the pill, beyond actually remembering to take their medication in the morning (which is a daily habit for many) and it can provide very useful, unbiased quantitative data that can be followed over time and compared with other individuals.
What else can the technology do?
The researchers have demonstrated that it can be used for monitoring self-administration of medication and adherence to treatment regimes, providing the opportunity for a reminder if the system does not detect that medication has been taken (Click here to read more about the research for this application).
Rather complex analysis of sleep is possible (Click here and here to read more on this research).
More recently, the technology has been tested for its utility in monitoring the long-term trajectories of respiratory and behavioral symptoms of elderly COVID-19 patients at home (Click here to read more about this research).
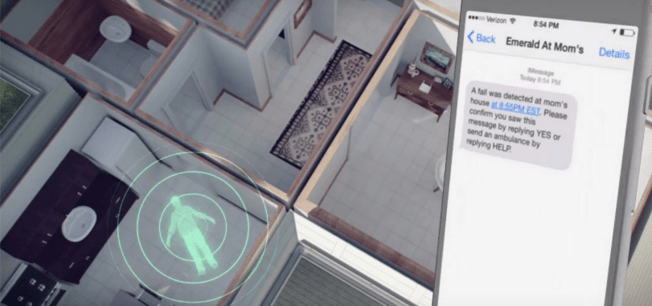
On a very basic level, this type of technology could be very useful in providing support to vulnerable communities (such as the elderly) who if they fall and are unable to get help, this WI-FI-based system could allow for more rapid alert and response options.
 Source: Robbreport
Source: Robbreport
There are lots of really exciting opportunities for this kind of technology, and this has led Prof Katabi to start a company Emerald Innovations.
But continuous monitoring sounds a bit ‘Big brother’ and is all that WI-FI exposure bad for you?
I hate to break this to you, but we as a population are already being continuously monitored.
If you have a cell phone or a bank card, your data is being continuously collected. Supermarkets, for example, are monitoring what you are buying and when. If you are reading this, then Google, Facebook (excuse me: META), and Netflix are probably constantly watching your online behaviour. It is very likely that the data already collected would tell us more about us than we know about ourselves.
In addition, if you are reading this, you are probably bathing in an environment saturated with radio frequencies. WI-FI is simply one of many (think of your TV, radio, cell phone, etc). I was shocked recently that I could pick up my home WI-FI network from inside a house several doors down our street. I doubt that one more WI-FI emitter in our lives would make much of a difference.
 Source: Toonpool
Source: Toonpool
All of that said, I would be a bit nervous about having a look at my daily patterns (I spend way too little time sleeping and way too much time in front of this laptop).
But I like this new technology because it provides useful real world data (as opposed to activities like finger tapping) and requires zero effort from the individual being monitored.
It could be really powerful in a clinical trial setting, collecting data in the background that may be very useful to determining if a treatment has had an effect.
So what does it all mean?
Here on the SoPD we have previously made a theme of posts exploring new technologies/approaches for monitoring and measuring Parkinson’s over time – from smart glasses (Click here to read that post) to smart rings (Click here to read that post) we have explored quite a few different approaches (Click here, here, here, here, here and here to read a few other examples). Such is the pressing need for better methods of monitoring Parkinson’s progression in clinical trials.
Many wearable technologies have thus far been rather intrusive approaches, requiring regular effort from the person being observed – which obviously brings an opportunity for bias to enter the equation – so here at the SoPD we have tried to focus on technologies that go largely unnoticed as they collect data.
The new WI-FI-based method discussed in today’s post may be the least physically intrusive one yet, as it requires nothing from the person being monitored. Yes, it may seem rather ‘big brother’-ish, but as you may have picked up, I rather like this approach and look forward to seeing how it develops and gets employed in future clinical trials.
And thanks to Pablo for bringing this technology to my attention.
 All of the material on this website is licensed under a
All of the material on this website is licensed under a
Creative Commons Attribution 4.0 International License
You can do whatever you like with it!
The banner for today’s post was sourced from safeum




2 thoughts on “From wearables to invisibles”