|
Self tracking/monitoring has become a popular habit for the general population with the introduction of products like Fitbit and Apple watch. It is particularly useful for groups like the Parkinson’s community though, who are tired of having just one hour per year of assessments with their neurologist. In today’s post, we will look at some new tracking/monitoring technologies that are being developed that could have important implications for not only how we assess Parkinson’s disease, but also for how we treat it. |
Homo deus. Source: RealClearLife
I have recently finished reading ‘Homo Deus‘ by Yuval Noah Harari – the excellent follow-up to his previous book ‘Sapiens‘ (which is an absolute MUST READ!). The more recent book provides an utterly fascinating explanation of how we have come to be where we will be in the future (if that makes any sense).
In the final few chapters, Harari discusses many of the technologies that are currently under development which will change the world we live in (with a lot of interesting and cautionary sections on artificial intelligence – the machines that will know vastly more about us than we know about ourselves).
Of particular interest in this part of the book was a section on the Google-Novartis smart lens.
What is the Google-Novartis smart lens?
In 2014, a company called Alcon, which is a wholly owned subsidiary of Novartis formed a collaboration with the Google offshoot Verily Life Sciences that would focus on developing smart lens.
The initial project is rather ambitious: develop and take to the clinic a glucose-sensing contact lens for people with diabetes. The idea has been particularly championed by Google founder Sergey Brin (a prominent figure within the Parkinson’s community with his significant contributions to Parkinson’s research each year).
People with diabetes have to keep pricking their finger over the course of a day in order to check the levels of insulin in their blood. A less laborious approach would be welcomed by the diabetic world (an estimated 415 million people living with diabetes in the world).
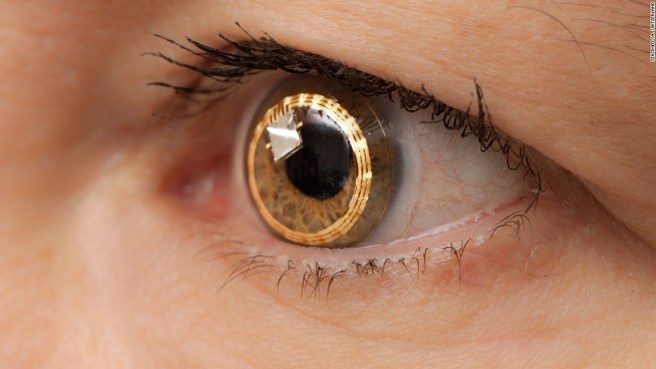
This is what the lens may eventually look like:
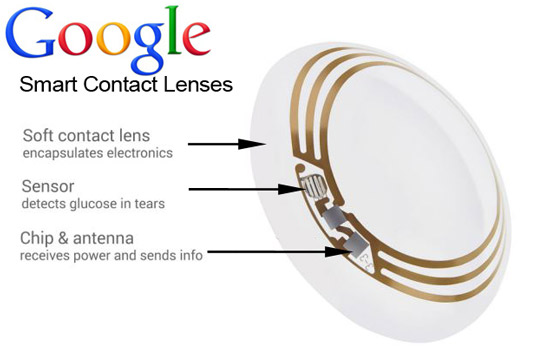
The system will include:
- A lens (obviously!).
- A sensor for detecting insulin levels in the lacrimal fluid (that solution passing over our eyes and making up our tears).
- A microchip and antenna for transmitting the results to a mobile device (e.g. a smart phone).
- A mobile device for tracking insulin levels over time and alerting the individual when more insulin is required.
The information collected on the mobile device will not only form a useful reminder system for the diabetic person, but will also serve as a means to tracking the course of the disease long term. This video may explain it all better than I can:
Sounds pretty science fiction/futuristic huh? If it works, it would be amazing!
But can you measure insulin levels in tear drops?
Apparently you can:

Title: Tear glucose levels in normal people and in diabetic patients
Authors: Sen DK, Sarin GS.
Journal: Br J Ophthalmol. 1980 Sep;64(9):693-5.
PMID: 7426593 (This article is OPEN ACCESS if you would like to read it)
In this study, the investigators recruited 50 normal people and 50 people with diabetes. They collected blood, urine and lacrimal fluid (tear) samples from all the subjects after overnight fasting and no diabetes treatments. The normal subjects glucose levels in the tears averaged 3.6 mg/100 ml and in the diabetic subjects it averaged 16.6 mg/100 ml. Similar to both blood and urine, lacrimal fluid glucose levels were significantly higher in diabetic patients than normal persons.
This study does raise cautionary findings though with regards to the accuracy of lacrimal fluid glucose levels: 4.6% of the diabetics fell into the normal range of glucose levels, while 5.8% of the normal persons were actually classified as diabetics!
This an other research has left a lot of people skeptical about the google lens idea, and the project has fallen behind schedule (Click here and here to read more about the delays). Many people worry that you can not measure insulin levels in the blood accurately enough for the readings to be used by diabetics to better control their condition. Variable or faulty readings are not desirable when one is injecting oneself with insulin.
In addition, there is serious competition in the area of monitoring insulin levels. A product from a company called Dexcom is one example:
The Dexcom system. Source: Nzmsdiabetes
Dexcom has developed an FDA approved patch that has a metal wire (sensor). The sensor is inserted just below the skin under the patch. The wire generates a small electrical signal in response to the amount of glucose that is present. Every 5 minutes, a signal is transmitted wirelessly to a dedicated receiver and/or compatible mobile device (e.g. smart phone or smart watch).
The Dexcom system. Source: Dexcom
The user can always be kept up to date with where his/her insulin levels are at any moment in time. The watch and mobile device (such as smart phone) can also have an alarm set up to let the wearer know when their insulin levels are getting too low.
So what dose all this have to do with Parkinson’s disease?
Well, what if such a monitoring system (the lens or the patch) could be adapted to monitor levels of Levodopa.
Can you measure Levodopa in tear solution?
Apparently it is possible:

Title: Catecholamine content of the lacrimal fluid of healthy people and glaucoma patients.
Authors: Zubareva TV, Kiseleva ZM.
Journal: Ophthalmologica. 1977;175(6):339-44.
PMID: 593659
In this study, the researchers recruited 86 people (aged between 35 and 65 years). 49 of these people had glaucoma and 16 people were diagnosed as ‘preglaucoma’. The remaining 21 individuals were healthy controls. The results of the study suggest that dopa and dopamine (as well as noradrenaline and adrenaline) can be determined from lacrimal fluid.
‘Dopa’ in this study was the naturally occurring type that is used to making dopamine. When one takes a tablet of Levodopa, the levels of levodopa go up as the medication circulates throughout the body.
By monitoring levels of Levodopa over time, one would have an objective means of tracking Parkinson’s disease (medication absorption, etc), and a means of alerting sufferers to when their Levodopa levels are getting low (increasing the risk of freezing or falls).
But how could this Levodopa monitoring information improve treatment though?
A information derived from the monitoring of levodopa levels in the lacrimal fluid or blood results could be communicated to a device like the Duopa system, which continuously pumps carbidopa and levodopa (by a pump) into the upper intestine.
The Duopa system. Source: 9and10news
So rather than simply having a continuous flow of Levodopa, the system could be tailored to the needs of the individual person. Such a continuous monitoring system connected to a device that could better maintain Levodopa levels in the blood would help to avoid the ‘roller-coaster’ (high and low) levels of Levodopa that are associated with taking this medication in a pill form.
The highs and lows of Levodopa pills over time
But what if I don’t have contact lenses and I’m also….scared of needles?
No problem.
There is a company called Proteus Digital Health who are developing pills and patches that can monitor what is happening both inside and outside your body.
The Proteus system. Source: Gestaltdesign
I am particularly impressed with this system.
Hypothetical situation: In the morning, you wake up and pop your first pills of the day. In amongst those pills is one covered in magnesium and copper. When the pills reach your stomach and come in contact with the digestive acids that reside there, most of the pills will be dissolved and release their therapeutic chemicals. The magnesium and copper covered pill, on the other hand, will start to generate energy (via chemical reaction). It will generate enough power, in fact, that the microchip inside the pill will be able to start communicating a unique time-stamped signal to the patch on your skin. The patch stores this number along with the exact time of pill ingestion and forwards that information to the users smartphone, from where the information can be shared with a doctor or relative who are given access to the information by the sufferer. Gone are the days when we ask “Is Dad OK today and has he taken his pills?” – now we can simply check on a smart phone.
Sounds a bit intrusive?
The amazing part of this system is that the patch also monitors your heart rate, steps, activity, rest and sleep quality:
The Proteus system. Source: Gestaltdesign
Never heard of this? Well, the ingestible sensor component secured FDA approval in July 2012, while the company’s sensor-laden patch got FDA clearance way back in 2010!
This short video may better explain the idea behind the Proteus approach:
So what does it all mean?
This post was stimulated by the reading of a book and various discussions with folks in the Parkinson’s community. It involves a bit of speculation about the future use of particular technologies for self tracking, but this is ultimately the way things are heading. We are moving away from periodic, irregular assessments towards an age of objective information.
And better methods of tracking Parkinson’s disease is a very necessary part of the future of researching and treating this condition. I and others within the research section of this community are very keen for more continuous and objective monitoring of folks with Parkinson’s disease (especially within the context of clinical trials – one UPDRS assessment every few months is soooo last century!).
Reading Harari’s book ‘Homo deus’, one could easily be scared of the future technological issues we will possibly face. But we can view every situation in two ways: as a problem or an opportunity. I prefer the latter…. though I have to admit to being weary of AI!
ADDENDUM: 31/8/2017
Taking this idea to an extreme: I have just read about a new form of tattoo that could one day be used to indicate biological activity within the body.
MIT and Harvard researchers have created colour-changing tattoos. By inserting biosensors into the ink that is used in tattoos, the researchers hope that the colour change of the tattoo will one day indicate changes in biological processes inside the body, such as insulin levels in diabetics (Click here to read more).
Question: Could the same approach be used to measure Levodopa levels in the body?
Just imagine a future world where checking the colour of dad’s tattoos in the afternoon could become a regular aspect of making sure he’s ok 🙂
The banner for today’s post was sourced from CNN








3 thoughts on “Self monitoring: there’s something in your eye”