|
At the end of each month, the Science of Parkinson’s writes a post which provides an overview of some of the major pieces of Parkinson’s-related research that were made available. In this post we review some of the research from February 2018. The post is divided into four parts based on the type of research (Basic biology, disease mechanism, clinical research, and other news). |
Seeing shadows: Punxsutawney Phil. Source: Wordonfire
In major world event news: On the 2nd February of 2018, Punxsutawney Phil – the groundhog who resides at Gobbler’s Knob of Punxsutawney, Pennsylvania – scurried out of his little hole and saw his shadow. This omen indicates that we have a long winter. Given how hard and bitter this particular winter has been, Americans naturally rejoiced.
On the 6th February, SpaceX successfully launched a Tesla sports car into space – see the video below for the highlights (and if you don’t have time to watch it all, at the very least jump forward to 3:45 and watch the two boosters land simultaneously – surely they didn’t plan for it to be that perfect!)
In other news, on the 1st February, the Centers for Disease Control and Prevention announced that it was dramatically downsizing its epidemic prevention activities in 39 out of 49 countries, due to concerns about funding.
And of course we had the 2018 Winter Olympics – where New Zealand came in 27th on the medals board:
Source: Madison365
In the world of Parkinson’s research, a great deal of new research and news was reported.
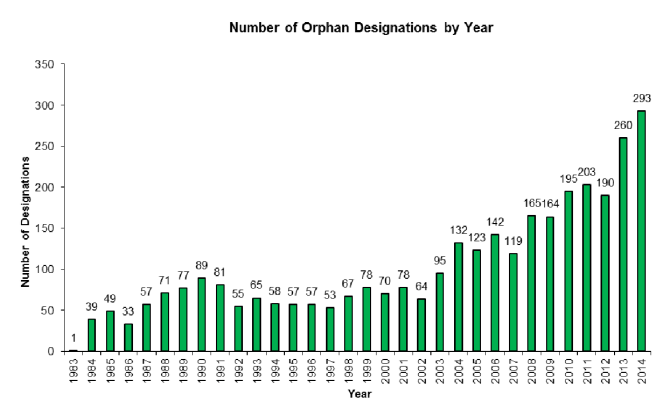
In February 2018, there were 698 research articles added to the Pubmed website with the tag word “Parkinson’s” attached (1577 for all of 2018 so far). In addition, there was a wave to news reports regarding various other bits of Parkinson’s research activity (clinical trials, etc).