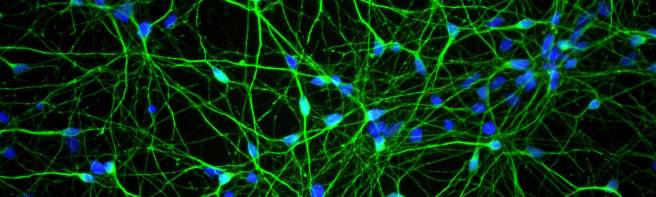
The classical clinical motor features of Parkinson’s disease (slowness of movement, rigidity and a resting tremor in one of the limbs) are associated with the loss 60% of the dopamine neurons in the midbrain.
What does this mean?
The midbrain is a structure at the top of the spinal cord – just as you enter the brain proper – and dopamine is a chemical that is produced in the brain. The dopamine neurons in the midbrain form connections with different areas of the brain, and are involved in many basic neurological functions, such as movement, motivation and addiction.

Sections of the human midbrain from a healthy individual (left) and a person who had Parkinson’s disease (right). The dopamine cells in the control subject can be seen on both sides of the brain with the eye because they produce a chemical (neuromelanin) that makes them black. These cells are noticeably absent in the Parkinsonian brain. Source: Springer
Not all midbrain dopamine neurons are affected in the same way in Parkinson’s disease though.
There are three basic groupings of dopamine neurons in the midbrain region:
- The substantia nigra pars compacta (or SNC)
- The ventral tegmental area (or VTA)
- The retrorubral fields (this is a very small group compared with the VTA and SNC)
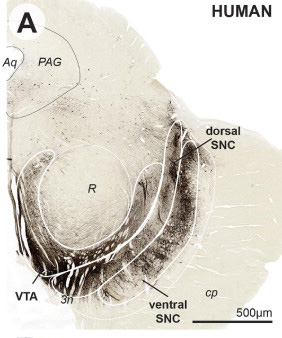
As the image above illustrates the SNC is divided into two regions – a dorsal layer and a ventral layer.
It has been acknowledged for a long time that the dopamine neurons in the SNC are more vulnerable in Parkinson’s disease than dopamine neurons in the VTA. We have no idea why this specific vulnerability exists. A great deal of attention has been focused on the SNC as a result.
The vulnerability of the SNC dopamine neurons when compared to the VTA, however, is not as clear as many researchers would believe.
In an interesting study published last year, some researchers from the University of Iowa, reviewed previous studies of postmortem analysis of the brains of people with Parkinson’s disease, in particular, focusing on the studies that had counted the number of dopamine neurons in the VTA and the SNC. The results were very interesting:

Title: The Vulnerable Ventral Tegmental Area in Parkinson’s Disease.
Authors: Alberico SL, Cassell MD, Narayanan NS.
Journal: Basal Ganglia. 2015 Aug 1;5(2-3):51-55.
PMID: 26251824
In essence, the study was very simple: the researchers compared the percentage of VTA and SNC dopamine neurons lost in Parkinson’s disease as determined by eight previous studies. They then conducted their own postmortem analysis and compared the results.
In their review of the previous studies, the researchers found that while the SNC was more vulnerable in Parkinson’s disease (approximately 70% of the dopamine neurons are lost), the VTA region still lost 50% of it’s dopamine neurons (see table below).
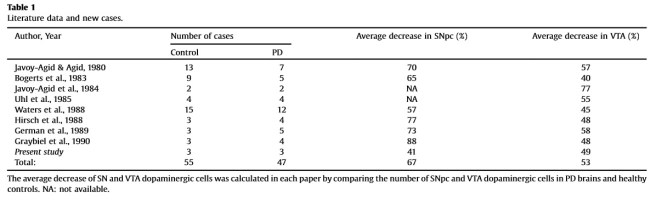
Curiously, the researcher’s own postmortem analysis found that the VTA was actually more vulnerable than the SNC. Their analysis, however, was based on only 3 brains. In addition, questions can be raised as to how the previous studies defined the borders of the SNC and VTA. Difference exist in those delineations of borders, which may impact on the number of dopamine neurons counted in each region.
The important message, however, is that the VTA is also badly affected in Parkinson’s disease. And given that the VTA is a region involved in mood and motivation, acknowledging its involvement in the disease will help to focus more research attention on to those areas of functioning in Parkinson’s.
 Wadlow (back row on the left). Source: Telegraph
Wadlow (back row on the left). Source: Telegraph Source: Businessinsider
Source: Businessinsider