|
It is one of the most frequent non-motor features of Parkinson’s and yet it is one of the least publicly discussed. The word ‘constipation’ is generally used to describe bowel movements that are infrequent or difficult to pass. The stool is often dry, lumpy and hard, and problematic to expel. Other symptoms can include abdominal pain, bloating, and the feeling that one has not completely passed the bowel movement. In today’s post we look at what can cause constipation, why it may be so common in Parkinson’s, discuss what can be done to alleviate it, and look at clinical trials focused on this issue.
|
Source: Hormonehelp
As many as 1 in 5 people say they have suffered from chronic (long-term) constipation at some point in their lives.
It results in more than 2.5 million hospital and physicians visits per year in the USA.
And Americans spend more than $700 million on treatments for it annually (Source).
More importantly, constipation is considered by many researchers to be a risk factor for developing Parkinson’s, as many people in the affected community claim to have experienced constipation for long periods prior to diagnosis.
Why this is, what is being done to research it, and what can be done about constipation in Parkinson’s is the topic of today’s post. But first, let’s start with the obvious question:
What is constipation?
In June 2016 – after 6 years of development, involving input from 117 experts (representing 23 countries) – The Rome IV diagnostic criteria for functional constipation was published. This is considered the definitive diagnostic criteria for constipation.
According to this new criteria, a diagnosis of constipation must include 2 or more of the following:
- Straining during more than 25% of defecations
- Lumpy or hard stools more than 25% of defecations
- Sensation of incomplete evacuation more than 25% of defecations
- Sensation of anorectal obstruction/blockage more than 25% of defecations
- Manual manoeuvres to facilitate more than 25% of defecations (e.g., digital evacuation, support of the pelvic floor)
- Fewer than 3 spontaneous bowel movements per week
In addition, loose stools are rarely present without the use of laxatives. And there is insufficient evidence for irritable bowel syndrome.
Yeah, that’s the technical definition, but what actually happens in my body when I’m constipated?
After the digestive process is started in your mouth and stomach, the broken down components of food is passed onto the intestines. The intestines are a long, continuous tube running from the stomach to the anus, which can be broken down into three regions: the small intestine, large intestine, and rectum.
Intestinal system. Source: Kidsbiology
The small intestine is approximately 20 feet long and about 2.5 cm (or an inch) in diameter. Its primary job is to absorb most of the nutrients from what we eat/drink.
Small intestine. Source: Asseintestinocervello
The large intestine (also called the colon) is about 5 feet long and about 8 cm (or 3 inches) in diameter. This is where water is absorbed and stool (or feces) is created and moved along .
Large intestine and rectum. Source: Insightstate
The rectum is where stool is stored until defecation. As stool enters the rectum, nerves there determine the urge to defecate.
Constipation is a condition of the large intestine and the rectum.
What is stool?
Most people probably think of stool as the semisolid remains of the food that has not been digested by the gastrointestinal system. But this is only a small part of what we defecate.
Stool usually is made up of mostly water (about 75%). Of the solid matter, about 30% consists of dead bacteria (which is the stuff that researchers analyse when they look at the ‘microbiome’ of the gut – click here to read more about this) and dead epithelial cells from the lining of the gut. Another 30% consists of indigestible food matter (such as cellulose). 10-20% is cholesterol and other fats, and another 10-20% is inorganic substances (think calcium phosphate and iron phosphate). Then there are also small amounts (2-3%) of protein that simply haven’t been absorbed in the digestive process.
So what goes wrong in constipation?
There are several different explanations.
“Gut transit time” refers to how long it takes for the food that enters your mouth to be excreted as stool from your anus. This will take anywhere between 50-70 hours. The longest part of this process is in the large intestine, where the average transit time is 40 hours (and there is significant difference between the sexes: 33 hours for men, 47 hours for women).
Gut transit time. Source: Thingsitellmymom
Constipation can result from a slowing of the gut transit time. This is referred to as ‘Slow transit constipation’, and it is characterised by the reduced motility of the large intestine, which could be caused by abnormalities of the enteric nerves (which may be playing a role in Parkinson’s – more on this below).
Another aspect of constipation is the absorption of water – too much absorption in the large intestine will result in harder stool, which will have trouble being transferred to the rectum. Medication can have an impact here.
And finally diet can be a major influencer of constipation. Diets low in fibre are at a higher risk of constipation (more on this below).
Source: Blogglophys
How common is constipation?
According to the National Institute of Diabetes and Digestive and Kidney Diseases, constipation is one of the most common digestive problems in the United States, affecting around 42 million Americans.
What causes constipation?
In the general population, there are many potential causes of constipation. For example:
1. Diet-related factors can leave you feeling constipated. These can include:
- Dairy products
- Too much junk food (high in fat and sugar)
- Lack of high-fiber foods (think fruits such as bananas and vegetables)
- Lack of water and other fluids
- Too much of certain fluids(think alcohol and caffeine)
2. Lack of exercise – simply moving around can help constipation (for example a regular walking regimen of 10 to 15 minutes several times a day can help).
3. Use of certain prescription and over-the-counter medications – these can include:
- Diuretics
- Narcotic painkillers
- Antacids (which neutralise the acid in your stomach to relieve indigestion and heartburn
- Iron supplements
- Anti-convulsants
- Certain antidepressants
- Blood pressure treatment
Constipation can also result from over use of the very medications taken to treat them — laxatives. Taking laxatives too often may cause your digestive system to become slack and dependent on them.
4. Certain medical conditions can also result in the increased frequency of constipation. These conditions can include:
Within the Parkinson’s community there are additional factors that can cause constipation, including certain medications (such as Artane (trihexiphenidyl) – a treatment that is often used to treat tremor).
Source: Macweld
How is constipation associated with Parkinson’s?
Constipation is very common in the Parkinson’s affected community.
One study from Pakistan, published earlier this year found that constipation was the most common non-motor symptom in a cohort of 80 people with Parkinson’s (occurring in 56% of cases):
Title: Frequency of non-motor symptoms in Parkinson’s disease presenting to tertiary care centre in Pakistan: an observational, cross-sectional study.
Authors: Mukhtar S, Imran R, Zaheer M, Tariq H.
Journal: BMJ Open. 2018 May 16;8(5):e019172
PMID: 29769252 (This report is OPEN ACCESS if you would like to read it)
In addition to the common occurrence of constipation within the Parkinson’s community, many studies have also shown that increased frequency and severity of constipation is associated with a higher risk of developing Parkinson’s (3 – 4 times higher in some studies – click here and here to read examples of research on this). Constipation is widely viewed as a common non-motor biomarker for Parkinson’s, with many in the PD community reporting episodes of constipation before diagnosis.
But why? How is the gut affected in Parkinson’s?
The simplest answer to this question is:
We simply do not know.
There are numerous studies indicating that the composition of the bacteria in the gut is different between people with Parkinson’s and unaffected individuals (Click here to read a previous post on this topic). The problem with much of this gut bacteria research, however, is the lack of consistency between the results.
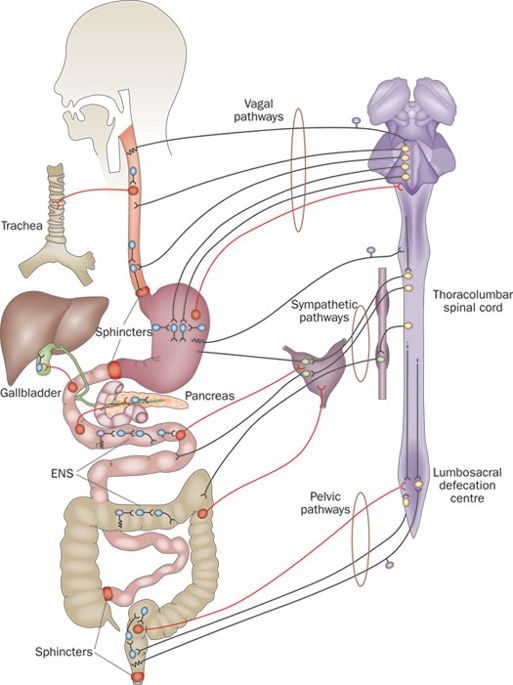
There has also previously been research suggesting that the Parkinson’s associated protein alpha synuclein could be clustering and aggregating in the nerve fibres surrounding the intestinal system of people with Parkinson’s (Click here, here and here to read about examples of this research). The nerves surrounding the gastrointestinal system are called the enteric nervous system:
Enteric nervous system. Source: Nature
It was proposed that the alpha synuclein building up in these nerves that help with gut motility, could be influencing the ability of the nerve cells to do their job – thus slowing or disrupting the gut transit.
But this research has also recently been questioned:
Title: Relation of Enteric α-Synuclein to Gastrointestinal Dysfunction in Patients With Parkinson’s Disease and in Neurologically Intact Subjects
Authors: Lee HJ, Jung KW, Chung SJ, Hong SM, Kim J, Lee JH, Hwang SW, Ryu HS, Kim MJ, Lee HS, Seo M, Park SH, Yang DH, Ye BD, Byeon JS, Choe J, Jung HY, Yang SK, Myung SJ.
Journal: J Neurogastroenterol Motil. 2018 Jul 30;24(3):469-478.
PMID: 29969861 (This report is OPEN ACCESS if you would like to read it)
In this study an endoscopic biopsy was performed on 35 people with Parkinson’s and 52 controls subjects.
What is an endoscopic biopsy?
Endoscopy is a procedure that allows doctors to visually examine the upper regions of your gastrointestinal tract. It involves a long, flexible tube (called an endoscope) with a light and camera at the end inserted in the patients mouth.
Source: Gfjules
This technique has been adapted slightly with the addition of a small set of scissors which allows for the grabbing and dissection of small biopsies. This is called an endoscopic biopsy.
Source: Murrasaca
The researchers in this study wanted to evaluate whether there was any association between gastrointestinal symptoms of Parkinson’s (like constipation) and levels of alpha synuclein in enteric nerves of the gut.
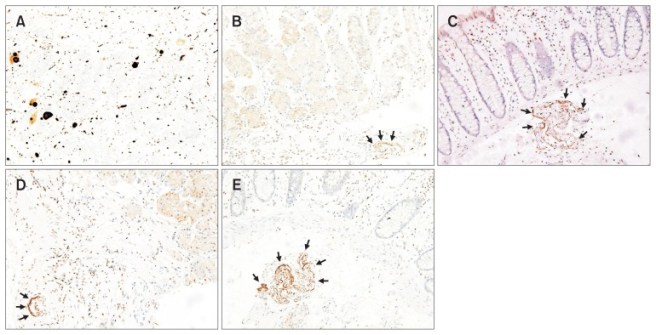
Of the 87 subjects in the study, 79 (or 90.8%) had one or more biopsy that was adequate for analysis. Alpha synuclein was found in 32 subjects (or 40.5% – see the image below).
Importantly though, the researchers found no difference in the presence of alpha synuclein in the enteric nerves when comparing the control and Parkinson’s biopsies. A similar percentage of people with alpha synuclein in the enteric nerves were found between the control and Parkinson’s biopsies (43.5% vs 36.4%, respectively).
Source: NCBI
In the image above, the researchers presented a positive control of alpha synuclein in Lewy bodies in panel A (staining of postmortem brain tissue from a person who passed away with PD). Panel B is alpha synuclein in gastric tissue from a 78-year-old man with an 11-year history of PD. Panel C is alpha synuclein in gastric tissue from a 55-year-old woman with a 2-year history of PD. Panel D is is alpha synuclein in gastric tissue from a 67-year-old woman as a control. And panel E is alpha synuclein in gastric tissue from an 80-year-old man as a control.
In addition, more people with Parkinson’s in the study with no alpha synuclein in the enteric nerves had self-reported constipation than those people with Parkinson’s who had high levels of alpha synuclein in the enteric nerves.
And this study is supported by another study which suggested that the presence of alpha synuclein in the enteric nerves is “a regular finding in adults with increasing age and may not be regarded as pathological correlate” (Click here to read more about this).
Thus, there are still questions as to whether the clustering of alpha synuclein is playing a role in gastrointestinal issues like constipation.
Ok, but how is constipation treated?
There are many different methods of trying to alleviate constipation – from medication to dietary. And before listing a few, I would just like to take this opportunity to remind you to discuss any change in your treatment regime with your doctor before embarking on any adventurous new anti-constipation approaches. Some of the methods listed below may impact on your current medication (Parkinson’s or otherwise). Please be safe.
Some of the approaches to treating constipation include:
1. Drinking more water – this one does help.
2. Eating more fiber, especially soluble, non-fermentable fiber.
3. Exercising more.
4. Taking senna–based treatments – this is a herbal laxative.
Died senna leaves. Source: Picclick
5. Over-the-counter or prescription laxatives – several are discussed below regarding clinical trials.
6. Eating brown rice, not white rice (with white rice the husk, bran, and germ have all been removed. This is where all the fiber and nutrients are. Brown rice can help to relief constipation as the husk, etc is still present).
7. Eating prunes or drinking prune juice (Click here to read more about this).
Prunes. Source: Gourmetfoodworld
8. Trying a low-FODMAP diet – the “Fermentable Oligo-, Di-, Mono-saccharides And Polyols” diet is better for sufferers of diarrhoea (Click here to read more about this), while the low-FODMAP diet can help with constipation (Click here to read more about this).
9. Trying magnesium citrate – it relaxes your bowels and pulls water into your intestines.
10. Avoiding dairy.
11. Avoiding alcohol (yes, I know).
12. Limiting chocolate intake (Again, yes I know, but chocolate is believed to slow foods movement through the bowel).
Chocolate – unfortunately popular stuff. Source: WallPapersCraft
13. Avoiding white bread and try gluten free.
14. Not peeling potatoes – leave the skin on because it has the best fiber benefits.
And what has been clinically tested for constipation in Parkinson’s?
Earlier this year a very good OPEN ACCESS review on this topic was published (Click here to read that review). I have used that review (and other sources) as the basis for the information provided here regarding clinical trial for constipation in Parkinson’s.
The obvious starting point is medical treatments, and the most well studied treatment for constipation in Parkinson’s are laxatives:
Laxatives
There have been many clinical trials of laxative treatments in Parkinson’s. These include:
Macrogol – A double-blind, randomised clinical study assessing the efficacy and safety of macrogol (7.3–21.9 g twice daily) in 57 people with Parkinson’s (27 in the treatment group and 28 in the placebo control group) found responder rates were significantly higher in the Macrogol-treated group than controls (Click here to read more about this study).
A second clinical study of Macrogol in 10 people with Parkinson’s (or multiple system atrophy) associated constipation reported that all of the treated participants reported improvements in stool consistency and marked improvements in their ease of defecation (Click here to read more about this study).
Lubiprostone – In a double-blind, randomised clinical study assessing the efficacy and safety of lubiprostone on 54 people with Parkinson’s associated constipation found a marked improvement reported by 16 of 25 (64.0%) subjects receiving drug vs 5 of 27 (18.5%) subjects receiving placebo (Click here to read more about this study).
Trends towards improvement have also been seen in clinical trials for other laxatives, including Tegaserod (Click here to read more about that study) and Relamorelin (Click here to read more about that study).
Botulinum neurotoxin A
In addition to laxatives, botulinum neurotoxin A (or “botox”) has also been assessed in clinical trials as a treatment for constipation in Parkinson’s (be warned dear reader that this segment may make some feel a bit uncomfortable – no illustrations will be provided here). Two clinical studies have assessed the efficacy of botox injections into the puborectal muscle – which is one of the muscles that comprise the pelvic floor and plays an important role in both fecal continence and defecation.
The first study involved 10 participants with Parkinson’s associated constipation and reported marked improvements in the puborectal muscle tone during straining (Click here to read more about this).
The second study used the same approach on 18 people with Parkinson’s and constipation. Improvement were noted in 10 of the participants at the 2 months evaluation, but given that the botox effect wears off after 3 months, the researchers suggested that ‘repeated injections could be necessary to maintain the clinical improvement’ (Click here to read more about this study).
Beyond medication, other clinical trials have been focused on:
Dietary – high fiber
Two clinical studies have looked at high fiber diets as a treatment for constipation in Parkinson’s:
1. Researchers from the Jiménez Díaz Foundation in Spain investigated the effects of a dietetic supplement (containing 375 mg wheat, 70 mg pectin, 2.5 mg dimethylpolyoxyhexane-900) in 19 people with Parkinson’s who had less than 2 weekly bowel movements. Two months after starting the treatment, the researchers reported that all of the participants were having more than ≥4 BMs/week and had higher bioavailability of Levodopa treatment in their blood (at 30 and 60 min after oral administration – Click here to read more about the results of this study).
2. Researchers from the University of Nebraska Medical Center (Omaha) treated three people with Parkinson’s with 5 mg psyllium (twice per day for 8 weeks) and compared them to four people with Parkinson’s who were treated with a placebo.
Psyllium. Source: Wikipedia
They reported that the psyllium-treated group experienced significant increases in the stool frequency (bowel movements increased from 2.9 to 5.8 per week) and stool weight (which increased from 400 g vs. 1300 g/week). The placebo group, however, did not demonstrate the same sorts of improvements (for example, 3.4 vs. 3.5 bowel movements per week – Click here to read more about the results of this study).
Dietary – probiotics
This has been a popular theme in the Parkinson’s community given recent research suggesting that the bacteria of the gut may be involved with Parkinson’s. Despite this, there has only been one peer-reviewed report of a clinical study focused solely on probiotics, which was conducted at the Parkinson’s institute (Milan). This study involved 40 people with Parkinson’s who were suffering from constipation who were treated for five weeks with a daily dose of 65 mL fermented milk drink which also contained a bacteria called Lactobacilus casei Shirota. Although the number of bowel movements did not improve, the participants did report experiencing less feelings of being bloated, less abdominal pain, and more complete emptyings (Click here to read more about the results of this study).
Dietary – fibers and probiotics
A study in 2016, again conducted by the Parkinson’s institute (Milan) recruited 120 people with Parkinson’s and constipation (2 bowel movements per week) and randomly assigned to either an active or placebo treatment group. The active treatment group recieved 125 ml of fermented milk each day (for 4 weeks), which also contained 7.8g fibre plus probiotic strains of bacteria. The placebo treated group recieved only daily doses of pasteurized fermented milk (125 grams) without prebiotics (for 4 weeks).
The results suggest an increase in the number of complete bowel movements per week (1.2 in the treatment group vs 0.1 in the placebo group). The active treatment group also exhibited an increase in stool consistency. And all of these results led to a higher percentage of participants in the active treatment group stating that they were ‘likely’ to continue the treatment after the study was completed (56.3% vs. 30.0% – Click here for more information regarding this clinical study and click here to read more about the results of this study).
A second clinical study investigating the combination of fibers and probiotics for constipation in Parkinson’s has been conducted, but this one had additional variables (such as increased water intake and fibre intake) which make the results difficult to interpret (Click here to read more about this).
Abdominal massaging
One clinical study has been conducted on abdominal massaging in 32 people with Parkinson’s associated constipation, but no significant difference was seen between the treatment and control groups (Click here to read more about this).
Deep Brain stimulation
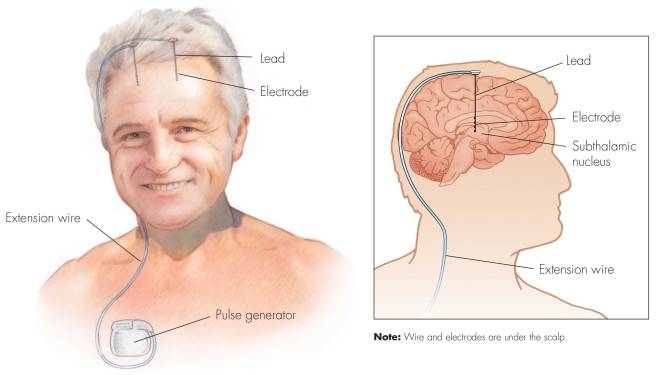
There has been a clinical study investigating whether deep brain stimulation can improve constipation in Parkinson’s. 20 people undergoing subthalamic nucleus deep brain stimulation surgery were recruited to the study, which involved monitoring of gastrointestinal symptoms before and 3 months after surgery. The results suggest that all gastrointestinal symptoms improved, the greatest improvement was observed in difficulty with defecation. Approximately 1/4 of the participants exhibited improvements in electrical recordings made of the gut motility (using electrogastrography – click here to read more about the results of this study).
Deep brain stimulation. Source: Ucdmc
Are there any clinical trials currently ongoing for constipation in Parkinson’s?
Yes there is.
In February of 2017, researchers published an article outlining how a compound (called Squalamine) derived from the spiny dogfish could completely suppress the toxic effect of the Parkinson’s associated protein alpha synuclein (Click here to read the SoPD post about that research).
The humble dogfish. Source: Discovery
And then in May (JUST 3 MONTHS LATER!!!), a biotech company called Enterin Inc. announced that they had just enrolled their first patient in the RASMET study: a Phase 1/2a randomised, controlled, multi-center clinical study evaluating a synthetic version of squalamine (called MSI-1436) in people with Parkinson’s (Click here for the press release).
Source: Onemednews
The study will enrol 50 patients over a 9-to-12-month period and given that MSI-1436 does not enter the brain, the researchers are hoping that it will have an impact on constipation. We are currently awaiting the results of this study.
Another Phase I clinical study, being run by Collaborative Medicinal Development Pty Limited, is a dose escalating study of Cu(II)ATSM to determine if this drug is safe for use in early idiopathic Parkinson’s.

Cu(II)ATSM (also known as diacetylbis(N(4)-methylthiosemicarbazonato) copper(II) – say that three times really fast!) is an orally administered drug that inhibits the activity of misfolded certain proteins (we have previously discussed this drug in the context of Amyotrophic lateral sclerosis (ALS; or motor neuron disease) – Click here to read that post). This multicenter study involves 6 months of open-label testing of 40 participants, and it is expected to be completed by the end of this year. We should have results in the 2019. A reduction in the levels of constipation is a secondary outcome for this study.
RaQualia Pharma Inc. is conducting a Phase I clinical trial of their drug RQ-00000010 (a serotonin 5-HT4 receptor agonist) as a treatment for constipation in Parkinson’s. This double blinded randomised placebo controlled trial will involve 75 participants taking the drug (or placebo) for 2 weeks. The study is supported by the Michael J Fox Foundation and should be finished early next year (2019 – Click here to learn more about this study). A reduction in the levels of constipation is also a secondary outcome for this study.
The University of Malaya is currently running a trial assessing the use of probiotics for constipation in Parkinson’s in a double blinded, randomised, placebo controlled clinical trial that will involve 60 participants. The subjects will be randomly given either the probiotic treatment or a placebo control. They will then be followed for 4 weeks during the treatment phase, with the number of stool movements per week being the primary outcome measure between the two conditions (Click here to learn more about this study).
And the New York Institute of Technology is currently conducting a clinical trial assessing the use of osteopathic manipulation on constipation in Parkinson’s. Osteopathy emphasises physical manipulation of muscle tissue and bones. This non-randomised study (involving 20 participants in a single group) will be seeking to determine if this approach decreases constipation symptoms over a 10 week period, but the researchers will also be analysing changes in the bacterial flora of the mouth and gut (Click here to learn more about this study).
What does it all mean?
Constipation is one of the most common non-motor feature associated with Parkinson’s, causing discomfort and agony for sufferers. In this post we have tried to provide an overview of not only what constipation is, but also on the research that has been done on it (and is currently being conducted) with regards to Parkinson’s.
It is surprising that more research isn’t being conducted on constipation given its frequency in both Parkinson’s and in the aging population. I can find no apparent reason for this, and only view it as a major opportunity for someone to grab the bull by the horns and run with it.
While those researchers conduct their investigations, however, there are tried and tested approaches for alleviating the burden of constipation that readers might like to try, but again: Please consult you doctor before attempting any change in your treatment regime.
EDITOR’S NOTE: The information provided by the SoPD website is for information and educational purposes only. Under no circumstances should it ever be considered medical or actionable advice. It is provided by research scientists, not medical practitioners. Any actions taken – based on what has been read on the website – are the sole responsibility of the reader. Any actions being contemplated by readers should firstly be discussed with a qualified healthcare professional who is aware of your medical history. While some of the information discussed in this post may cause concern, please speak with your medical physician before attempting any change in an existing treatment regime.
In addition, many of the companies mentioned in this post are publicly traded companies. That said, the material presented on this page should under no circumstances be considered financial advice. Any actions taken by the reader based on reading this material is the sole responsibility of the reader. None of the companies have requested that this material be produced, nor has the author had any contact with any of the companies or associated parties. This post has been produced for educational purposes only.
The banner for today’s post was sourced from Haber7





















There is no doubt that exercise is critical. Hard stools gradually became a problem as my other PD symptons manifested, but were useally manageable. I walk every day (the dog is fit and I get tired!). After 4 days of no walking during “the beast from the east” frost when I was scared to go out in case I slipped, I promptly had 2 weeks period when I had needed lots of laxatives. With better weather and walking things gradually improved.
Subsequently a great improvement came as a result of diet change. Breakfast of grananola with nuts, dried fruit, a spoonfull of husk, topped with half a banana made a great change. I now go almost every day, though sometimes still a strain.
LikeLike
Thanks for sharing Andy – there are useful bits of advice in your comment for everyone.
Kind regards,
Simon
LikeLike
Like Andy, I find that exercise and diet (I have a similar breakfast to Andy’s) are the best way to treat this problem, coupled with drinking more water.
Can I raise an unrelated (well, there is a loose connection!) issue. For 5 years, I have had no sense of smell. It went away completely. But suddenly, last weekend, I started to smell things again!! I wouldn’t say that I’ve regained it completely, but there has been a real change (for no discernible reason). Has anyone experienced this,or has any research been carried out in similar circumstances?
LikeLike
Hi Ken,
That is really interesting news regarding your sense of smell. I have had folks in the clinic suggest similar things (on rare occasions), so I can say that it is not unheard of. But I would be very interested to know what (if anything) has changed in your life over the last few weeks (hot, dry summer weather?).
Kind regards,
Simon
LikeLike
Have a look at this info/study on Mannitol and sense of smell (etc) https://youtu.be/9VVj7GeppNk
LikeLike
Excellent production as always! For my hubby who’s currently on Oramorph (Morphine sulfate) because of his acute pain after trapping the femoral nerve, it has meant trying to get ahead of impaction. So that means more water, lactulose (a brand of osmotic laxative) and a big gulp of good clean olive oil. So far it’s working….
LikeLike
Glad you found it interesting Lisa and thanks for sharing the useful bits of advice for folks to try.
Kind regards,
Simon
LikeLike
Simon,
Thanks for looking at this relatively unexplored symptom of PD. Constipation happens to have the biggest impact on my QOL. When drinking lots of water and taken macrogol haven’t worked, I find water enemas useful. (Note, many medics would not favour the chronic use of enemas. But, in my view, needs must.)
John
LikeLike
You’re welcome John – thanks for sharing.
Kind regards,
Simon
LikeLike
The prune juice reference in this column was most helpful. 4 oz prune juice, following a regular breakfast that includes fruit, whole grain, 4 oz coffee, 5 g mannitol in 12 oz water, and then a 15-20 minute walk, are working for me. The mannitol is part of CliniCrowd study about loss of smell. After several years of no smell at all, I am currently getting whiffs of things I had forgotten, but given spontaneous recovery of smell like that reported in other comments, am not sure 3 months of mannitol use can be credited. My advice to anyone trying mannitol is to be very sure to include plenty of liquid with every dose. After one experience with cramping after mannitol on fruit without a glass of water, I am conscientious about getting at least 12 oz. each time.
LikeLike
After a lifetime of horrible constipation problems for my husband and a myriad of expensive doctors never getting us anywhere, and now a diagnosis of PD, we’ve solved the constipation ourselves. We do an (almost) Paleo diet and fairly large doses of Vitamin C in the form of Ascorbic Acid.
LikeLike
Dear Sharon,
Thanks for your comment and the information shared. Nutritional laxatives such as ascorbic acid have become more popular, particularly with individuals who have constipation that is resistant to fiber. But (the usual cautionary note coming here) readers should consult their doctors regarding their current medication and dosing of vitamin C before initiating any changes to their treatment regimes.
Kind regards,
Simon
LikeLike