|
Here at the SoPD, we regularly talk about the ‘bad boy’ of Parkinson’s disease – a protein called Alpha Synuclein. Twenty years ago this year, genetic variations were identified in the alpha synuclein gene that increase one’s risk of developing Parkinson’s. In addition, alpha synuclein protein was found to be present in the Lewy bodies that are found in the brains of people with Parkinson’s. Subsequently, alpha synuclein has been widely considered to be the villain in this neurodegenerative condition and it has received a lot of attention from the Parkinson’s research community. But it is not the only protein that may be playing a role in Parkinson’s. Today’s post is all about TAU. |
Source: Wallpaperswide
I recently informed my wife that I was thinking of converting to Taoism.
She met this declaration with more of a smile than a look of shock. And I was expecting the latter, as shifting from apatheism to any form of religious belief is a bit of a leap you will appreciate.
When asked to explain myself, I suggested to her that I wanted to explore the mindfulness of what was being proposed by Lao Tzu (the supposed author of the Tao Te Ching – the founding document of Taoism).
This answer also drew a smile from her (no doubt she was thinking that Simon has done a bit of homework to make himself sound like he knows what he was talking about).
But I am genuinely curious about Taoism.
Most religions teach a philosophy and dogma which in effect defines a person. Taoism – which dates from the 4th century BCE – flips this concept on its head. It starts by teaching a single idea: The Tao (or “the way”) is indefinable. And then it follows up by suggesting that each person should discover the Tao on their own terms. Given that most people would prefer more concrete definitions in their own lives, I can appreciate that a lot of folks won’t go in for this approach.
Personally speaking, I quite like the idea that the Tao is the only principle and everything else is a just manifestation of it.
According to Taoism, salvation comes from just one source: Following the Tao.
Source: Wikipedia
Oh and don’t worry, I’m not going to force any more philosophical mumbo jumbo on you – Taoism is just an idea I am exploring as part of a terribly clichéd middle-life crisis I’m working my way through (my wife’s actual response to all of this was “why can’t you just be normal and go buy a motor bike or something?”).
My reason for sharing this, however, is that this introduction provides a convenient segway to what we are actually going to talk about in this post.
You see, some Parkinson’s researchers are thinking that salvation from neurodegenerative conditions like Parkinson’s will come from just one source: Following the TAU.
What is TAU?
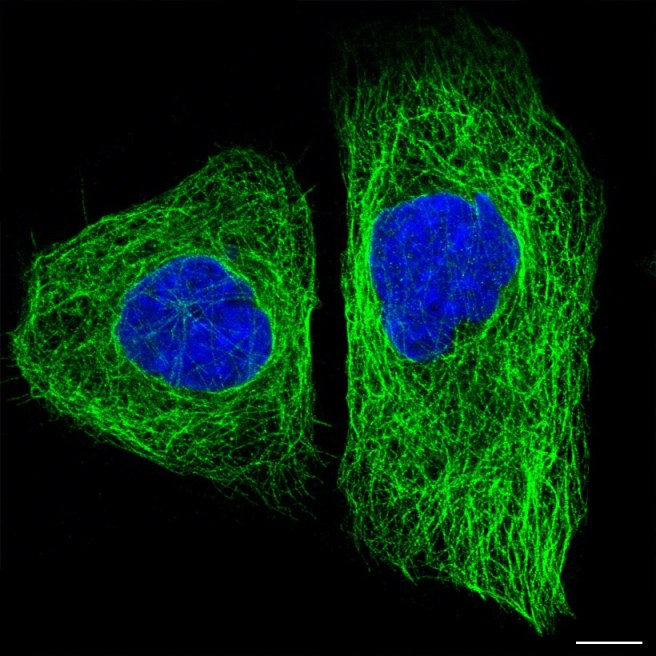
Tau protein (green) inside two cells. Source: The human protein atlas
Above is a special photo.
It is a fluorescent image of two cells that have been stained with two different dyes: one that labels the nucleus (in blue) and another that stains the microtubules (in green). Everything else in the cell (membrane and all) is left invisible.
What are microtubles?
Everyone who has done high school biology should be familiar with the nucleus of the cell – it is the command centre of the cell, where the DNA is kept. But microtubules may be a novelty for many readers.
Microtubles are the highways and byways inside a cell. They are structures inside of cells that are involved with both cellular and intracellular transportation. That is to say, these skeleton-like structures help cells move from place to place within the body (‘cellular transportation’), but they also aid in the movement of proteins from place to to within the cell (‘intracellular transportation’). On top of this, microtubules also play an important function in cell division.
The stability and maintenance of these microtubles relies on proteins like TAU.
But what is TAU???
TAU is protein that is very abundant in the brain. It is generated from the RNA (the instructions for making protein) of the MAPT gene, located on chromosome 17.
TAU protein is a microtubule-associated protein, which functions by stabilising the highways and byways inside a cell. Basically, these proteins hold together the roads which allows vesicles (the small bags I mentioned above) to be moved around the cell (by transporter proteins like kinesin).

TAU: a stabilising presence. Source: Hindawi
So why is TAU interesting to researchers?
Because TAU is associated with both Parkinson’s disease AND Alzheimer’s disease.
In both conditions there is a build up of TAU protein, which accumulates and clusters (or ‘aggregates’) in a similar fashion to our old friend the Parkinson’s disease-associated protein alpha synuclein (Click here for a good review article on this topic).
Tau protein in Alzheimer’s disease. Source: Dreamstime
And an association between TAU and other neurodegenerative conditions has recently been highlighted:

Title: Presence of tau pathology within foetal neural allografts in patients with Huntington’s andParkinson’s disease.
Authors: Cisbani G, Maxan A, Kordower JH, Planel E, Freeman TB, Cicchetti F.
Journal: Brain. 2017 Oct 24.
PMID: 29069396
In this study, the researchers conducted a postmortem analysis on the brains of two people with Huntington’s disease that received cell transplants 9 and 12 years before they passed away. And they also looked at sections of brain for two people with Parkinson’s that had received cell transplants 18 months and 16 years before they passed away (due to natural causes). I have previously discussed how alpha synuclein aggregates have been found inside dopamine neurons within cell transplantation grafts in people with Parkinson’s (Click here to read that post), but no one had ever looked at TAU in this context before this report.
Remarkably, when the investigators looked at the localisation of TAU protein in the Huntington’s disease-affected brains, they found aggregated TAU inside the transplanted cells. That is to say, somehow the healthy transplanted cells had taken on one of the pathological features of the Huntington brain. Similarly, the researchers also found TAU protein aggregation in the 16 years transplant in the Parkinson’s brain. Curiously, they did not find any in the 18 month old transplant, suggesting that the clustering of TAU may be a very slow process.
Thus, the idea that alpha synuclein is being passed from cell to cell as Parkinson’s progresses, may also apply to other proteins like TAU.
Methods by which alpha synuclein and TAU may be passed from cell to cell. Source: Openi
And the aggregation of TAU is certainly not unique to Alzheimer’s or Parkinson’s. And there is a lot of research now indicating that TAU is possibly involved in other neurodegenerative conditions, such as amyotrophic lateral sclerosis (ALS; motor neuron disease; Click here to read more on this) and multiple sclerosis (Click here to read more on this).
Ok, so TAU may be involved with all neurodegenerative diseases?
Perhaps.
This is still being investigated though. And there is evidence to suggest that TAU protein levels increase naturally in the ageing brain (Source).
But TAU appears to be different in the case of Parkinson’s.
Different? How so?
Back in 2010, this research report was published:

Title: Elevated tauopathy and alpha-synuclein pathology in postmortem Parkinson’s disease brains with and without dementia.
Authors: Wills J, Jones J, Haggerty T, Duka V, Joyce JN, Sidhu A.
Journal: Exp Neurol. 2010 Sep;225(1):210-8
PMID: 20599975 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers wanted to investigate where in the postmortem brain TAU aggregates could be found. They compared brains from people who passed away with Parkinson’s and Parkinson’s with dementia (PDD) with healthy control brains. They found that in both Parkinson’s and PDD, alpha synuclein levels in the brain were high, especially in PDD which had persistently higher levels than Parkinson’s brain across all brain regions analysed.
Interestingly, however, higher levels of TAU aggregation were only found in the striatum of the Parkinson’s and PDD brains, when the brains were compared with healthy control samples.
The researchers were unable to detect any high levels of TAU aggregates in other regions of the brains that they looked at, in either the Parkinson’s or PDD brains despite observing the increased levels of alpha synuclein. And this result is very different from brains affected by Alzheimer’s disease, where high levels of TAU aggregation are more global – observed in many different brain regions. The investigators concluded that their “data demonstrates restricted expression of tauopathy in brains of PD and PDD, probably limited to dopaminergic neurons of the nigrostriatal region” (the nigrostriatal region being the substantia nigra – where the dopamine neurons reside – and the striatum – where the dopamine neurons release the bulk of their dopamine).
And a more recent research report has indicated similar sorts of differences between Alzheimer’s, Parkinson’s and PDD (Click here to read that report).
Do alpha synuclein and TAU protein interact?
There does appear to be some ‘co-localisation’ (both being in the same location) of alpha synuclein and TAU protein in the Parkinsonian brain:

Title: Colocalization of tau and alpha-synuclein epitopes in Lewy bodies
Authors: Ishizawa T, Mattila P, Davies P, Wang D, Dickson DW.
Journal: J Neuropathol Exp Neurol. 2003 Apr;62(4):389-97.
PMID: 12722831
In this study, the researchers analysed postmortem brains of people who passed away with Parkinson’s. The researchers compared where alpha synuclein and TAU were located. They found that TAU staining was present in Lewy bodies – dense circular clusters of protein that are characteristic of the Parkinsonian brain – in 80% of the cases, irrespective of the stage of Parkinson’s (recently diagnosed or long term sufferer). And in most cases, TAU was located at the periphery of the Lewy body, not in the core (similar to alpha synuclein).
TAU (Brown) staining around the edge of a Lewy body (LB). Source: Tremorjournal
Interestingly, the investigators found that the proportion of Lewy bodies with TAU protein inside them was highest in the neurons that are most vulnerable to Parkinson’s (such as those in the locus ceruleus and basal nucleus of Meynert – two regions in the brain that are badly affected by Parkinson’s), and lowest in neurons that demonstrate resistance to Parkinson’s.
And in addition to this study, there has been some research that suggests that TAU and alpha synuclein actually interact, forming a dangerous pair with regards to neurodegeneration:
Title: Interactions between Tau and α-synuclein augment neurotoxicity in a Drosophila model ofParkinson’s disease.
Authors: Roy B, Jackson GR.
Journal: Hum Mol Genet. 2014 Jun 1;23(11):3008-23.
PMID: 24430504 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers used genetically engineered flies to look at the effect of combining TAU and alpha synuclein. They found that producing high levels of human alpha synuclein in flies had no effect (compared to non-engineered control flies) when looking at the eyes of the flies. But when the researchers caused high levels of human TAU protein in flies, it resulted in smaller eyes.
The interesting result, however, came when the researchers engineered flies that produce high levels of both of the two proteins. The eyes were smaller and the surface of the eye was rougher than the TAU alone flies (see image below).
Fly eyes. Source: Ncbi
The researchers also assessed the motor performance of flies (their ability to fly), and again they found that producing high levels of human alpha synuclein in flies had no effect on flying ability (compared to non-engineered control flies). On the other hand, flies producing high levels of TAU had severe motor deficits – with an approximately 67% decrease in ability compared to the control flies). This motor behaviour was even further impaired (88% reduction) when high levels of both TAU and alpha synuclein were present in flies.
Interesting. Are there any genetic variants that increase the risk of developing Parkinson’s?
Before reading any further, can I recommend that readers unfamiliar with the genetics of Parkinson’s have a look at our genetics of Parkinson’s page.
The gene from which TAU is produced (called MAPT) is not considered a PARK gene. Since the first mutations in this gene were discovered in 1998, however, over 40 genetic variants in the MAPT gene have been associated with increased risk of developing certain neurodegenerative conditions.
There has been an association made with Parkinson’s disease though:

Title: Tau acts as an independent genetic risk factor in pathologically proven PD.
Authors: Charlesworth G, Gandhi S, Bras JM, Barker RA, Burn DJ, Chinnery PF, Gentleman SM, Guerreiro R, Hardy J, Holton JL, Lees A, Morrison K, Sheerin UM, Williams N, Morris H, Revesz T, Wood NW.
Journal: Neurobiol Aging. 2012 Apr;33(4):838.e7-11.
PMID: 22221882 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers wanted to assess whether genetic variations in the MAPT gene (which produces TAU) were associated with increased risk of Parkinson’s. They had previously found such an association, but that particular study there were questions about whether some of the cases of ‘Parkinson’s’ were actually cases of ‘Progressive supranuclear palsy’ (or PSP) which is very similar to Parkinson’s (Click here to see that previous study). The researchers wanted to eliminate the possibility of any PSP “contamination” in their data set.
So they analysed DNA from 385 cases of neuropathologically proven Parkinson’s disease (meaning that pathologist had assessed the brains at the postmortem stage and given a diagnosis of Parkinson’s). This group included 245 males and 140 female, and genetic analysis of the MAPT gene demonstrated statistically significant associations in the 8 individual variations across the MAPT gene with Parkinson’s. This result suggests that genetic mutations within the MAPT gene are influential in the development of Parkinson’s.
And then there is the other very strange feature of the MAPT gene.
Huh? What strange feature?
Some of us carry an inverted version of MAPT.
And by that I mean that the MAPT gene on chromosome 17 has actually flipped. It is completely inverted. The change which happened a very long time ago in our evolution occurred via a process called ‘Chromosomal Inversion’. This is a genetic mutation resulting in a portion of a chromosome being in the opposite orientation (inverted).
Source: Yourgenome
In the case of TAU, a stretch of DNA (approximately 900,000 base pairs long) which encompasses the MAPT gene flipped and it present in a lot of the general public.
This inversion has resulted in the what is called the ‘TAU haplotype’.
What is a haplotype?
A haplotype is a set of variations in DNA that are usually inherited together. The genetic variations making up a haplotype can be located in different places on the chromosome but they are inherited together.
Importantly, the concept of haplotype differs from that of ‘genotype’ which refers to a single trait or multiple inherited traits. Critically, a genotype involves alterations to a single gene or combination of genes at a particular locus (a specific position). The genetic material in a haplotype can be at different locations on the chromosome, but for a genotype the genetic material is all at one locus.
So because the TAU region of DNA is inverted, it is considered a haplotype (a change of location) rather than a genotype?
Exactly.
And there are two major haplotypes for TAU called H1 and H2.
H1 is the correct orientation of TAU, while H2 is the inverted form.
Curiously, both haplotypes provide RNA (the instructions) for making TAU protein. But several studies have suggested that the H2 haplotype produces lower levels of TAU protein, and this may have a protective effect in neurodegeneration (Click here to read more about this). More recently, researchers have suggested that there is no difference in the levels of TAU protein between the two haplotypes, but rather the H2 haplotype is associated with an error in some of the TAU RNA (with the introduction of a segment called ‘exon-3’). And it is this error that may be responsible for the reduction in functioning TAU protein.
Either way, the H1 haplotype (with higher levels of functioning TAU protein) is considered to be a genetic risk factor with regards to the severity of many neurodegenerative conditions.
And this effect shows itself in Parkinson’s:
Title: The effect of MAPT haplotype on neocortical Lewy body pathology in Parkinson disease
Authors: Robakis D, Cortes E, Clark LN, Vonsattel JP, Virmani T, Alcalay RN, Crary JF, Levy OA.
Journal: J Neural Transm (Vienna). 2016 Jun;123(6):583-8.
PMID: 27098667 (This research report is OPEN ACCESS if you would like to read it)
In this study, the researchers looked at Lewy bodies in the postmortem brains of 71 people who passed away with Parkinson’s and 52 control brains. When they also took into account the TAU haplotype of the individuals, the investigators found an interesting result: the Parkinsonian brains with two copies of the H1 haplotype (in other words, both copies of the MAPT gene – one from each parent – were normal and NOT inverted) had a higher burden (or number) of Lewy bodies than the H2 haplotype.
It should be noted that while that H1 haplotype may cause more severe forms of Parkinson’s, it also appears to cause more severe forms of other neurodegenerative conditions (Click here to read more about this).
Interesting. Can we do brain scans for TAU?
Yes we can:
Title: Tau Positron Emission Tomographic Imaging in the Lewy Body Diseases.
Authors: Gomperts SN, Locascio JJ, Makaretz SJ, Schultz A, Caso C, Vasdev N, Sperling R, Growdon JH, Dickerson BC, Johnson K.
Journal: JAMA Neurol. 2016 Nov 1;73(11):1334-1341.
PMID: 27654968 (This article is OPEN ACCESS if you would like to read it)
In this study, the researchers wanted to compare TAU aggregation in folks with Lewy body dementia, cognitively impaired Parkinson’s (PD-impaired), cognitively normal Parkinson’s (PD-normal), and normal healthy control subjects. But critically, they wanted to do this in live subjects. In order to do this, they used a technique called Positron-emission tomography (or PET) brain imaging, which allows one to visualise the activity of specific activity in the human in real time. Many people with Parkinson’s will have had a ‘DAT-Scan’ which provides an bird’s eye image of dopamine activity in the brain (see image below). Subjects are injected with a radioactive solution that labels a channel on the surface of cells which regulates the re-absorption of dopamine. If there are less dopamine neurons, there will be less of these channels to label.
An example of a DAT-Scan. Source: Cedars-sinai
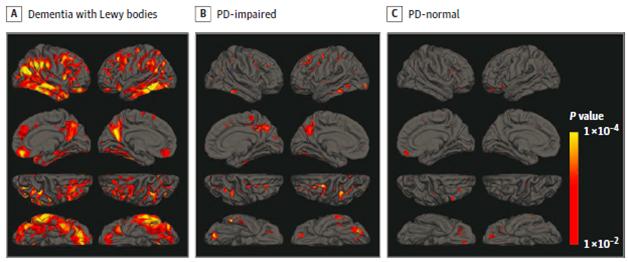
In this new study, however, the researchers used a radioactive solution that labelled aggregated TAU protein (the solution is called [18F]AV-1451 – catchy name, huh?). This solution allowed the investigators to visual in real time the aggregation of TAU. What they found was that in the cortical regions of the brain, there was a lot more aggregated TAU in subjects with Lewy body dementia than cognitively impaired Parkinson’s subjects and cognitively normal Parkinson’s subjects (see image below).
Source: Ncbi
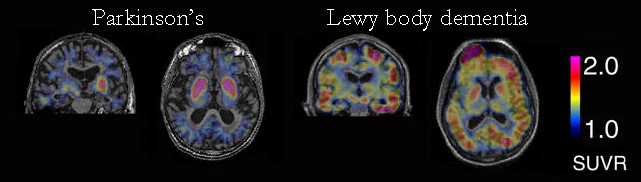
One interesting detail in the study was the high level of TAU aggregation in the striatum of the Parkinson’s subjects (see image below). As discussed above, higher levels of TAU aggregation were only found in the striatum of postmortem Parkinson’s brains, and we see the same result here. In the image below, the highest levels of aggregated TAU (as determined by red coloration), can be seen in just two spots in the Parkinson’s brain on the left. These two red spots are the striatum. Compare that result with the global presence of aggregated TAU in the Lewy body dementia subject on the right.
Source: Ncbi
This imaging technique will be very useful in clinical trials looking at TAU.
Have there been any clinical trials targeting TAU?
Yes, but not for Parkinson’s (that I’m aware of).
Drugs targeting TAU have been assessed in different types of dementia…. but thus far, not with much success.
A good example was TauRx Pharmaceuticals, who conducted a large phase III trial of their drug TRx0237 in frontotemporal dementia (a form of neurodegeneration similar to Alzheimer’s). TRx0237 is a compound that inhibits the aggregation of TAU.
Source: TauRx Pharmaceuticals
The researchers enrolled 221 people with frontotemporal dementia (as determined by MRI brain imaging). They were primarily Caucasian, males with an average age of 63. Half the participants took 100 mg of TRx0237 twice daily, while the other half took a 4 mg TRx0237 pill twice daily as a placebo. Kind of a strange placebo I agree, but because TRx0237 turns urine blue, the researchers used a low dose of 4 mg of TRx0237 in the placebo in order to keep the participants blind to their treatment status.
Participants underwent clinical, cognitive, and motor assessments at 16, 32, and 52 weeks, but on every measure, rates of decline were identical in the treatment and placebo groups at the end of the clinical trial.
So developing drugs that target TAU are a waste of time then?
No, I wouldn’t say that.
This negative result may simply mean that TAU targeting drugs like TRx0237 are not working as a ‘monotherapy’ (or a single, stand-alone treatment). Perhaps it needs to be administered in combination with another drug targeting another protein. Maybe targeting TAU alone is not enough.
What do you mean?
There is currently a drug called PRX002 which is being clinically tested for Parkinson’s by a company called Prothena.
This drug targets a toxic form of alpha synuclein. It removes this protein as it is passed between cells and it is hoped that this will slow down the gradual spread of the condition (Click here to read more about this).
In a worst case scenerio, if the Prothena PRX002 approach is found to not be effective by itself in the current clinical trials, it may be interesting to test it in combination with a drug which also targets TAU (like TRx0237). Perhaps a combination of drugs targeting both alpha synuclein and TAU will be effective.
But let’s worry about that situation if and when we get to it. Until then, fingers are crossed that PRX002 actually works as a monotherapy.
What does it all mean?
I have long worried that the ‘cult of alpha synuclein’ may be taking us in the wrong direction (I’m going to be discussing this in an up coming post). It has focused a great deal of research on just one gene/protein. And in some cases I have feared that some researchers may be seeing what they want to see or – worse – results that may not be disease relevant (for example, by producing very high/toxic levels of alpha synuclein in cells in culture they see cell death which may actually have no association with Parkinson’s what-so-ever). There are most certainly other proteins at play in Parkinson’s, and by focusing on just the one we may be taking the very long route to fully understanding the condition.
The purpose of this post was to provide an overview for readers of another protein – TAU – and how it is associated with Parkinson’s. TAU is an interesting protein in that it appears to play a role in many other neurodegenerative conditions. Given that TAU protein aggregation is associated with so many other neurodegenerative conditions, I wonder if a better understanding of this protein’s functions would be more enlightening.
It is certainly something to meditate on.
Speaking of which, I’m off to find and follow the TAO.
The banner for today’s post was sourced from picturequotes.













An exceptional explanation of TAU and its role in PD; I’m most grateful (and have been stuck on the A-SYN train, admittedly!), Simon. This is a keeper!
LikeLike
Glad you liked it Lisa! I hope all is well.
Simon
LikeLike
I think it’s tragic how difficult it is to maintain open sharing between researchers, doctors, patients, and pharma companies, and the fact that some researchers may be focusing on one element too much is not surprising. I honestly believe there are “cocktails” of treatments available today, but getting the disparate research together and congealing a medical community around such a difficult concept is all but impossible.
Thanks for another great article!
LikeLike
Hi Joe,
You’re very welcome! Glad you liked it. But don’t despair, there is certainly acknowledgement from the PD research community that the situation is probably more complicated than just one protein. And this idea is now being investigated by many groups.
Alpha synuclein was the first genetic risk factor to be discovered for PD (20 years ago this year), and people with elevated levels of the protein were found to have a higher risk of developing PD, so it made sense that researchers would focus on it – following where the data is pointing. Tau seems to be a risk factor for a wider range of conditions, so more research on this protein may have wider implications.
Kind regards,
Simon
LikeLike
simon
most interesting; now that i have a diagnosis of PSP which as you will know is predominantly involving the TAU protein. I this exclusive or does the alpha synuclein play a part too?
kind regards
Keith
LikeLike