|
# # # # Neuromodulation of specific circuits in the brain represents a means of adjusting deficits in neural performance and significantly improving quality of life. Deep brain stimulation has been widely applied to the treatment of Parkinson’s since Alim Benabid first discovered that electrical stimulation of the basal ganglia improves the symptoms of the condition in the late 1980s. Now researchers are attempting to refine the approach further with new technology (such as optogenetics) and more specific targeting – stimulating only particular types of neurons – with impressive results and potentially immediate implications for treatment. In today’s post, we will discuss what optogenetics is, review some new preclinical results, and explore those potentially immediate implications for the treatment of Parkinson’s. # # # # |
 Vienna. Source: Worldofcruising
Vienna. Source: Worldofcruising
In 2016, I was lucky enough to be at the “Dopamine” research conference in Vienna (Austria).
It is a wonderful city, the late summer weather was perfect, and an amazing collection of brilliant researchers had gathered to focus on all things dopamine-related for four days. The conference highlighted all the exciting new research being done on this chemical.
 Source: Medium
Source: Medium
There was – of course – a lots of research being presented on Parkinson’s disease as well, given that dopamine plays such a fundamental role in the condition.
And I was sitting in the lecture presentations, listening to all these new results being discussed, thinking how fantastic it all was, when a researcher from Carnegie Mellon University stood up and (without exaggeration) completely – blew – my – mind!
 Basically sums my reaction. Source: Canacopegdl
Basically sums my reaction. Source: Canacopegdl
Seriously. I was left speechless by the results presented.
Wow, what were the results???
The researcher’s name is Aryn H. Gittis:
And her research group investigates the neural circuits underlying the regulation of movement, learning, motivation, and reward.
And the ‘mind blowing‘ research that she presented in Vienna was later published soon after the conference in the scientific journal “Nature Neuroscience”:

Title: Cell-specific pallidal intervention induces long-lasting motor recovery in dopamine-depleted mice
Authors: Mastro KJ, Zitelli KT, Willard AM, Leblanc KH, Kravitz AV & Gittis AH
Journal: Nature Neuroscience (2017) doi:10.1038/nn.4559
PMID:28481350 (This report is OPEN ACCESS if you would like to read it)
In this report, Dr Gittis and her colleagues demonstrated that elevating the activity of one particular type of cell – in an area of the brain called the globus pallidus – could provide long lasting relief from Parkinson’s-like motor features in mice.
Hang on a second. What is the globus pallidus?
The globus pallidus is a structure deep in the brain and before Dr Gittis and her colleagues published their research, we already knew it played an important role in our ability to move.
Movement is believed to be largely controlled by the activity in a specific group of brain regions, collectively known as the ‘Basal ganglia‘.

The basal ganglia structures (blue) in the human brain. Source: iKnowledge
But while the basal ganglia controls movement, it is not the starting point for the movement process.
The prefrontal cortex is where we do most of our ‘thinking’. It is the part of the brain that makes decisions with regards to many of our actions, particularly voluntary movement. It is involved in what we call ‘executive functions’. It is the green area in the image below.

Areas of the cortex. Source: Rasmussenanders
When the prefrontal cortex decides that the left hand should start to play the piano, it will communicate this idea with the premotor cortex (the blue area in the image above) and together they will send a very excited signal down into the basal ganglia for it to be considered. Now in this scenario it might help to think of the cortex as hyperactive toddlers, and the basal ganglia as the governing parental figure. The toddlers are all making demands/proposals and sending mixed messages, and it is for the inhibiting basal ganglia to gain control and determine which is the best.
So the basal ganglia receives signals from the cortex, processes that information before sending a signal on to another important participant in the regulation of movement: the thalamus.

A brain scan illustrating the location of the thalamus in the human brain. Source: Wikipedia
The thalamus (from Greek origins, meaning “chamber”) is a structure deep inside the brain that acts like the central control unit of the brain. Almost all of the sensory information coming into the brain from the spinal cord, passes through the thalamus. And everything leaving the brain, passes through the thalamus. It is aware of most everything that is going on and it plays an important role in the regulation of movement. If the cortex is the toddler and the basal ganglia is the parent, then the thalamus is the ultimate policeman. The high court judge if you like.
Now to complicate things for you, the processing of movement in the basal ganglia involves a direct pathway and an indirect pathway. In the simplest terms, the direct pathway encourages movement, while the indirect pathway does the opposite: inhibits it.

Source: Studyblue
The thalamus will receive signals from the two pathways and then determine – based on those signals – whether to send an excitatory or inhibitory message to the primary motor cortex, telling it what to do (‘tell the muscles to play the piano’ or ‘don’t start playing the piano’, respectively). The primary motor cortex is the red stripe in the image below.

The primary motor cortex then sends this structured order down the spinal cord (via the corticospinal pathway) and, all going well, the muscles will do as instructed.

Source: adapted from Pinterest
Now, in Parkinson’s, the motor features (slowness of movement and resting tremor) are associated with a breakdown in the processing of those direct and an indirect pathways. This breakdown results in a stronger signal coming from the indirect pathway – thus inhibiting/slowing movement. This situation is associated with the loss of dopamine in the brain.
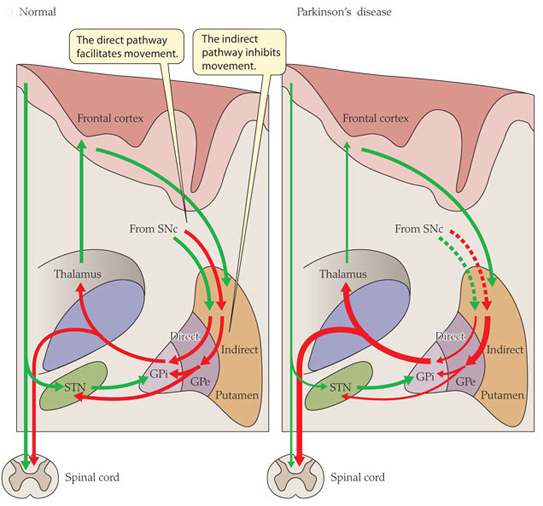
Excitatory signals (green) and inhibitory signals (red) in the basal ganglia, in both a normal brain and one with Parkinson’s disease. Source: Animal Physiology 3rd Edition
Under normal circumstances, dopamine neurons release dopamine in the basal ganglia that helps to mediate the local environment. It acts as a kind of lubricant for movement, the oil in the machine if you like. It helps to reduce the inhibitory bias of the basal ganglia.
Thus, with the loss of dopamine neurons in Parkinson’s, there is an increased amount of activity coming out of the indirect ‘inhibitory’ pathway.
And as a result, the thalamus is kept in an overly inhibited state. With the thalamus subdued, the signal to the motor cortex is unable to work properly. And this is the reason why people with Parkinson’s have trouble initiating movement.

Source: BJP
Now, as you can see from the basic schematic above, the globus pallidus is one of the main conduits of information into the thalamus. Given this pivotal position in the regulation of movement, the globus pallidus has been a region of major research focus for a long time.
It is also one of the sites targeted in ‘deep brain stimulation’ therapy for Parkinson’s (the thalamus being another target).
What exactly does deep brain stimulation mean?
Deep brain stimulation (or DBS) involves placing electrodes deep into the brain to help regulate activity with patterns of short electrical pulses.

DBS in the globus pallidus. Source: APS
By regulating the level of activity in the globus pallidus, DBS can help to control the signal being sent to the thalamus, reducing the level of inhibition, and thus alleviating some of the motor-related features of the Parkinson’s.
The dramatic effects (and benefits) of deep brain stimulation can be seen in this video (kindly provided by fellow kiwi Andrew Johnson):
Deep brain stimulation is not perfect, however.
The placing of the electrodes can sometimes be off target, resulting in limited beneficial effects. Plus the tuning of the device can be a bit fiddly in some cases.
A more precise method of controlling the globus pallidus would be ideal.
|
# RECAP #1: The globus pallidus is a region of the brain involved in the control of motor movements, acting as a conduit for information being passed into the thalamus (a major control center). Deep brain stimulation involves the placement of electrical probes in regions like the globus pallidus and patterns of electrical pulses being applied to help modulate the neural activity of the local region. # |
Ok, so the globus pallidus region of the brain is important for movement. Got it. What did Dr Gittis and her colleagues find in their research?
They used a truly amazing piece of technology called ‘optogenetics‘ to specifically determine which group of cells in the globus pallidus are involved in the inhibitory signals going to the thalamus.
And as I mentioned above their results were VERY interesting.
But what is optogenetics?
Good question.
The short answer: Magic.
The long answer: In 1979, Nobel laureate Francis Crick suggested that one of the major challenge facing the study of the brain was the need to control one type of cell in the brain while leaving others unaltered.

The DNA duo: Francis Crick (left) and James Watson. Source: CNN
Electrical stimulation cannot address this challenge because electrodes stimulate everything in the immediate vicinity without distinction. In addition the signals from electrodes lack precision; they cannot turn on/off neurons as dynamically as we require. The same problems (and more) apply to the use of drugs.
But Crick thought that he had a solution. He speculated that the answer might be light.
How on earth would you do that?
Well, in 1971 – eight years before Crick considered the problem – two researchers, Walther Stoeckenius and Dieter Oesterhelt, discovered a protein, bacteriorhodopsin, which acts as an ion pump on the surface of a cell membrane. Amazingly, this protein can briefly become activated by green light.
It is a rather remarkable property.
Later, other groups found similar proteins. One such protein, called ‘Channelrhodopsin’, was discovered in green algae (click here to read more on this). When stimulated by particular frequencies of light, these channels open up on the cell surface and allow ions to pass through. If enough channels open, this process can stimulate particular activity in the cell.

Channelrhodopsin. Source: Openoptogenetics
Interesting, but how does this apply to activity in the brain?
This is Karl Deisseroff:

Karl Deisseroff. Source: Ozy
Looks like the mad scientist type, right? Well, remember his name, because this guy is fast heading for a Nobel prize.
He’s awesome!
He is the D. H. Chen Professor of Bioengineering and of Psychiatry and Behavioral Sciences at Stanford University. And he is one of the leading researchers in a field that he basically started.
Back in 2005, he and his collaborators published this research report:
 Title: Millisecond-timescale, genetically targeted optical control of neural activity
Title: Millisecond-timescale, genetically targeted optical control of neural activity
Authors: Boyden ES, Zhang F, Bamberg E, Nagel G, Deisseroth K.
Journal: Nat Neurosci. 2005 Sep;8(9):1263-8. Epub 2005 Aug 14.
PMID: 16116447
In this research report, Deisseroth and his colleagues (particularly Ed Boyden, lead author and now a professor of Biological Engineering at the McGovern Institute for Brain Research at MIT) took the short section of DNA that provides the instructions for making Channelrhodopsin from green algae and they put that piece of DNA into neurons.
And when they then shined blue light on the neurons, guess what happened? Yes, the neurons became activated – that is to say, they produced an ‘action potential’ – an impulse of electrical activity that helps information to be passed from one neuron to another.
Basically: light activated brain activity.
Like I said ‘Magic’!

Source: Sqonline
And the best part of this biological manipulation was that Deisseroth and his colleagues could activate the neurons with absolutely amazing precision! By pulsing light on the cells for just millisecond periods, they could elicit instant action potentials:

Precise control of the firing of a neuron. Source: Frontiers
And of course any surrounding cells that do not have the Channelrhodopsin DNA were not affected by the light, but were activated by the signal coming from the Channelrhodopsin+ cells.
This original research report lead to a gold rush-like search for other proteins that are light activated, and we now have an ever increasing toolbox of new proteins with curious properties. For example, we can now not only turn on neurons, but we also have proteins that can shut their activity down, blocking any action potentials (with proteins called ‘Halorhodopsin’ – click here for more on this). And many of these proteins are activated by different frequencies of light. It is really remarkable biology.

Source: Harvard
Click here for an excellent first-hand history of the early development of optogenetics (written by Ed Boydon who worked with Diesseroff on the first optogenetics study).
Two years after the first report of optogenetics, the first research demonstrating the use of this technology in the brain of a live animal was published (Click here and here to read more on this). And these fantastic tools are not just being used in the brain, they are being applied to tissues all over the body (for example, optogenetics can be used to make heart cells beat – click here to read more on this).
This TED talk video of Ed Boyden’s description of optogenetics is worth watching if you want to better understand the technique and to learn more about it:
Very interesting, so Dr Gittis and her colleagues used optogenetics in their research. What did they find?
Well, from previous research the team knew that there were two types of neurons in the globus pallidus that regulate a lot of the activity in this region. Those two types were identifiable by two different proteins:
- Lim homeobox 6 (Lhx6)
- Parvalbumin (PV).
The Lhx6 neurons, which do not have any PV protein, are generally concentrated in the medial portion of the globus pallidus (closer to the centre of the brain), and they have strong connections with the striatum and substantia nigra parts of the brain (two regions associated with Parkinson’s and dopamine activity). The PV neurons, on the other hand, are more concentrated in the lateral portions of the globus pallidus (closer to the side of the brain), and they have strong connections with the thalamus (Click here to read this previous research).
In their new research report, Dr Gittis and her colleagues have used optogenetics to determine the functions of these two types of cells in the globus pallidus.
Initially, they stimulated both Lhx6 and PV neurons at the same time to see if they could restore movement in mice that had been treated with a neurotoxin (6-OHDA) that killed all the dopamine neurons.
Unfortunately, they saw no rescue of the motor abilities of the mice.
Next, they shifted their attention to activating the two groups of cells separately to see if one of them was inhibiting the other. And when they stimulated the PV neurons alone, something amazing happened: the mice basically got up and started moving around like normal.
But the really mind blowing part of this research – and this was my:
moment at the dopamine conference in Vienna – was that even after the researchers turned off the stimulating light (so no more artificial stimulation of the cells) the mice were still able to keep moving around.
 Stimulation of the PV neurons. Source: PMC
Stimulation of the PV neurons. Source: PMC
In the image above, the grey line represents control mice and the red line is the PV stimulated mice. As you can see with repetitive stimulation (illustrated by the light blue lines), the time spent immobile becomes less and less in the PV stimulated group, while the control group remains still.
…
…
Mind not blown yet?
How about this: The effect lasted for several hours after they turned off the stimulation!
 Stimulation of the PV neurons. Source: PMC
Stimulation of the PV neurons. Source: PMC
In the image above, after the light pulse stimulation period (the light blue line), the PV stimulated group of mice (red line) remain mobile 75% of the time (compared to a functional control group (purple line) who had their D1-spiny projection neurons stimulated). Note that the red line remains stable across 3-4 hours (indicating movement).
Surely that is mind blowing.
That must make you feel a little:
Or am I the only one impressed by this?
How on Earth are those mice still moving around with no stimulation?!?
Next, the investigators tested the reverse experiment: inhibiting the Lhx6 neurons.
And guess what?
They found that by inhibiting the Lhx6 neurons with pulses of light, they could restore movement in the dopamine-depleted mice (and again for hours beyond stimulation – note the blue line in the image below remains even after the light pulses – green lines – have stopped).

Inhibiting of the Lhx6 neurons. Source: PMC
These results further blew my mind at the conference in Vienna. And even now as I write this, I am still….well, flabbergasted! (there’s a good word).
In addition to being a very elegant experiment and use of this new optogenetic technology, this study opens new doors for us in the Parkinson’s research field regarding our understanding of how movement works and how we can now potentially treat PD.
|
# # RECAP #2: Optogenetics is a technique that allows for the controlled stimulation of cell activity (or inhibition) using light. Using optogenetics, researchers have determined a specific type of cell in the globus pallidus that allows for Parkinsonian mice to be more mobile, and the effect of the stimulation can last several hours after the application of light has stopped. # # |
I will admit the result is impressive. How have the researchers followed up their findings?
Well, that study was published in 2017. And Dr Gittis and her team were wondering about the translatability of their findings, since optogenics is still a long way from the clinic.
They started questioning whether standard DBS could achieve similar results and that has led to the publication a follow up study last week:
 Title: Population-specific neuromodulation prolongs therapeutic benefits of deep brain stimulation.
Title: Population-specific neuromodulation prolongs therapeutic benefits of deep brain stimulation.
Authors: Spix TA, Nanivadekar S, Toong N, Kaplow IM, Isett BR, Goksen Y, Pfenning AR, Gittis AH.
Journal: Science. 2021 Oct 8;374(6564):201-206.
PMID: 34618556
In this study, the researchers started the investigation using a ‘bottom up’ approach, by making electrical recordings from the Lhx6 neurons and PV neurons in the globus pallidus to better characterise them and see if there were any features that could be used to their advantage. In doing this, they noticed something interesting about the two types of cells: the Lhx6 neurons received proportionately more inhibitory signals than PV neurons.
While the Lhx6 neurons were inhibited by stimulation, the PV neurons were typically excited by it.
Further recordings revealed additional differences, which meant that the researchers could separate out the firing responses of PV neurons from Lhx6 neurons during stimulation with a bit of careful calculation. Basically, they found “a sweet spot” that allowed them to inhibit the Lhx6 neurons while activating the PV neurons using traditional DBS electrical stimulation (rather than optogenetics). It required a particular burst DBS method.
They tested this the new burst DBS protocol in a mouse model of Parkinson’s.
Before stimulation began, the mice in the study were not very mobile. Both the conventional DBS protocol and the new burst DBS method reduced this immobility in the mice, allowing them to move freely around an arena while the DBS stimulation was on.
What happened when the researchers turned off the stimulation?
When the investigators switched off the conventional DBS, the mice quickly returned to an immobile state. But the mice that had been treated with the new burst DBS method continued to move around after the stimulation was turned off. In fact, 5 of the 8 mice in the new burst DBS method group were still moving around 2.5 hours after the stimulation was turned off.
Are you feeling a little:
You should be.
The researchers stated that “on average the therapeutic effects of burst DBS persisted >4.5 times as long as those of conventional DBS“. And they concluded their study by noting that their “burst DBS protocol can be delivered through commonly used DBS implants and falls within US Food and Drug Administration–approved stimulus frequencies, enabling immediate testing in PD models across species, including human patients“.
So this is to be tested in humans?
Yes.
In fact, the investigators are already exploring this with Nestor Tomycz, a neurological surgeon at Pittsburgh’s Allegheny Health Network. They will conduct a randomized, double blind crossover study assessing safety and tolerability in patients with idiopathic Parkinson’s. The participants will be assessed and followed over 12 months (Source). This trial is not yet listed on the ClinicalTrials.gov website (please correct me if I am wrong), so we don’t know all of the details for it yet, but it will be interesting to see if this work translates well.
So what does it all mean?
One of the pleasures of writing these posts is to go back through the previous research and to see the steps that were taken to get to where we are now on some of these topics. Gradually shifting from the identification of a particular subtype of cell in an area of the brain involved in movement to testing their role in mobility. Deciphering patterns of electrical behaviour and then progressing to initiating a clinical trial based on subsequent work. For me it is an evening of reading and learning, but for the scientists doing the research it is decades of dedicated work – sweat, prepared minds, and a little luck.
New research has been published that has provided new insights into our understanding of how our brains allow us to move freely. Scientists at Carnegie Mellon University have identified subtypes of cells in the brain that if modulated in the right way can allow a mouse model of Parkinson’s to move freely – even hours after the modulation has stopped. These novel findings are allowing for the initiation of a clinical trial, which could have immediate impact on how we use technology like deep brain stimulation.
Rather than waiting years to find out if a particular drug works, we could see this research impacting DBS programming in the near future.
Fingers crossed it all continues to go well.
 All of the material on this website is licensed under a
All of the material on this website is licensed under a
Creative Commons Attribution 4.0 International License
You can do whatever you like with it!
The banner for today’s post was sourced from Hopkinsmedicine


this is awesome news…wow
LikeLike