|
Over the last 12 months, the Silverstein Foundation has quickly established itself as a major focused force in the fight against Parkinson’s. And when I say ‘focused’, I mean ‘focused’ – the foundation is “actively pursues and invests in cutting edge research with the goal of discovering new therapies for the treatment of Parkinson’s Disease in glucocerebrosidase (GBA) mutation carriers”. But the output of this effort may well have major benefits for the entire Parkinson’s community. In today’s post, we will discuss what GBA is, how it functions inside cells, its association with Parkinson’s, and what all of this GBA focused research being funded by the Silverstein Foundation could mean for the Parkinson’s community. |
Jonathan Silverstein. Source: Forbes
This is Jonathan Silverstein.
He’s a dude.
He is also a General Partner and a Co-Head of Global Private Equity at OrbiMed – the world’s largest fully dedicated healthcare fund manager. During his time at OrbiMed, the company has invested in healthcare companies that have been involved with over 60 FDA approved products.
In February 2017, he was diagnosed with Parkinson’s disease at just 49 years of age.
Rather than simply accepting this diagnosis, however, Mr Silverstein decided to apply the skills that he has built over a long and successful career in funding biotech technology, and in March 2017, he and his wife, Natalie, set up the Silverstein Foundation.
They raised $6 million from donors and then provided another $10 million of their own money to fund the endeavour, which has funded a dozen research projects and started a new company called Prevail Therapeutics (we’ll come back to this shortly).
Source: Businesswire
The foundation has just one mission: “to actively pursue and invest in cutting edge research with the goal of discovering new therapies for the treatment of Parkinson’s Disease in GBA mutation carriers”
And it seeks to address this by achieving three goals:
- to find a way to halt the progression of Parkinson’s with GBA.
- to identify regenerative approaches to replace the damaged/lost cells
- to find preventative measures
What is ‘GBA’?
GBA is a gene – a section of DNA that provides the instructions for making a particular protein. In the case of the GBA gene, the protein is an enzyme, called Glucocerebrosidase (also known as GCase) .
What does Glucocerebrosidase do?
Glucocerebrosidase helps with the digestion and recycling of certain waste inside cells. The enzyme is located and active inside ‘lysosomes‘.
What are Lysosomes?
Lysosomes are small bags of degradative enzymes – like glucocerebrosidase – that can be found inside of cells.
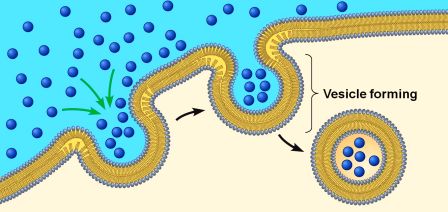
On a continual regular basis, small parts of the external layer of the cell membrane is brought inside the cell. This is a process called endocytosis. It occurs when the cell consumes resources from the outside world in order to find what it needs to function and survive. As a section of cell membrane is brought into the cell, it forms a vesicle (which is a term used to refer to small spherical bags of stuff inside cells). Given the process by which that vesicles was formed, it is referred to as an endosome (sometimes it is also called a vacuole).
Source: Socratic
Once the endosome is inside the cell and detached from the rest of the membrane, it will bind to another vesicle which is called a lysosome. And as I mentioned above, lysosome is a small bag that is full of digestive enzymes, which help to break down the contents of the endosome.

How lysosomes work. Source: Prezi
The lysosome will fuse with the endosome/vacuole and the enzymes from the lysosome will mix with the material in the vacuole and digest it (or it break down into more manageable components).
This enzymatic process works in a very similar fashion to the commercial products that you use for washing your clothes.
Enzymatic degradation. Source: Samvirke
The reagents that you put into the washing machine with your clothes contain a multitude of enzymes, which help to break down the dirty, bacteria, flakes of skin, etc that cling to your clothes. Each enzyme breaks down a particular protein, fat or such like. And this is very similar to the collection of enzymes in the lysosome. All of them are needed to break down all of the contents of the endosome.
And if one of those enzymes – such as glucocerebrosidase – is faulty (due to a mutation in the DNA providing the instructions for its construction), then the enzymatic process is disrupted, which could result in the build up of un-degraded material over time.
OK, so how is Glucocerebrosidase associated with Parkinson’s?
Take a wild guess which gene in your DNA is one of the most commonly affected genes in Parkinson’s?
Approximately 5%–8% of people with Parkinson’s have a genetic mutation in the GBA gene (Click here and here to read more about this). According to the Michael J Fox foundation webpage on GBA “up to 10 percent of people with PD in the United States carry” a genetic variation in the GBA gene.
The GBA gene and mutations associated with Parkinson’s. Source: Neurology
GBA is a very large gene and there are numerous genetic variants spread across its length. The most common mutations are located in positions N370S and L444P. These mutations cause a reduction in the enzymatic activity of the glucocerebrosidase enzyme.
People have two copies of each gene in their DNA (each copy is called an allele), so if one allele doesn’t work properly there is a back up option. Call it mother nature’s insurance policy. But if people have a genetic mutation in one allele of their GBA genes, cells in their body will often produce a normal version of the glucocerebrosidase enzyme and an abnormally short, non-functioning version of the glucocerebrosidase enzyme. In those cases, the breaking down of waste inside the lysosome becomes less efficient. And if waste can not be disposed of or recycled properly, things start to go wrong in the cell.
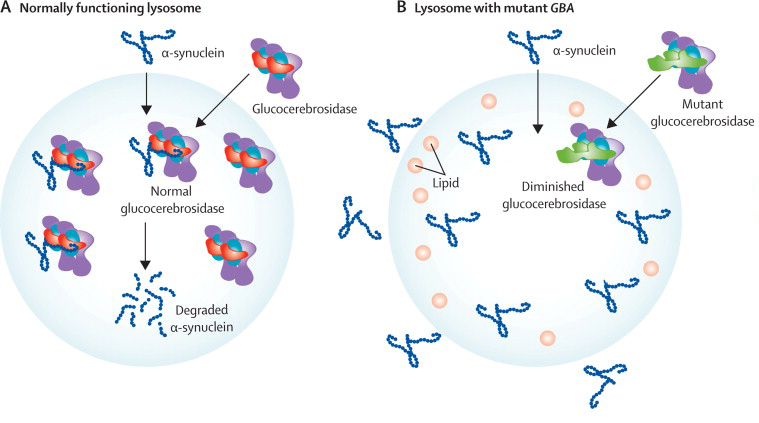
Lysosome function in normal and mutant GBA situations. Source: The Lancet
What impact does a GBA mutation have on someone’s Parkinson’s?
Generally, people with GBA-associated Parkinson’s will exhibit more severe symptoms than people without a GBA mutation, and this has recently been confirmed in a large clinical observation study:
Title: Features of GBA-associated Parkinson’s disease at presentation in the UK Tracking Parkinson’s study.
Authors: Malek N, Weil RS, Bresner C, Lawton MA, Grosset KA, Tan M, Bajaj N, Barker RA, Burn DJ, Foltynie T, Hardy J, Wood NW, Ben-Shlomo Y, Williams NW, Grosset DG, Morris HR; PRoBaND clinical consortium.
Journal: J Neurol Neurosurg Psychiatry. 2018 [Epub ahead of print]
PMID: 29378790 (This article is OPEN ACCESS if you would like to read it)
In this multi-research centre study, the investigators studied 1893 people with Parkinson’s. Of these 48 (2.5%) had one copy of a known GBA mutation, 117 (6.2%) had a non-GBA genetic variant that had previously been associated with Parkinson’s (such as mutations in genes like LRRK2 or Alpha Synuclein), and 28 (1.5%) carried genetic variants of unknown significance in the GBA gene. The most common GBA mutation associated with Parkinson’s is called ‘L444P‘ and this was also the most common GBA mutation observed in this study.
Individuals with Parkinson’s associated GBA mutations were on average diagnosed 5 years earlier compared with non-carriers. They were also more likely to have postural instability and gait difficulties compared with non-carriers. In addition, they had more progressive forms of Parkinson’s (as determined by more advanced Hoehn and Yahr staging – after adjustment for age – compared with non-carriers). Curiously, no differences was observed in cognitive function between GBA mutation carriers and non-carriers. Cognitive impairment/dementia have been reported in other studies at a later stages of the condition (Click here to read more about this). This observation led the researchers to conclude that “this offers an important window of opportunity for potential disease-modifying therapy that may protect against the development of dementia”.
This is really bad, right?
Yes, but this pattern of disease progression in GBA-associated Parkinson’s is not always the case. In fact, 2-3% of the general population will have a Parkinson’s associated GBA mutation in their DNA, but never present any features of Parkinson’s. And then there are cases of identical twins who both have a GBA mutations, but only one of them has developed Parkinson’s (Click here to read more about this).
Thus, the genetics of Parkinson’s is still very complex, and just because a person has a GBA mutation, it does not necessarily mean that they will go on to develop Parkinson’s or necessarily present the aggressive form of the condition. More research is required to increase our understanding of this situation.
OK, so what has the Silverstein Foundation achieved in their first 12 months?
The foundation has recently updated their website, and they have a page time lining their initiatives (Click here to see that page).
Numerous funding grants have been made by the foundation, both to academic research groups as well as commercial biotech companies. For example, in September 2017, they issued two grants to Alector, a Californian-based biotechnology company developing novel immuno-neurology therapies.
Source: Alector
Alector’s research focuses on harnessing the brain’s innate immune cells, the microglia, to counteract the effects of neurodegeneration. Several years ago, genome-wide DNA sequencing studies identified new genetic variants that increase or decrease the chance of developing neurodegenerative conditions. Surprisingly, many of these variants were in immune-system associated genes that are primarily active in the microglia (Click here to read a good review on this topic). This suggested to many researchers that the microglia not only respond to disease, but may also actively help to drive the degeneration. Alector is developing therapies to limit that process.
In January 2018, the Silverstein Foundation also awarded a research grant to resTORbio, a biotech company developing selective inhibitors TORC1.
Source: restorbio
mTOR is a protein that signals via two protein complexes (combination of proteins bound together). These two complexes are known as TORC1 and TORC2.
TORC1 and TORC2. Source: dev.biologists
Now, TORC1 inhibition is associated with lots of good things, such as prolonging lifespan, enhance immune function, enhancing memory, and delaying the onset of age-related conditions in multiple animal models (Click here for a review of this topic). Meanwhile, TORC2 inhibition has been associated with lots of bad stuff (eg. decreased lifespan, worsening memory, etc – Click here for more on this). Thus, the biotech firm resTORbio is trying to inhibit TORC1, without inhibiting TORC2.
And their lead drug candidate, RTB101 – a selective, orally-administered TORC1 inhibitor – is currently being tested in a Phase 2b clinical trial for reducing the incidence of respiratory tract infections (Click here to find out more about that trial). The Silverstein Foundation believes that there could be therapeutic potential for RTB101 in neurodegenerative conditions like Parkinson’s.
What about the company that the Silverstein foundation started?
The company called Prevail Therapeutics.
Source: Businesswire
It was launched by the Silverstein Foundation, REGENXBIO and OrbiMed in July 2017, and the company has entered an exclusive worldwide license agreement with REGENXBIO to develop and commercialise gene therapy approaches for GBA-associated Parkinson’s using REGENXBIO’s gene therapy technology, called NAV AAV vectors.
Source: Regenxbio
Gene therapy involves treating medical conditions with DNA rather than pills. It involves introducing a piece of DNA into a cell which will cause the cell to produce proteins that they usually do not (either by nature or by mutation). The DNA is artificially inserted into cells and the cell’s protein producing machinery does the rest. This introduction of DNA is usually achieved using carefully engineered viruses. The viruses have had all the disease causing components removed, allowing us to use the virus as an efficient biological delivery system. The most common form of virus being proposed for clinical development are adeno associated virus (or AAV).

AAV Viruses. Source: HuffingtonPost
Prevail Therapeutics and REGENXBIO will explore various viral approaches to introducing DNA with a normally functioning copy of the GBA gene into the brain. These efforts may well include the non-invasive gene therapy technology that we have previously discussed on this website (Click here to read more about this).
Virus in the arm, treats the brain. Source: ScienceDirect
Importantly, Prevail Therapeutics is taking on this task with a massive war chest of resources – last week the Silverstein Foundation announced that the company had raised $75 million series A financing (Click here to read the press release). And while large pharmaceutical companies like Pfizer might be pulling out of neurodegenerative research (Click here to read a previous SoPD post on this foolish move), Prevail Therapeutics is attracting the attention and backing of biotech firms that do not have any activity in neuroscience, such as cancer firm Celgene who have put $5 million into the company (Click here to read more about this).
This is fantastic, but will it all work?
This is a difficult question to answer. It all certainly sounds very positive.
But what we do know is this:
Mr Silverstein has a great deal of experience and expertise in the area of biotechnology. He knows the healthcare industry – from drug discovery/development through to the regulation of healthcare – and, more than most, he is aware of the enormous challenge that lies before him.
Despite this, he is very optimistic (Click here, here and here to watch recent interviews with the man) and he appears to have ‘declared war’ on GBA-associated Parkinson’s.
What about the other forms of Parkinson’s?
The stated goals of the Silverstein Foundation are:
- to find a way to halt the progression of Parkinson’s with GBA.
- to identify regenerative approaches to replace the damaged/lost cells
- to find preventative measures
While the first one is specific to GBA associated Parkinson’s, the other two will certainly have benefits for everyone in the Parkinson’s community.
And even though the first goal is focused on GBA, there is a lot to suggest that approaches targeting GBA could have beneficial effects in other forms of Parkinson’s (such as idiopathic PD). In fact, this very idea is currently being tested in a clinical trial in London that we should hear the results of very soon. That trial is testing a clinically available drug called Ambroxol:

Ambroxol. Source: Skinflint
Ambroxol is a commonly used treatment for respiratory diseases (the respiratory system being the lungs and related components required for breathing). Ambroxol promotes the clearance of mucus and eases coughing. It also has anti-inflammatory properties, reducing redness in a sore throat. It is the active ingredient of products like Mucosolvan, Mucobrox, and Mucol.
Researchers believe that Ambroxol could help with Parkinson’s in two ways:
1. Ambroxol is believed to triggers exocytosis of lysosomes (Source). Exocytosis is the process by which waste is exported out of the cell (the opposite of ‘endocytosis’ which we discussed above). Lysosomes are the bags of digestive that rubbish and waste is put into inside a cell for recycling. By encouraging lysosomes to undergo exocytosis and spit their contents out of the cell – digested or not – Ambroxol allows the cell to remove waste effectively and therefore function in a more normal fashion.

Exocytosis. Source: Socratic
2. Ambroxol has been shown to increase levels of the enzyme glucocerebrosidase in the brain (Source).
Thus, by administering Ambroxol to people with Parkinson’s, researchers are hoping to raise levels of the enzyme glucocerebrosidase to help digest proteins and increase the excretion of this waste from cells. This would ideally keep cells healthier for longer and slow down the progression of Parkinson’s.
The clinical trial (named AiM-PD) is a phase IIA Prospective, single-centre, open label clinical trial to evaluate the safety, tolerability and pharmacodynamic effects of Ambroxol in Parkinson’s (Click here to read more about this trial). This trial, which is funded by the Cure Parkinson’s Trust and the Van Andel Research Institute(USA), is being conducted at the Royal Free Hospital in London (UK). It is testing the safety of slowly increasing doses of Ambroxol in Parkinson’s.
The researchers are also looking to see if Ambroxol can increase levels of glucocerebrosidase activity and whether this has any beneficial effects in the subjects. The study has been conducted over a 6 month period, on 20 people with Parkinson’s (critically 10 people with the GBA variant and 10 people with out a GBA mutation – Click here to read more about it).
We are expecting results from the AiM-PD study in 2018.
What does it all mean?
This last week the Silverstein Foundation observed their first anniversary.
The group has been established to focus specifically on finding therapies for a specific genetic form of PD: GBA-associated Parkinson’s.
It is fair to say that few other non-profit organisations focused on a specific medical condition have achieved as much as they have in just their first 12 months of operations. There is a lot to admire in this story – proactively confronting a diagnosis, deploying personal financial resources, laser-like focus, and laying out ambitious plans of attack – and here at the SoPD we will be checking in on the Foundation to see how they are progressing. It will be interesting to see how much things have changed in another 12 months.
Fingers crossed all goes well.
EDITOR’S NOTE: This post includes several publicly traded companies. That said, the material presented on this page should under no circumstances be considered financial advice. Any actions taken by the reader based on reading this material is the sole responsibility of the reader. Neither the Silverstein Foundation or any of the companies mentioned in this post have requested that this material be produced, nor has the author had any contact with these companies (or any associated parties), beyond highlighting their news on social media (see the SoPD Twitter feed). This post has been produced solely for educational purposes.
The banner for today’s post was sourced from the Silverstein foundation













You’re so interesting! I do not believe I have read through anything like that before.
So nice to discover somebody with some genuine thoughts on this topic.
Really.. many thanks for starting this up. This web site is
something that’s needed on the web, someone with a bit of
originality!
LikeLike
I discovered Ambroxol by accident, I was giving my husband Mucinex for congestion and he seemed to be thinking better. I put Musinex and Parkingsons in the computer and came up with Ambroxol. I also saw it was a repourposed drug without side effects and under clinical trials for Parkinsons. I ordered some capsules from Germany because it isn’t sold in the United States but is an over the counter drug. He’s been taking it for a year, what a difference. i don’t think we would have had this year without it. I have had to up the dose to 4 to keep his congestion under control. The clinical trials I’ve looked at have been well over that amount. His doctor is aware of what I’m doing.
LikeLike
Hi Sharon,
Thanks for the interesting comment and for sharing news about Ambroxol. Very interesting that your husband has responded to it. This is great news for you and raises hope for the ongoing clinical trial that we should be hearing the results of shortly. When you say ‘what a difference’, what exactly do you mean? Are there particular aspects of his Parkinson’s that are markedly improved compared to others? Without having you share too much, I would be interested to learn more.
Kind regards,
Simon
LikeLike